Staying Fit
The lungs are ground zero for COVID-19, making underlying respiratory problems a dire concern.
With chronic obstructive pulmonary disease (COPD) in particular, irreversible changes occur in the lungs’ small airways and alveoli — the tiny air sacs at the end of the airway branches where oxygen is delivered to the body and the waste product, carbon dioxide, is removed. As a result of these changes, the number of air sacs can decrease markedly, potentially making the effects of the coronavirus worse.


AARP Membership— $12 for your first year when you sign up for Automatic Renewal
Get instant access to members-only products and hundreds of discounts, a free second membership, and a subscription to AARP the Magazine.
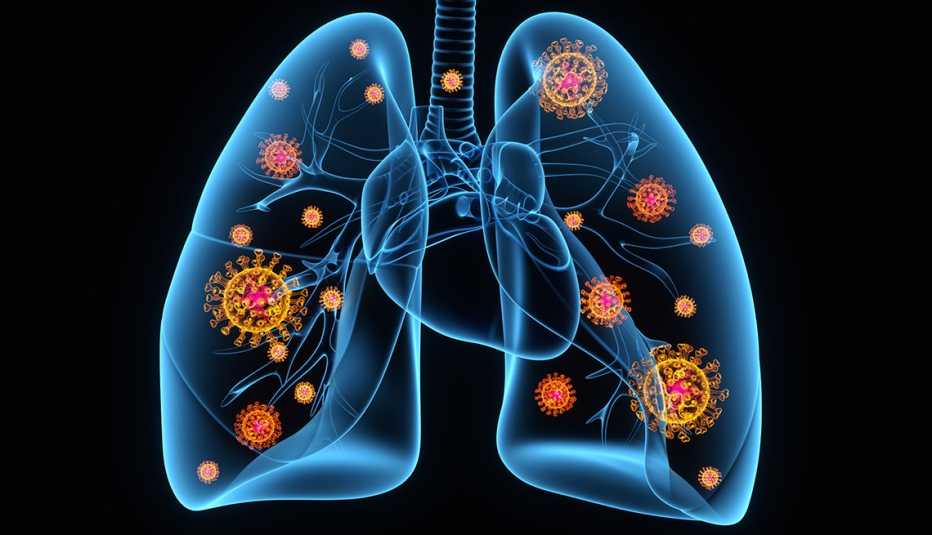
In severe cases of COVID-19, a patchy, diffuse pneumonia develops, causing the air sacs to fill with fluid, preventing oxygen from crossing into the body. “If there is already a decreased number of air sacs due to COPD, the problem is compounded, increasing the chance for respiratory failure and the need for assisted ventilation with a ventilator,” says Neil Schachter, M.D., a professor specializing in pulmonary medicine at the Icahn School of Medicine at Mount Sinai Health System in New York City.
“One reason we are concerned about patients with COPD during this pandemic is, if they already have problems with low oxygen, the virus can make them worse, potentially bringing oxygen to life-threateningly low levels,” adds Christopher Worsham, M.D., a pulmonologist and intensive care physician at Harvard Medical School in Boston.
A new study helps quantify the added risk of COPD
A new review of studies in the journal Respiratory Medicine showed that COPD patients have over a fivefold increased risk for severe COVID infections — the kind that lands people in the ICU and on a ventilator. COPD patients also tend to be older and have other conditions that up the risk of their health deteriorating when COVID strikes.