AARP Hearing Center


Even though you can sign up for Medicare during your initial enrollment period around your 65th birthday, you may decide to delay signing up without penalty if you or your spouse still work and you have health insurance through an employer.
You may choose to sign up at 65 for Medicare Part A, which covers hospitalization, because it’s premium-free as long as you or your spouse paid Medicare taxes for at least 10 years.
However, you might delay enrolling in Medicare Part B, which covers doctor and outpatient services and costs $174.70 a month for most people in 2024. High earners pay more. You or your spouse will typically need to work for an employer with 20 or more employees to delay signing up for Medicare without coverage gaps.
How a special enrollment period works
When your job-based insurance ends, you’ll qualify for a Medicare special enrollment period. Sign up before your coverage ends or within eight months of losing the insurance to avoid a late enrollment penalty.
Other coverage decisions: You’ll also need to make decisions about other types of coverage when you enroll in Medicare, including Part D prescription drug coverage and Medicare supplement insurance, better known as Medigap, to help pay Medicare’s deductibles and copayments.
Or you may decide to get a private Medicare Advantage plan that provides health and drug coverage. You must have Medicare Part A and Part B before you can enroll in Medigap or Medicare Advantage.
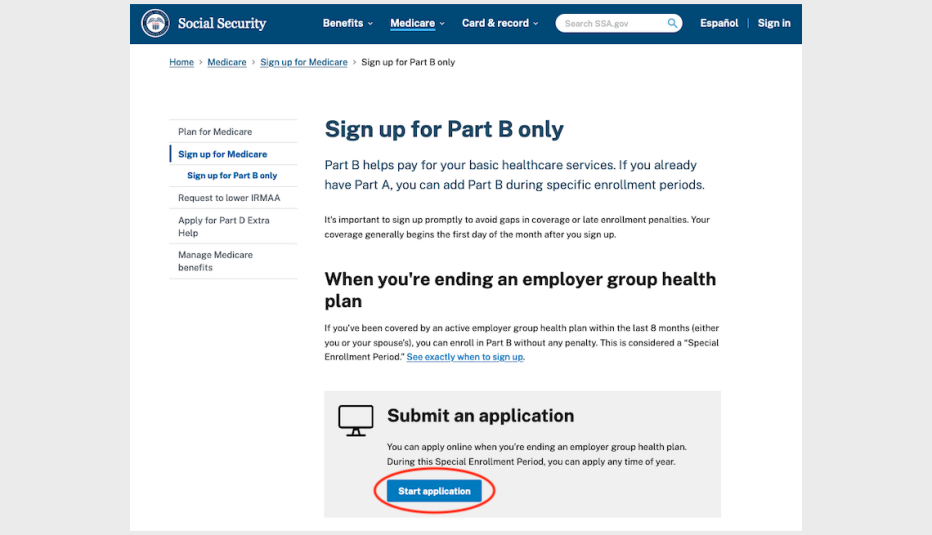
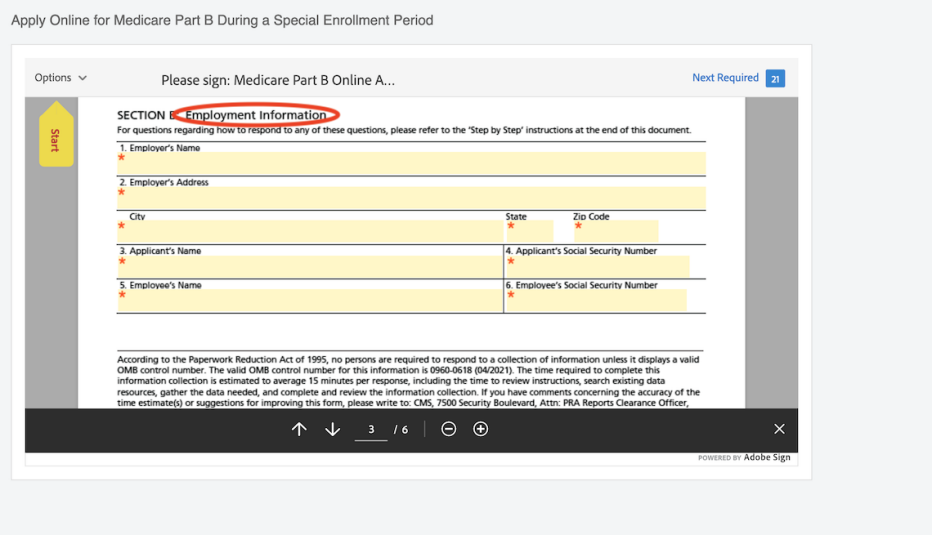
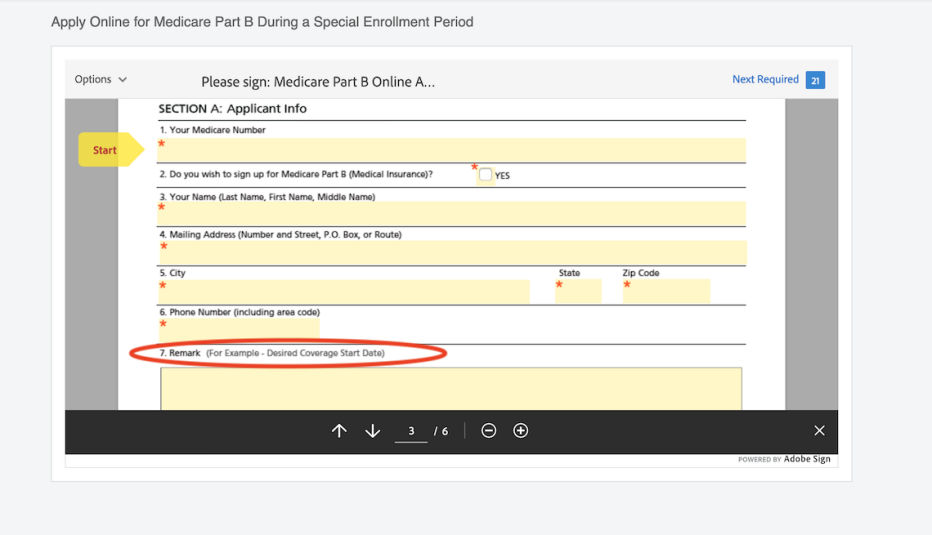
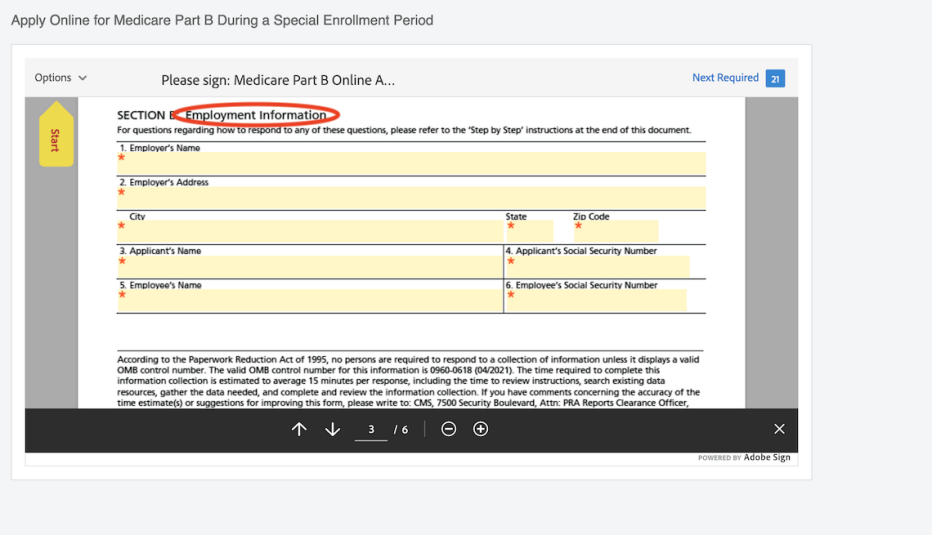
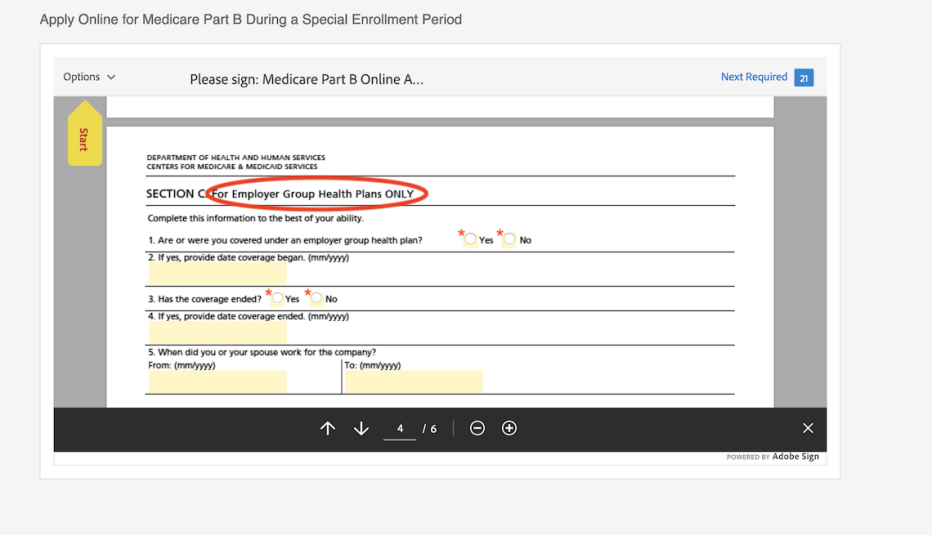
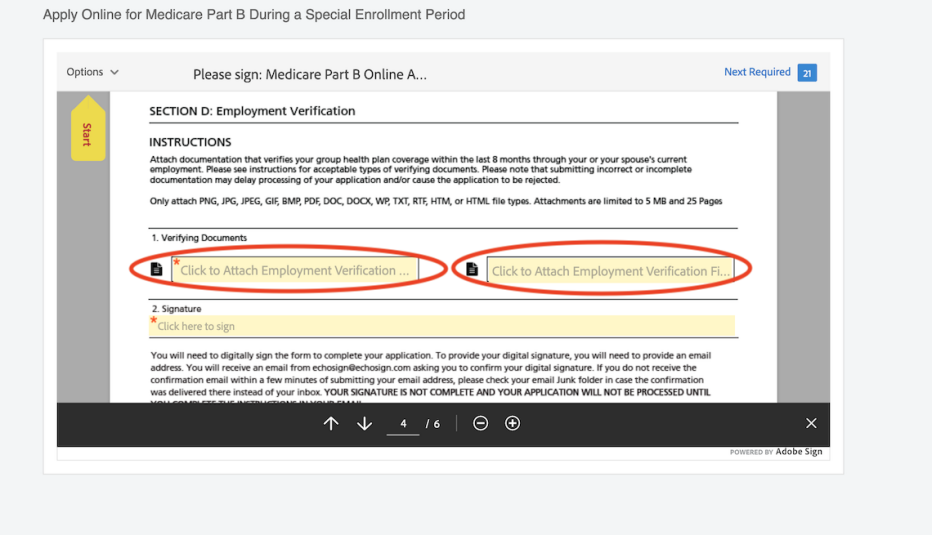
11 steps to enroll online in Part B during a SEP
The steps to sign up for Medicare Part B during a special enrollment period are different than they are during your initial enrollment period at 65.




































































Next in Series
Your Options for Medicare Enrollment After 65
You have options, but you can’t enroll whenever you want