Staying Fit

The federal government’s response to the COVID-19 pandemic is winding down.
The national emergency that went into effect in early 2020 wrapped on April 10, and the public health emergency came to a close on May 11, marking a symbolic end to a pandemic that has taken the lives of more than 1.1 million Americans.


AARP Membership— $12 for your first year when you sign up for Automatic Renewal
Get instant access to members-only products and hundreds of discounts, a free second membership, and a subscription to AARP the Magazine.
There is never a perfect time to end an emergency like this, said Joshua Sharfstein, vice dean for public health practice and community engagement at the Johns Hopkins Bloomberg School of Public Health. But, he said, “I think this reflects the fact that COVID is under much better control than it was a couple years ago.”
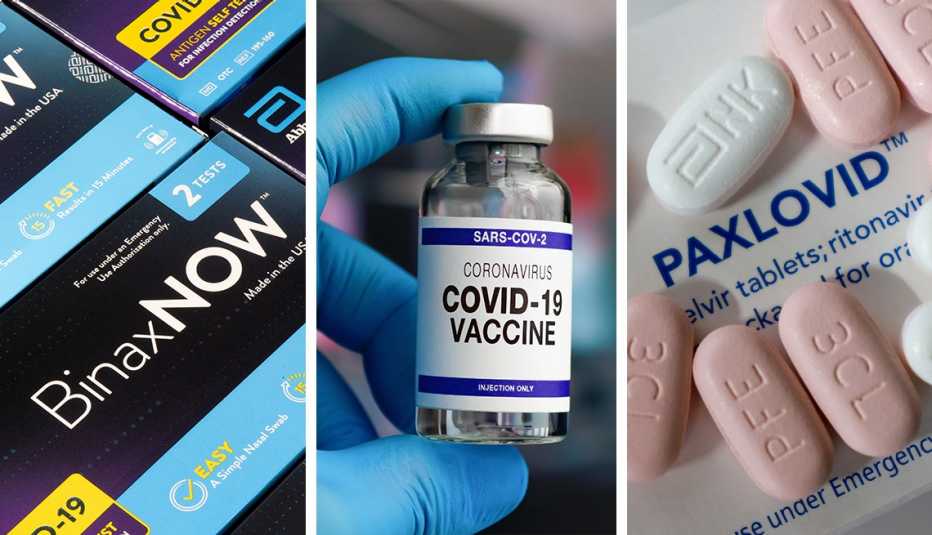
Since 2020, vaccines have been approved that can help keep people from getting seriously sick from a coronavirus infection, and there are now treatments that can help curb COVID complications. We also have greater access to fast, convenient testing and high-quality masks to tamp down on spread.
But the end of the pandemic emergency declarations affects how many people will be able to access these tools.
“One of the more immediate changes that people will notice is that they may be required to pay for things or face cost sharing for things that they have been getting for free under the public health emergency,” said Juliette Cubanski, deputy director of the Program on Medicare Policy at KFF, also known as the Kaiser Family Foundation. How much you end up paying will depend on the type of insurance you have, she added.
End of free at-home tests
Curious if your cough is due to COVID? A quick swab of the nose with an at-home test kit makes it easy to figure out.
These tests “have been really an important new development with COVID,” Mark McClellan, M.D., founding director of the Duke-Margolis Center for Health Policy at Duke University, said in a recent AARP tele-town hall. Testing at home for serious diseases like COVID-19 is “something we didn’t have the ability to do before” the pandemic struck, he said.
For the last year-plus, these over-the-counter tests have been free to many Americans with public and private insurance. Now that is no longer the case.
People with original Medicare will need to pay out of pocket for at-home testing, though tests ordered in a doctor’s office by a health care provider will still be covered. People with Medicare Advantage plans or private insurance may also have to start paying for some or all of these over-the-counter tests — it just depends on your plan.




































































More From AARP
Is It a Cold, the Flu or COVID?
Is It a Cold, the Flu or COVID?
Benefits of Wearing a Face Mask Beyond COVID-19
From allergy relief to keeping your heart healthy
Free At-Home COVID Tests Only Available Until May 11
End of public health emergency means over-the-counter tests will cost you