AARP Hearing Center

Charles Friedlander had the heebie-jeebies about cataract surgery. A gastroenterologist, Friedlander, 75, was no stranger to surgery. Still, “it’s always nerve-racking having someone do something to your eyes,” he says. But on this early spring Friday, he’s calm and relaxed on a gurney at New York Eye and Ear Infirmary of Mount Sinai, awaiting his second procedure in four weeks. “The first went so well, I thought, let’s get the other eye done,” he adds.
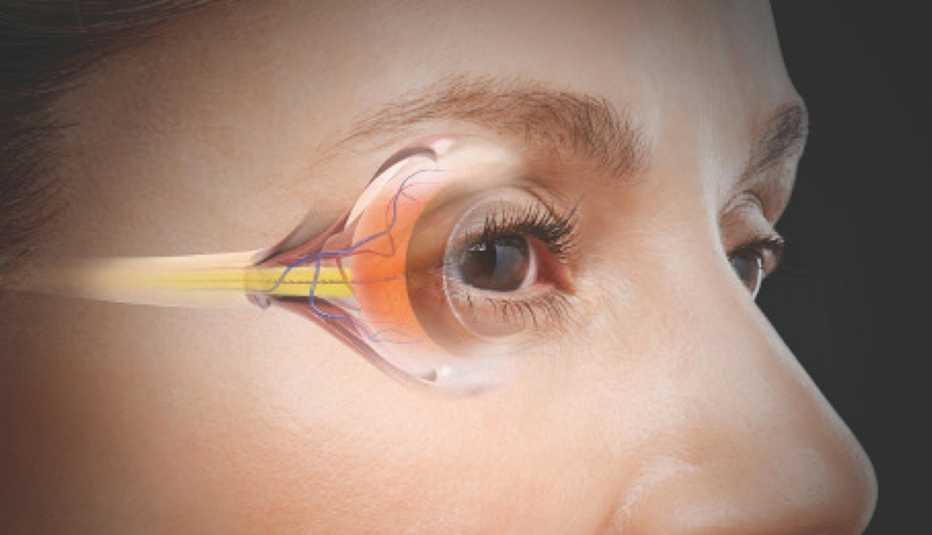
The focal point of Friedlander’s surgery is the artificial lens his ophthalmologist, Tal Raviv, will insert in place of the stiff, cloudy natural lens in Friedlander’s right eye. Called the Tecnis Symfony, the replacement is a newly approved, first-in-class EDOF — extended depth of focus — lens.
“It’s such a big leap forward that the Food and Drug Administration has recognized this as a completely new category of lens,” Raviv says.
Most cataract-replacement lenses allow you to focus only near or far; patients must choose in advance which distance they would prefer to see well. A full-range EDOF lens, which allows patients to see their entire depth of vision clearly, has been the holy grail of cataract surgery for many years, Raviv explains, but early versions were more prone to glare and halos — side effects that are reduced (although not eliminated) with the Symfony lens, for which Raviv is a consultant. The Symfony provides sharp focus from far away to the critical middle distance, where people view computers, countertops and dashboards, while minimizing bothersome aberrations. (Reading a book may still require reading glasses.)
If Friedlander also had glaucoma — as about 20 percent of Raviv’s patients do — the ophthalmologist could simultaneously install a tiny stent that drains fluid from the eye, relieving pressure that can damage the optic nerve. The iStent, which is about the size of a 1 in the date on a penny, is “the smallest implant the FDA has approved for use in the human body, and it’s revolutionizing glaucoma treatment,” Raviv says.
Friedlander’s surgery seems over in the blink of an eye. Raviv takes about three minutes to soften the cataract with intense bursts of laser light, making it easier to remove. “The result is faster recovery,” he notes. Next, Friedlander is wheeled to a darkened room where Raviv peers at his patient’s spotlighted lens through a microscope while an advanced system measures the eye and projects the surgery on a flat-screen TV. About nine minutes later, the new lens is in place.
Sitting in a recovery room a half hour later, Friedlander already sees better. “The light is cleaner and crisper,” he says. After a weekend recovering, he’s back to work at his gastroenterology practice. “Before surgery I couldn’t read at all through my left eye and needed strong glasses through my right,” he continues. “Now I don’t need glasses at all. My vision is back to what it was in my late 40s.”
Advances such as these are changing the way eye doctors treat every major age-related problem. “It’s an exciting time in eye health,” says Julia Haller, ophthalmologist in chief at Wills Eye Hospital in Philadelphia.
Here are some innovations you can set your sights on:
Cataracts
The problem
Proteins that make up the eye’s light-focusing lens start to clump with age, gradually making vision clouded, blurry and sensitive to glare. The Symfony lens is just one of the recent breakthroughs.
New hope
Post-op adjustment: During cataract surgery, your ophthalmologist has to estimate the correction your replacement lens needs, but shifts that occur with healing can throw the correction off, resulting in less than optimal results, says ophthalmologist Nick Mamalis, codirector of the Intermountain Ocular Research Center at the University of Utah. The RxSight Light Adjustable Lens lets doctors alter its power two to four weeks after surgery, when the eye has healed and refraction has stabilized.
A fix for old replacement lenses: If you’ve already had cataract surgery, you may one day be able to upgrade your existing lens. A system in the pipeline by Perfect Lens uses a laser to change the correction on a standard lens already in your eye. If your eyes change over time, you could keep adjusting the same lens without needing another surgery.
Poor night vision together with sensitivity to glare may indicate the beginning of cataracts.






































































More on health
FDA Warns Against Using Contaminated Eye Drops
Testing finds bacteria and fungus