AARP Hearing Center

Key takeaways
- Your risk of arthritis increases as you age.
- Osteoarthritis is the most common type of arthritis.
- Grinding or grating sounds in your joint may be a sign the cartilage has worn down.
- Many cases of arthritis develop from previous injuries to joints.
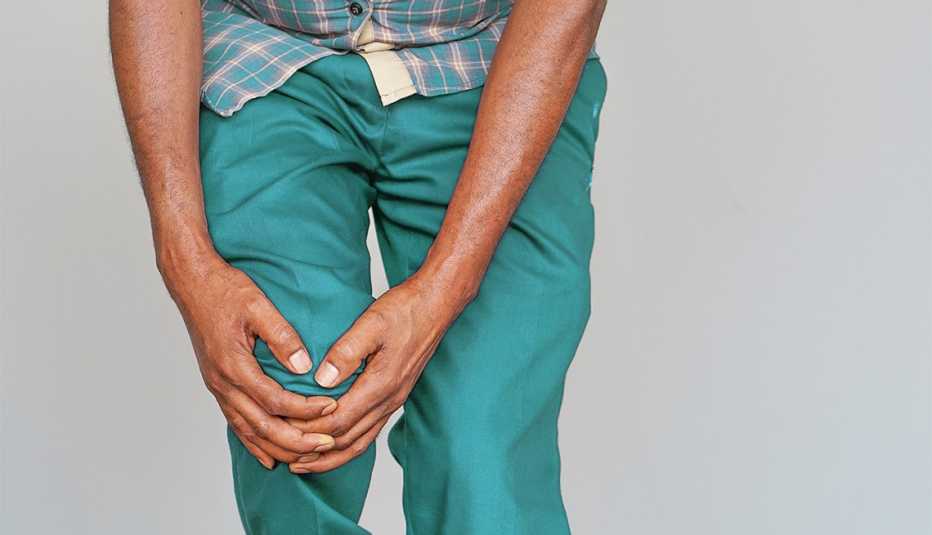
- Groin pain could actually be hip arthritis.
It’s not unusual to experience pain in your joints on occasion, especially if you’re active and participate in high-impact activities, such as running. That unwanted ouch can be caused by injured muscles, tendons and ligaments around the joint — or by tendinitis. It may also be because it’s time to upgrade your mattress. But if you start experiencing aching, pain and stiffness on a routine basis — and particularly if the pain is right at the joint — those are signs of arthritis, says Dr. Uzma Haque, rheumatologist and associate professor of clinical medicine at Johns Hopkins Medicine.
Studies show that cases of early-onset osteoarthritis are rising, largely driven by obesity. But your risk of arthritis increases as you age, and it’s a leading cause of disability in the U.S., affecting around 58.5 million people, according to the Centers for Disease Control and Prevention (CDC).
Inflammatory arthritis vs. osteoarthritis
Arthritis actually describes more than 100 different conditions that affect joints and the surrounding tissue. They fall into two main categories: inflammatory arthritis and osteoarthritis.
Inflammatory arthritis is a systemic disease that’s caused when your immune system mistakenly attacks your joints and tissues, causing pain, swelling and stiffness. The most well-known example is rheumatoid arthritis (RA), which tends to be symmetrical, meaning you’ll have problems in the same joints on both sides of your body, like both wrists or both knees.
Osteoarthritis is a degenerative disorder caused by trauma or age-related wear and tear on your joints. Osteoarthritis is most likely to affect weight-bearing joints such as the knees, hips, lower spine or big toe, but it can also cause pain and stiffness in your thumb or finger joints.
8 early signs of arthritis
Wondering what arthritis feels like? The signs of early-onset arthritis and arthritis that develops after age 50 are the same. Here are some early arthritis symptoms that should prompt you to see a medical provider.
1. Pain in a joint.
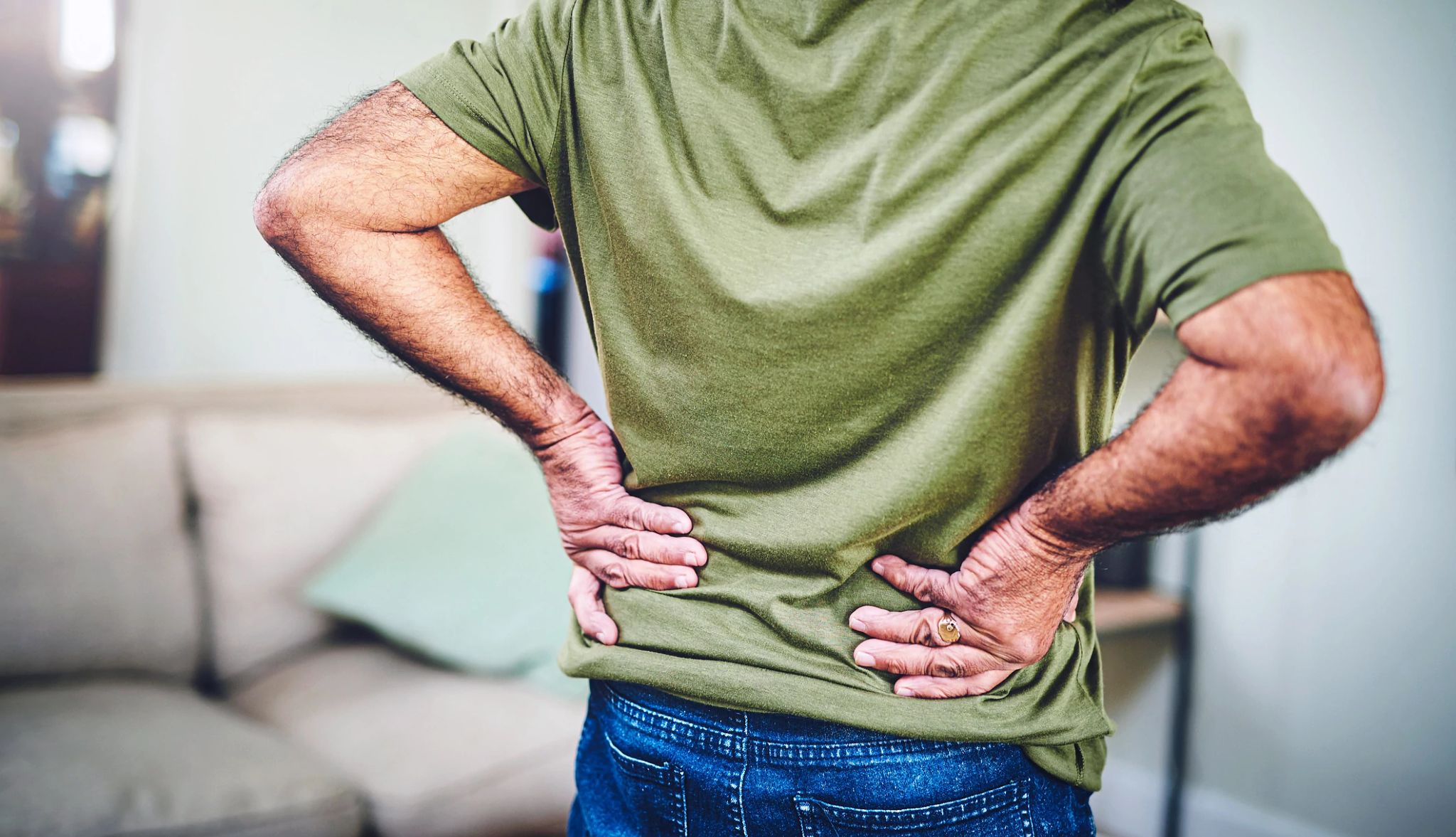
Pain or aching in a joint that gradually becomes worse over time is a classic symptom of arthritis, says Dr. Lisa Cannada, an orthopedic trauma surgeon at Novant Health in Charlotte, North Carolina. The pain may come on during activity, or it may come on after activity or at the end of a long day.
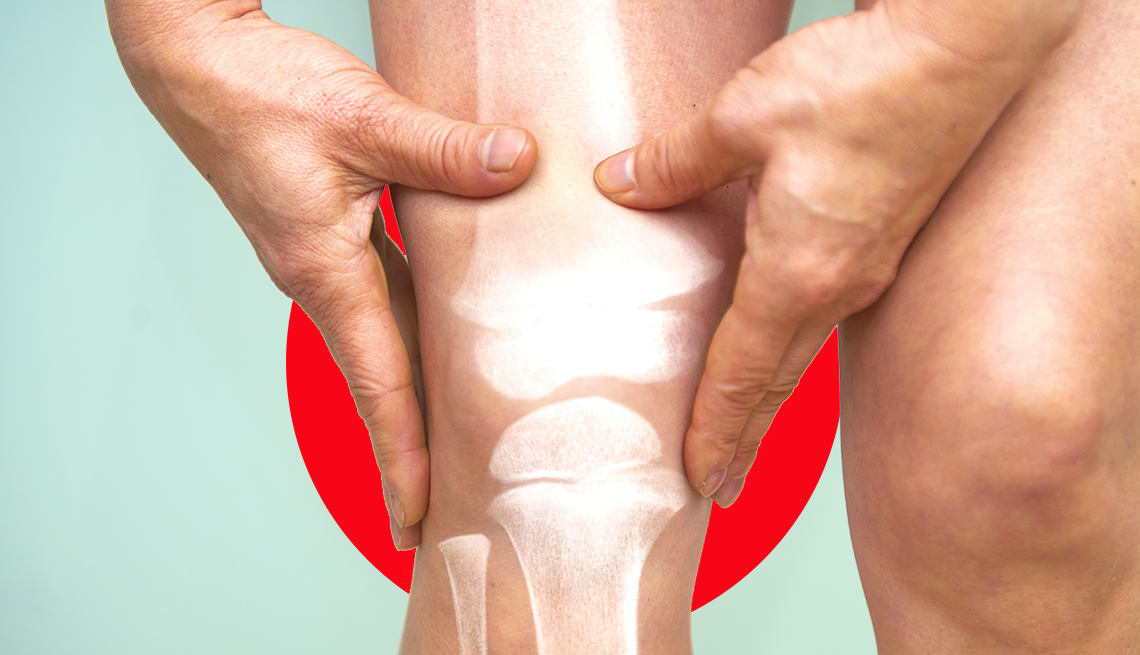
2. Joint swelling and tenderness.
As arthritis gets worse, it can cause joints to be swollen and tender. It may hurt when you press down on the joint.

















































































More From AARP
7 Hand Exercises to Prevent Arthritis
How to stay loose and pain free
AARP Smart Guide to Sleep
35 ways to help fight restless nights and get the slumber you need
Arthritis Diet: What to Eat for Joint Relief
8 superfoods that can help reduce arthritis pain and inflammation.