AARP Hearing Center
What COPD Patients Should Know About COVID-19
From managing risk factors to why you shouldn't rely on a pulse oximeter

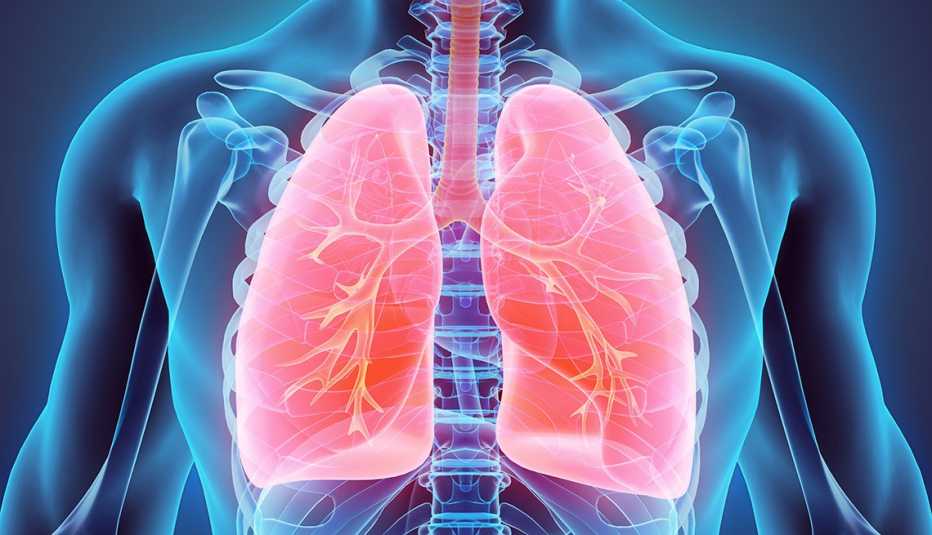
The lungs are ground zero for COVID-19, making underlying respiratory problems a dire concern.
With chronic obstructive pulmonary disease (COPD) in particular, irreversible changes occur in the lungs’ small airways and alveoli — the tiny air sacs at the end of the airway branches where oxygen is delivered to the body and the waste product, carbon dioxide, is removed. As a result of these changes, the number of air sacs can decrease markedly, potentially making the effects of the coronavirus worse.
In severe cases of COVID-19, a patchy, diffuse pneumonia develops, causing the air sacs to fill with fluid, preventing oxygen from crossing into the body. “If there is already a decreased number of air sacs due to COPD, the problem is compounded, increasing the chance for respiratory failure and the need for assisted ventilation with a ventilator,” says Neil Schachter, M.D., a professor specializing in pulmonary medicine at the Icahn School of Medicine at Mount Sinai Health System in New York City.
“One reason we are concerned about patients with COPD during this pandemic is, if they already have problems with low oxygen, the virus can make them worse, potentially bringing oxygen to life-threateningly low levels,” adds Christopher Worsham, M.D., a pulmonologist and intensive care physician at Harvard Medical School in Boston.
A new study helps quantify the added risk of COPD
A new review of studies in the journal Respiratory Medicine showed that COPD patients have over a fivefold increased risk for severe COVID infections — the kind that lands people in the ICU and on a ventilator. COPD patients also tend to be older and have other conditions that up the risk of their health deteriorating when COVID strikes.
COPD patients may also be at greater risk for catching the disease in the first place, Schachter says. Cigarette smoking, which often precedes COPD, and COPD itself are known to increase the number of ACE (angiotensin-converting enzyme) receptors — the structures on the surface of airway cells — that the COVID virus attaches to and then penetrates.
Steps to take to protect yourself
For these reasons, experts say COPD patients need to be especially diligent about avoiding exposure to the virus. “We offer the same advice we would give folks with chronic lung conditions when there are poor air-quality days, like a muggy period of summer: Stay inside as much as possible,” says Jonathan Parsons, M.D., a pulmonologist and associate professor of internal medicine at the Ohio State University Wexner Medical Center. During this time, physical distancing, good hand hygiene and wearing a mask are also critical.


It’s also more important than ever to manage your condition. “This includes vaccination against flu and pneumococcus, and treatment of the airway obstruction with appropriate bronchodilator and anti-inflammatory medications, and oxygen use as indicated by your physician,” Schachter says.
If your COPD symptoms worsen, get help immediately. “Some people, out of a concern about contracting COVID, are ignoring or minimizing symptoms and pushing back at the idea of coming in seeking in-person medical attention when they really need it,” says Benjamin J. Seides, M.D., director of interventional pulmonology at Northwestern Medicine Central DuPage Hospital. “We’ve seen an increase in patients presenting with non-COVID-related problems who have waited a lot longer than they normally would to come to the hospital, thereby making their problems less manageable.”
If you develop flulike symptoms, difficulty breathing, or notice a bluish or purplish color in your lips or fingertips, call your doctor right away, Worsham says. The same goes if you use oxygen at home and find that you need more oxygen than usual.
And don’t rely on store-bought pulse oximeters — devices that go over the fingertips to measure oxygen levels — to gauge your lung health. “These can be very inaccurate and can provide false reassurance,” Worsham says. “Again, the best thing to do with breathing or oxygen concerns is to call the doctor’s office.”
If you do end up with COVID, keep in mind that most patients — including those with COPD — survive. “Every day we’re getting better at managing these patients,” Seides says.


































































MORE ON HEALTH
Coronavirus: Impact on Lungs, Heart, Brain
Understanding the system-wide toll the virus takes — and how to protect yourselfCOVID-19 Insights for People 50-Plus
A CDC official explains why more risk comes with age from COVID-19
5 Ways to Boost Your Immune System
Science-backed tips for strengthening your immune response quickly and effectively