AARP Hearing Center


Black adults hospitalized with COVID-19 are more likely to suffer from obesity, hypertension, diabetes and heart failure than their white counterparts, according to a study that found that these preexisting conditions were evident in nearly two-thirds of the 906,849 American adults hospitalized as of Nov. 18, 2020.
But for those preexisting conditions, which are often associated with poor diet, as many as 575,419 adults in the United States, including many 50 and older, may have avoided hospitalization, according to the study, which was led by Tufts University researchers and published in the Journal of the American Heart Association. Doctors refer to obesity, hypertension (high blood pressure), diabetes and heart failure as cardiometabolic conditions.
"Our findings lend support to the need for prioritizing vaccine distribution, good nutrition and other preventive measures to people with cardiometabolic conditions, particularly among groups most affected by health disparities,” lead author Dariush Mozaffarian, a cardiologist and dean of Tufts’ Friedman School of Nutrition Science and Policy, said in a statement.
In breaking down the numbers, the researchers noted that disparities were evident by age, race and ethnicity.
Together, the four preexisting conditions factored into 44.2 percent of COVID-19 hospitalizations among those ages 18 to 49, 64.5 percent among those 50 to 64 years old and 73.9 percent among those 65 and older. The proportion of hospitalizations attributable to the four conditions combined was highest in Black adults of all ages, followed by Hispanics, according to the study. Among young adults ages 18 to 49, the four conditions jointly were estimated to cause about 39 percent of COVID-19 hospitalizations among white subjects, compared with 50 percent among Black adults.
Separately, the preexisting conditions have a wide-ranging role across age, race and ethnicity among adults hospitalized with COVID-19.
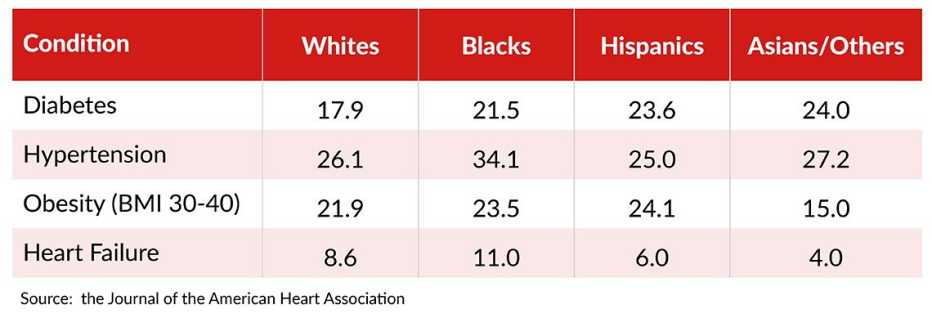
- Diabetes ranged from 6.1 percent among white patients (ages 18 to 49) to 33.7 percent among Hispanics 65 and older.
- Hypertension ranged from 7.4 percent among Hispanics (18 to 49) to 38.1 percent among Blacks 65-plus.
- Heart failure ranged from 0.7 percent among white patients (18 to 49) to 28.2 percent among Black patients 65-plus.
- Obesity (BMI 30 to 40) ranged from 14.6 percent among Asians 65-plus to 24.1 percent among Hispanics (ages 50 to 64).
- Severe obesity (BMI >40) ranged from 6.7 percent among Asians (ages 18 to 49) to 16.9 percent among Black patients (18 to 49).







































































More on health
COVID-19 Could Leave Millions of Minorities Without Health Insurance
More Blacks, Hispanics, Asians uninsured due to pandemic-driven job lossesNursing Homes With More Minority Residents Had Triple the Number of COVID Deaths
In a national study, researchers conclude that this outcome stems from historic disparities in the facilities
Medicare Data Shows Older Minorities Hit Hardest by COVID-19
Black, Hispanic, American Indian/Alaskan Native beneficiaries hospitalized at highest rates