Staying Fit
While the world’s attention remains focused on battling COVID-19, another global health crisis is intensifying — and it’s one that could change the way we treat simple infections, like strep throat, or go about doing routine surgeries, such as joint replacements.
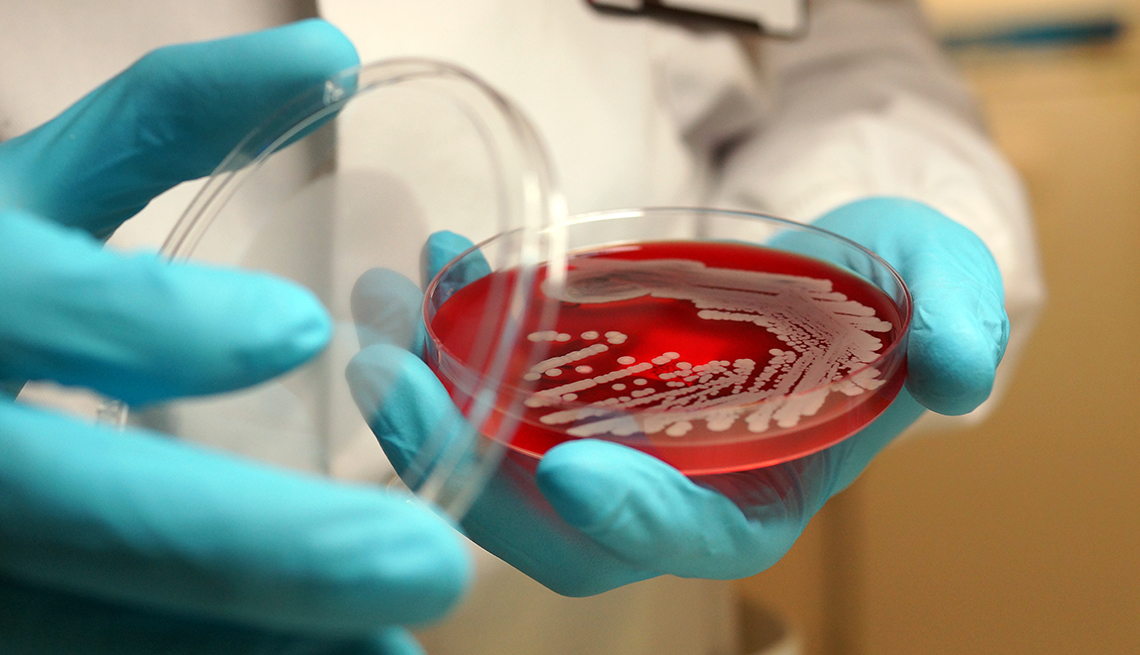
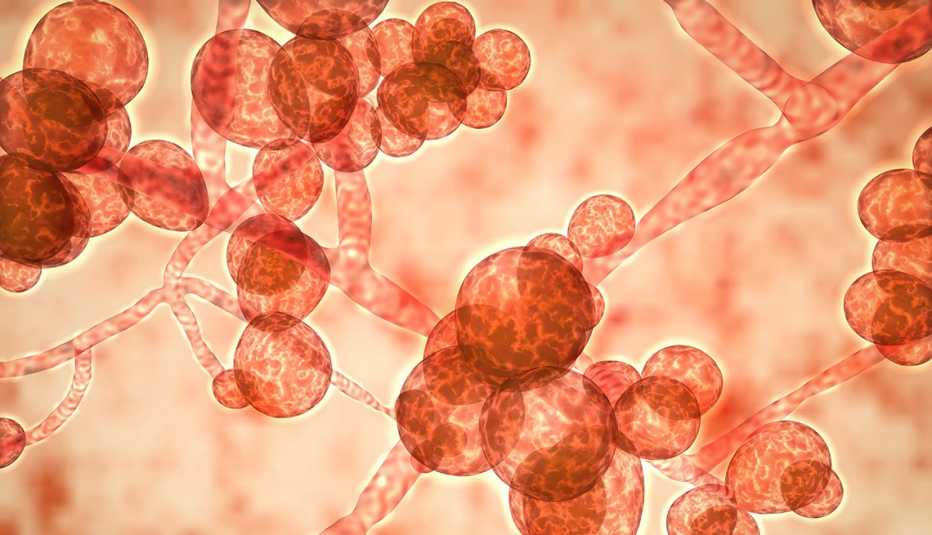
What is a superbug?
A superbug is any microbe — bacteria, virus, parasite or fungus — that has grown resistant to most of the medications commonly used to treat the infections it causes.
Source: Mayo Clinic
It’s antibiotic resistance, and it’s “rising to dangerously high levels,” the World Health Organization (WHO) says. In the U.S. alone, more than 35,000 people die from antibiotic-resistant infections each year, according to the latest data from the Centers for Disease Control and Prevention (CDC). Globally, that number is at least 700,000, and by 2050, it could be 10 million, experts predict.


AARP Membership— $12 for your first year when you sign up for Automatic Renewal
Get instant access to members-only products and hundreds of discounts, a free second membership, and a subscription to AARP the Magazine.
“People are calling it the silent pandemic,” says David Weiss, director of the Antibiotic Resistance Center at Emory University’s School of Medicine. “It's more like a slow-developing chronic [issue], but it could definitely get to pretty epidemic proportions.”
Yet despite the danger it poses, antibiotic resistance is widely misunderstood, global research shows. Here are six myths about antibiotic resistance, plus tips on how you can protect yourself from a superbug infection.
Myth 1: Antibiotic resistance is when people become resistant to antibiotics
Fact: Antibiotic resistance is when bacteria become resistant to the drugs designed to kill them. It does not mean that people develop a resistance to antibiotics. “The simplest way to understand it is that the bacteria are just trying to survive,” Weiss says, and they do that by mutating, or changing their genetic material, in order to escape the lethal effects of the drugs. Those that succeed continue to grow and spread.
Fungi can also morph into drug-resistant germs, as can viruses. “And what is happening is we're seeing that this is becoming more and more frequent,” says Matthew McCarthy, M.D., an associate professor of medicine at Weill Cornell Medicine and author of Superbugs: The Race to Stop an Epidemic. “And that means we're running out of treatment options.”
Having a smaller arsenal of effective drugs makes treating infections caused by drug-resistant bugs more difficult — sometimes impossible. In many cases, antibiotic-resistant infections require extended hospital stays and expensive and toxic treatment alternatives, the CDC says.
Several types of bacteria that cause common ailments — like urinary tract infections and pneumonia — have become resistant to antibiotics, the U.S. Food and Drug Administration reports. Bacteria that cause skin infections and meningitis also make the list.
Myth 2: Antibiotic resistance is a new phenomenon
Fact: Germs have been outsmarting drugs for decades. In fact, shortly after the first antibiotic was introduced in 1941, researchers identified a bacteria that was resistant to it. But it never became the problem it is today because science was always one step ahead.