Staying Fit
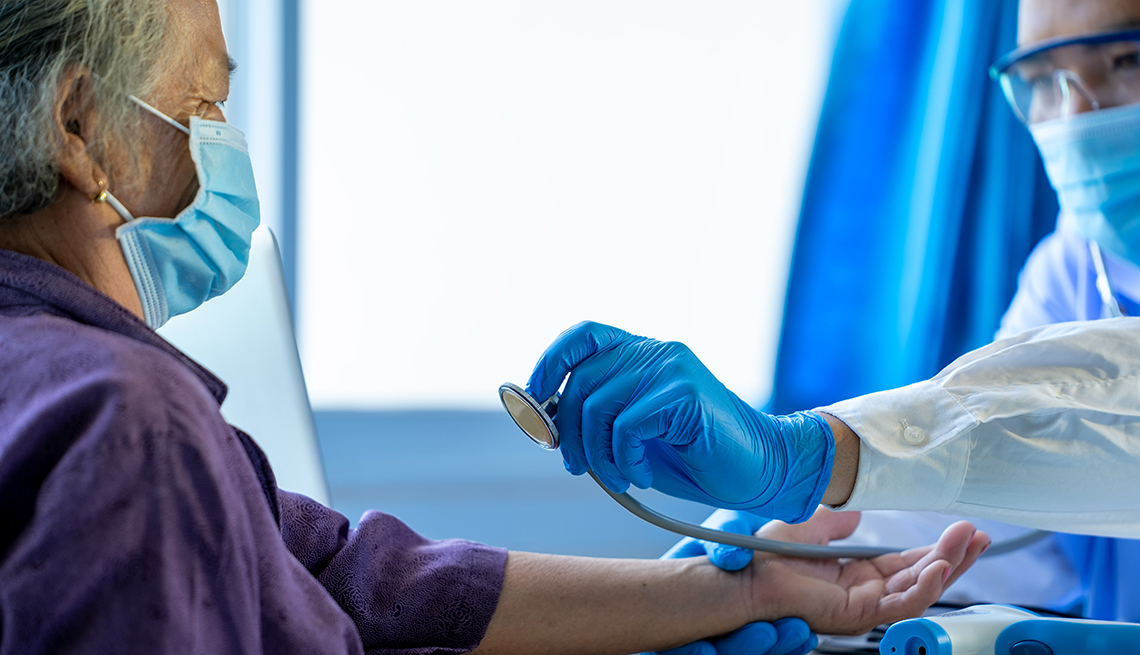
Ron Thomas, 69, of Clemson, South Carolina, had never been hospitalized before he got COVID-19 in July.
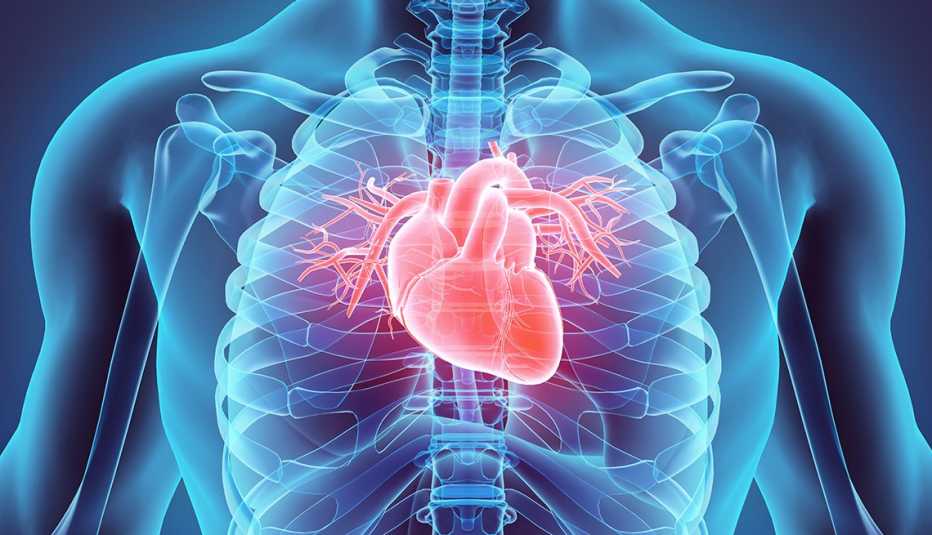
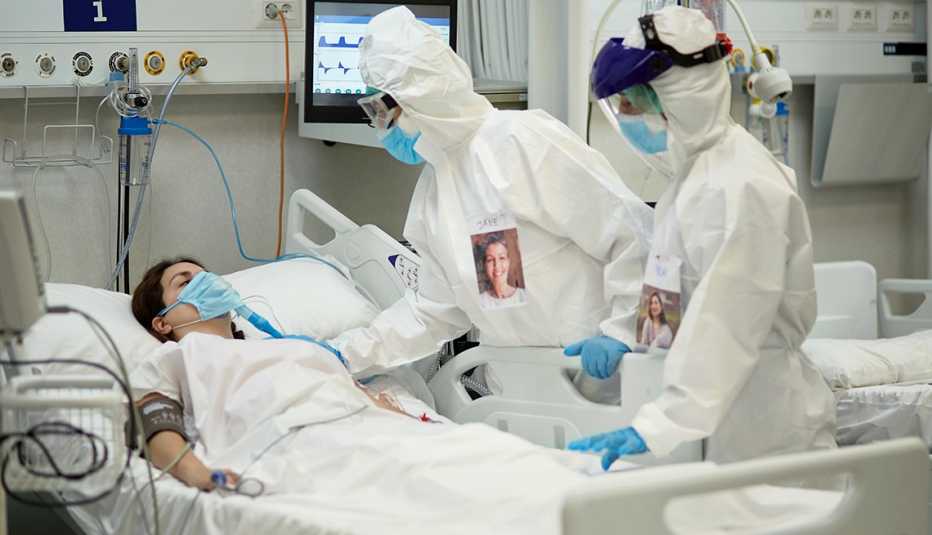
After spending 12 days in the hospital, Thomas developed atrial fibrillation (AF), a rapid and irregular heart rate that causes poor blood flow and can lead to blood clots or even stroke. He needed to go back and forth to the hospital six times for the heart condition — twice in a single night.


AARP Membership— $12 for your first year when you sign up for Automatic Renewal
Get instant access to members-only products and hundreds of discounts, a free second membership, and a subscription to AARP the Magazine.
Thomas describes the condition as unsettling and frightening. “I felt shortness of breath and fluttering in my chest because my heart was racing at 150 to 160 beats per minute.” The symptoms sometimes lasted as long as an hour, until he thought he would pass out.
While doctors have gotten the condition under control with medication, Thomas, an avid golfer, says it's affected his lifestyle.
"This slowed me down,” he says. “I was pretty active, but I'm not able to walk the golf course anymore.” He also had to pare back coaching a local teen golf team because the medications that control his AF also make him lethargic.
While such reports of cardiac problems have mounted after nearly a year of the pandemic, experts say some of the issues they see following a COVID-19 infection may resolve on their own. For now, they report, it's difficult to know which COVID survivors should be screened for which heart issues.