AARP Hearing Center
9 Signs Your Scaly Skin Patches Could Be Psoriasis
This common condition is easy to confuse with other ailments

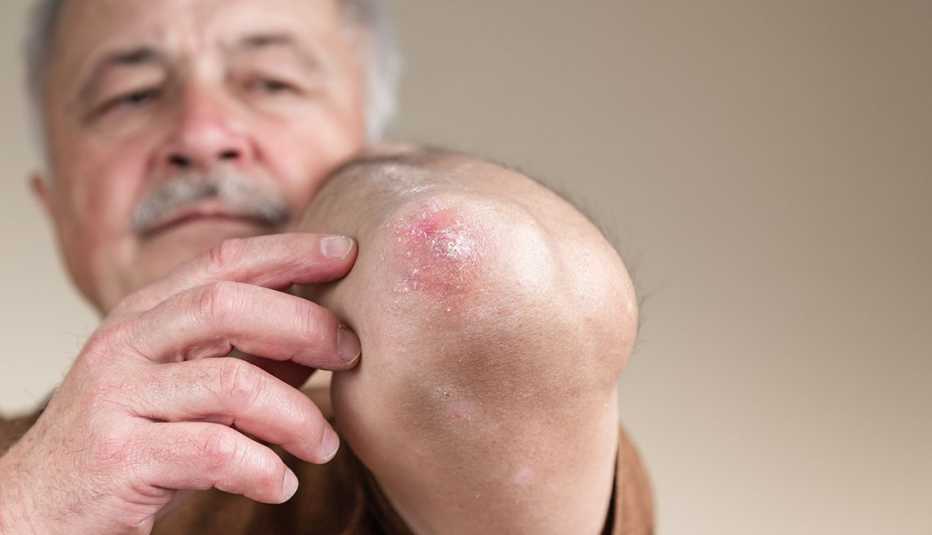
More than 7 million American adults have psoriasis, a chronic skin disease caused by a glitch in the immune system. It’s a widespread and potentially serious condition linked with problems ranging from depression to heart disease. And yet psoriasis is often initially mistaken for something else, experts say.
Psoriasis, in its most common form, produces inflamed scaly patches. The issue is, “there are many other diseases that produce red scaling patches,” says Robert Kalb, M.D., a clinical professor of dermatology at the State University of New York at Buffalo Jacob School of Medicine and Biomedical Sciences.
Most notably, eczema, an even more common skin disorder, causes scaly, inflamed skin. And familiar fungal infections of the skin, including ringworm and athlete’s foot, also create scaly patches. Some rarer conditions cause symptoms that might look like psoriasis as well.
Dermatologists and other doctors well trained in skin diseases usually can diagnose psoriasis quickly by examining your skin and asking a few questions about your medical history, Kalb says. Occasionally, doctors might need to scrape off or cut out a very small skin sample to get a clear answer, says Mark Lebwohl, M.D., chairman of the Department of Dermatology at Icahn School of Medicine at Mount Sinai in New York.
If you haven’t seen a doctor yet, here are nine clues that the scaly patches on your skin might be psoriasis:
1. The patches have clear borders
Psoriasis patches, unlike patches of eczema, have “sharply demarcated” edges that you can clearly see and feel, Lebwohl says. The patches usually look red but might appear purple in dark-skinned people, he adds. A ringworm patch also might have well-defined edges, but it has a distinct circular shape and often a clear area in the center of the ring, according to Cleveland Clinic. If there’s any doubt about whether you have psoriasis or a fungal infection, a doctor can scrape off a bit of the affected skin and look at it under a microscope, Lebwohl says.
2. The inflamed skin is covered by thick scales
In plaque psoriasis, the most common form, an overactive immune system causes skin cells to reproduce too rapidly and build up on the skin surface in thick scales, or plaques. The scales may be white or silvery. Eczema patches typically are covered with finer, flakier scales of dry skin.
3. The patches are on your elbows, knees, scalp, lower back or all of the above
While psoriasis can show up anywhere on your body, the bony parts of the knees and elbows, along with the scalp and lower back, are especially common. Eczema, by contrast, often appears in the creases of elbows and knees and other skin folds, especially in children. It can also show up on the face or hands of adults, according to the National Eczema Association. Most people with psoriasis have it in more than one place, Kalb says, so if you have one suspicious spot, your doctor should check your whole body.
4. You also have fingernail changes
Psoriasis can affect the fingernails in several ways, according to the American Academy of Dermatology. Common signs include tiny dents, or pits, in the nails; white, yellow or brown discoloration; crumbling nails; nails separating from the fingers or toes; and blood beneath the nail. Nail psoriasis typically develops after skin symptoms.
5. You have a family history of psoriasis
If one of your parents had psoriasis, you have a 28 percent chance of developing the condition; if both had it, your risk rises to 65 percent, according to the National Psoriasis Foundation. An estimated 35 to 40 percent of people with psoriasis have one or more family members with the condition. But an absence of family history by no means rules it out: “Psoriasis does tend to run in families, but sometimes you’re the first one,” Kalb says.


6. You’ve had psoriasis before
Psoriasis is a chronic condition that, with treatment, can seem to disappear for a while and then reemerge. New patches can show up even after a long period of control, Kalb says. He says he recently saw a woman with just a couple of mild patches on her body that he might not have confidently diagnosed as psoriasis — until she told him she had been treated for widespread psoriasis years before.
7. Your skin is not intensely itchy or oozing
While psoriasis can cause burning or itching, the itching associated with eczema tends to be much more intense, Lebwohl says. Eczema patches also may ooze fluid, while psoriasis patches do not, he says. He adds one caveat: It is possible to have both eczema and psoriasis at the same time.
8. You also have sore, stiff joints
About 20 percent of people with psoriasis develop a related form of arthritis, called psoriatic arthritis. “The majority of people have psoriasis first, then the arthritis, but there’s a very small percentage of patients who get the arthritis first,” Kalb says.
It’s also possible for both conditions to emerge at about the same time, he says. In addition to sore, stiff joints, people with psoriatic arthritis can have swollen fingers and toes, foot pain and inflamed eyes. If you have such symptoms, you should see a rheumatologist, a doctor who specializes in arthritis, to get a firm diagnosis, Kalb says.
9. You are in your 20s ... or your 50s
In general, age is not a strong clue that your skin condition is or is not psoriasis. “Psoriasis can start at any age,” Lebwohl says. “There have been people born with it [and] people who developed it for the first time over the age of 100.” However, there are peak ages for when the disease tends to show up: One is between 20 and 30 and the other is between 50 and 60, according to the National Psoriasis Foundation.
After the diagnosis
The good news for people newly diagnosed with psoriasis is that “the treatment for psoriasis in the last two decades has improved unbelievably,” Kalb says. Newer drugs provide safe and effective options, even for people with severe cases or complicated medical histories, he says.
Growing evidence also suggests that at least some psoriasis treatments may also reduce the heart risks linked to psoriasis, Lebwohl says. (The chronic inflammation psoriasis causes in the body may affect the heart and blood vessels, putting a person at greater risk for heart disease and stroke, the American Academy of Dermatology explains.)
Among the options for psoriasis treatment:
• Creams and ointments. For people with mild cases, prescription steroids applied directly to the affected skin patches remain mainstays of treatment. Steroids can cause skin thinning, so they must be used with care. (Another option, for people with just one or two troublesome patches, is to inject steroids directly into the psoriasis plaques, Kalb says). Creams, gels and other products containing synthetic forms of vitamin D and vitamin A also may be prescribed.
• Light therapy. If your psoriasis is more extensive, you might be offered so-called phototherapy. Patients go to a clinic two to three times a week, often for months, to stand in a special light box that uses ultraviolet light that is safer than the kind used in tanning booths. You might also take a medication that makes your skin more sensitive to the light. Light therapy is less used than in the past because of the time commitment required, Lebwohl says.
• Pills. Moderate to severe psoriasis also can be treated with prescription pills. These include methotrexate, which is typically taken once a week to decrease inflammation; and apremilast, a newer daily medication that tamps down inflammation; as well as cyclosporine and other immune-suppressing medications. Each of these medications has potential side effects. For example, methotrexate can cause liver damage, apremilast can worsen depression, and cyclosporine can cause kidney damage.
• Shots and infusions. Newer drugs, called biologics, target specific parts of the immune system and are given as shots or intravenous (IV) treatments on schedules that range from weekly (or twice a week) to every three months, Lebwohl says. These medications, which can increase the risk of serious infections, are used for moderate to severe psoriasis. They also treat psoriatic arthritis. They are more expensive than other options and not always covered by insurance.
• Lifestyle changes. Losing weight if you are obese, not smoking and limiting alcohol may all help limit psoriasis flares, studies suggest.
Rarer Forms of Psoriasis
Most people with psoriasis, an estimated 80 to 90 percent, have the most common type, plaque psoriasis, which causes thick, scaly patches. But psoriasis can also take these forms:
Guttate psoriasis. This type mostly affects young adults and children. It is often triggered by bacterial infections, such as strep throat. It typically appears as small, drop-shaped spots on the trunk, arms or legs. The spots usually are covered with a fine scale.
Inverse psoriasis. Inverse psoriasis shows up in the folds of skin around the groin, buttocks, armpits and breasts. Instead of scaling patches, it causes smooth patches of inflamed skin. The condition may be triggered by fungal infections.
Pustular psoriasis. This type produces blisters filled with pus. It can be widespread or confined to small areas of the palms or soles.
Erythrodermic psoriasis. This is the least common type. It can cover the entire body with a peeling rash that may itch or burn intensely. The condition may be short-lived or chronic.
Source: Mayo Clinic


































































MORE ON HEALTH
Stress and Immune Aging: What to Know
Its impact on the immune system could speed up the process, study finds
Avoid These 8 Skin Habits to Stay Healthy
Smoking, scratching and skipping out on SPF can be damaging
The 7 Worst Habits for Your Joints
Everyday actions that can cause inflammation and pain