AARP Hearing Center

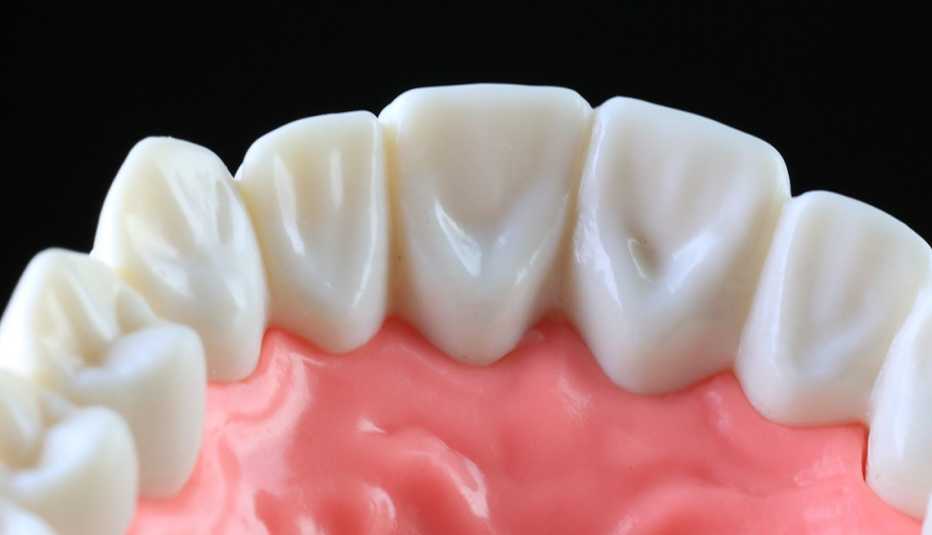
You’ve probably heard the expression “long in the tooth,” but when it comes to older adults and gum disease, it’s a sad reality. About 70 percent of adults over the age of 65 develop periodontal disease — which in serious cases causes gums to pull away from the teeth — according to the Centers for Disease Control and Prevention (CDC).
But just as you can help minimize wrinkles with lifestyle steps like avoiding the sun, not smoking and eating a healthy diet, there are things you can do to protect your gums, notes Sasha Ross, a dentist at the Cleveland Clinic. Here’s why gum disease creeps up with age, and what you can do to help prevent it.
What’s going on as you age
As you hit your 50s or 60s, you may notice that your gums are receding. While this can sometimes be the result of overzealous brushing, most of the time it’s due to untreated gum disease, says Vera Tang, a dentist and clinical assistant professor of periodontology and implant dentistry at the NYU College of Dentistry. “Gum disease starts when bacteria that contain plaque builds up on your teeth and gums,” Tang explains. “When it’s not removed, it produces toxins that inflame the gums. Over time, that destroys your gum tissue, causing it to separate from your tooth and form spaces called pockets.”
These pockets also collect bacteria, which makes things worse. Over the longer term, gum disease can destroy both your gums and the bones supporting your teeth, which can lead to tooth loss.
While anyone can develop gum disease, there are certain conditions that raise your risk, says Mark Wolff, dean of the University of Pennsylvania School of Dental Medicine in Philadelphia. They include:
- Smoking. As it weakens your immune system, smoking makes it harder for your body to fend off a gum infection and makes it harder for gums to heal. Smokers face twice the risk of gum disease that nonsmokers do, according to the CDC.
- Diabetes. If your blood sugar is not well controlled, high glucose levels in your saliva encourage the growth of bad bacteria. This leads to more plaque on your teeth.
- Certain drugs. Some specific medications, including oral contraceptives, antidepressants and blood pressure drugs, can encourage the growth of plaque on your teeth, raising the risk of gum disease.
- Dry mouth. This condition, where the salivary glands in your mouth don’t produce enough saliva to keep your mouth moist, is more common with age. But since your body relies on saliva to help wash away plaque, dry mouth raises your risk of developing gum disease.






































































More on Health
When Dental Implants Go Wrong
What to know before you get implants — and how to watch for symptoms of infectionKeeping Teeth Healthy for Longer
Simple tips for heading off the common dental problems that come with age