AARP Hearing Center


In this story
Not a bill • Three kinds of MSNs • Recordkeeping • Go electronic • Also known as
A Medicare summary notice (MSN) is a quarterly statement showing your Medicare Part A and Part B health care coverage claims. If you have original Medicare, you probably recognize it as your health care statement noting providers and hospitals you’ve seen because they send their bills for your care directly to Medicare. The big distinction here is that this is not a bill.
Instead, your MSN shows the services and supplies billed to the program the previous quarter as well as how much Medicare paid and the maximum amount you owe a provider. It’s similar to an explanation of benefits (EOB) notice you receive from private health insurance companies.
If you prefer to see your activity every month, you can sign up for electronic MSNs (eMSNs). You can also review your claims for parts A and B in your online account within 24 hours without having to wait for your MSN.
Like any other medical form, even though your MSN is not a bill, you should still review it carefully. It can help you keep track of the care you’ve received and monitor your out-of-pocket costs. It also can help you spot errors — and even instances of fraud — on your Medicare account.
How do I read the Medicare summary notice?
There are three kinds of Medicare summary notices — Medicare Part A, Part B and durable medical equipment — with different information about claims and appeals.
All Medicare summary notices include:
- A list of services
- Claim approvals
- How to appeal denied claims info
- Appeal filing deadlines
- How to get help filing an appeal info
- Appeal form (last page)
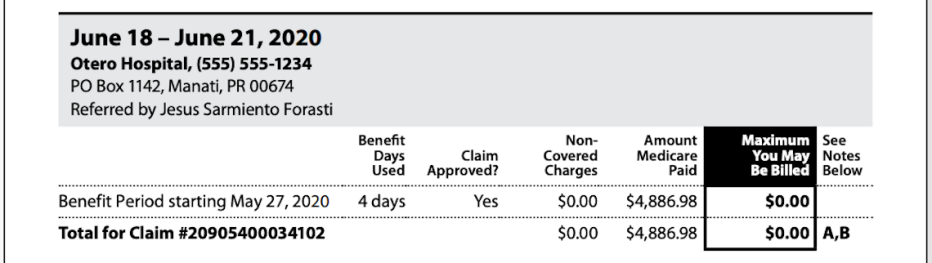
Part A Medicare summary notice
This MSN identifies coverage for inpatient care in a hospital or skilled nursing facility, certain home health care services and end-of-life hospice care. It contains:
- Service dates at each facility
- If the claim was approved
- What Medicare paid and what you owe
- What you’ve paid toward your Part A deductible during that benefit period, including the date the benefit period began and how many days you’ve used
For more information, see the Part A MSN example at Medicare.gov.








































































Next in Series
What is Medicare Assignment? How Does It Work?
You’ll pay less if your doctor accepts assignment