AARP Hearing Center
A highly contagious and potentially fatal fungal infection is spreading at an alarming rate in health care facilities including hospitals and nursing homes, according to data collected by the Centers for Disease Control and Prevention (CDC).
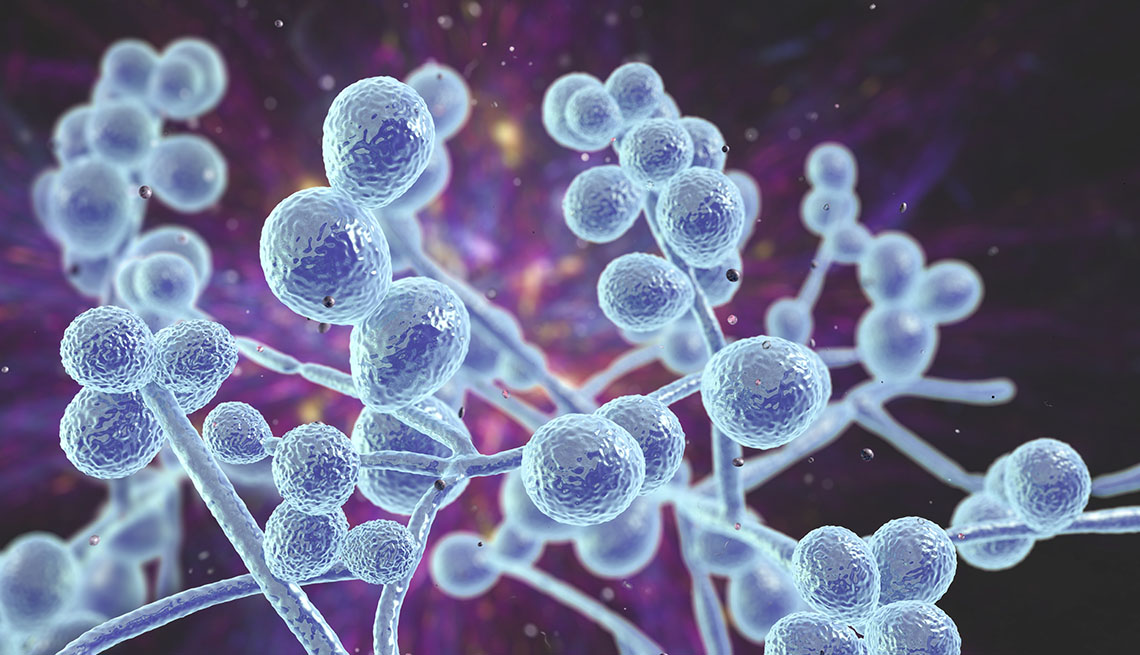
First reported in the U.S. in 2016, the fungus Candida auris is now considered an “urgent antimicrobial resistance (AR) threat” by the CDC because it spreads easily in health care facilities, is increasingly resistant to antifungal drugs and can cause severe, sometimes deadly, infections, particularly in hospital and nursing home patients with serious medical problems.
More than 1 in 3 patients with invasive C. auris — infections that affect the blood, heart or brain — die, according to the CDC. Health officials say it is not a threat to most healthy people.
Nationwide, cases of C. auris infections rose from 476 in 2019 to 1,471 in 2021. Moreover, there was a tripling in 2021 of the number of cases that were resistant to echinocandins, the antifungal medicine most recommended for treatment of C. auris infections, according to a study published in the Annals of Internal Medicine.
Most transmission occurs in health care facilities, especially among residents of long-term care facilities or among persons using catheters, feeding tubes, mechanical ventilators or other similar devices. The CDC has continued to see an increase in case counts for 2022.
“The rapid rise and geographic spread of cases is concerning and emphasizes the need for continued surveillance, expanded lab capacity, quicker diagnostic tests, and adherence to proven infection prevention and control,” said CDC epidemiologist Meghan Lyman, M.D., lead author of the paper.
The CDC also notes that the fungus can spread through contact with affected patients and contaminated surfaces or equipment.
What you need to know about C. auris
1. It takes a laboratory test to determine if someone has a C. auris infection. Symptoms aren’t always noticeable because the infections often occur in individuals already sick with another serious illness or condition. Plus, the fungus can infect a variety of body parts that result in different symptoms, according to the CDC.
2. Most infections are treatable with echinocandins, but not all. Several new antifungal medications are in development, but Lyman and her colleagues write that “more research is needed to understand outcomes for patients with these highly resistant strains and to guide treatment.”
3. Family members, who are otherwise healthy, are at low risk of getting infected. If they are visiting a relative with an infection in a nursing home or hospital, they should wash their hands thoroughly afterward, according to the CDC. In most instances, the CDC does not recommend that family members or other close contacts of patients with an infection be tested for C. auris.