Staying Fit

With travel booming, office work resuming and social distancing seeming like a thing of the past, dodging COVID-19 — which health experts say is here to stay — has become increasingly difficult.
And while the newly updated vaccines can help to curb the worst of a coronavirus infection, people at increased risk for severe illness due to their age or other health conditions have an additional tool to help ensure their symptoms don’t progress to a critical state: antiviral pills that stop the virus from replicating.


AARP Membership— $12 for your first year when you sign up for Automatic Renewal
Get instant access to members-only products and hundreds of discounts, a free second membership, and a subscription to AARP the Magazine.
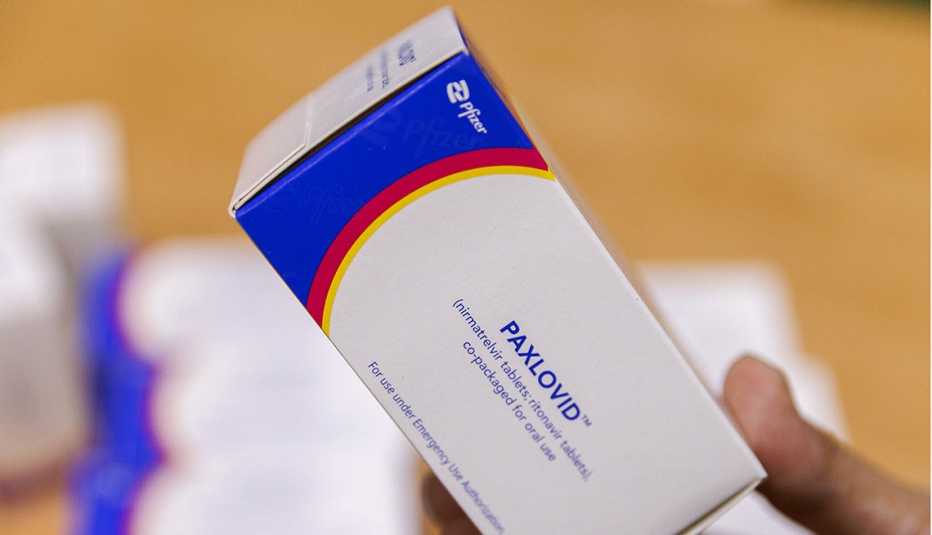
In May, the Food and Drug Administration (FDA) granted full approval to the prescription medication Paxlovid for the treatment of COVID-19. A second antiviral pill, Lagevrio (molnupiravir), is also available through emergency use authorization, though treatment guidelines specify that Paxlovid is the preferred at-home option.
Conditions that increase risk for severe COVID-19
- Cancer
- Chronic kidney disease
- Chronic liver disease
- Chronic lung diseases
- Cystic fibrosis
- Dementia or other neurological conditions
- Diabetes (type 1 or type 2)
- Some types of disabilities
- Heart conditions
- HIV infection
- Immunocompromised conditions
- Mental health conditions
- Overweight and obesity
- Physical inactivity
- Pregnancy
- Sickle cell disease or thalassemia
- Smoking, current or former
- Solid organ or blood stem cell transplant
- Stroke or cerebrovascular disease
- Substance use disorders
- Tuberculosis
Source: CDC
In clinical trials, Paxlovid was found to be highly effective at reducing the risk of COVID-19 hospitalization and death in high-risk patients, and new research shows it still packs a punch when up against the latest omicron subvariants. An observational study published in September in JAMA Network Open found that compared to no treatment, Paxlovid lowered risk of death by 84 percent among patients diagnosed with COVID-19 at Cleveland Clinic between April 2022 to February 2023. Lagevrio reduced the risk by 77 percent.
Still, physicians and public health experts say Paxlovid is underused. Here’s what you need to know about the treatment.
Who should be seeking it?
Testing positive for COVID-19? If you are 50 or older, have certain health conditions (heart disease, lung disease and diabetes are a few examples) or are unvaccinated, talk to a health care provider about getting treated as soon as the double line appears.
With Paxlovid widely available and still free — at least until the government-purchased supply runs out — the approach at this phase in the pandemic should be, “Why shouldn’t you take this?” says William Garneau, M.D., an assistant professor of medicine at Johns Hopkins Medicine.
Of course, not everyone is a good candidate for Paxlovid. People with severe liver and kidney problems should not take it. There are also several medications that can interact with Paxlovid, some of which preclude a patient from getting it.
“And there are other drugs that are what we would consider to be warning drugs, that we can adjust the dose of, or we can withhold for a few days,” says Kelly Gebo, M.D., an infectious disease specialist and professor of medicine at Johns Hopkins Medicine. Examples include certain statins, antidepressants and anticoagulants (blood thinners), so be sure the doctor or pharmacist prescribing Paxlovid is aware of every medication you are taking.
If you’re not eligible for Paxlovid, your health care provider may recommend another treatment, like Lagevrio or remdesivir, an antiviral that’s administered by IV.
“[People] need to understand that there are some options and that they need to work with their providers in their clinics to explore what option is going to work the best for them,” says Mark Rupp, M.D., a professor in the Department of Internal Medicine and chief of the Division of Infectious Diseases at University of Nebraska Medical Center.
“I think the biggest take-home point is don’t just blow it off. Talk to somebody about whether [you should be treated],” says Steven Lawrence, M.D., a professor of medicine in the Division of Infectious Diseases at Washington University School of Medicine in St. Louis.



































































More From AARP
Do You Still Need Your Vaccine Card?
The CDC says it has stopped printing the paper cardsIs It Time to Start Wearing a Mask Again?
Experts share advice as COVID-19 cases start to climbWhat to Know About The COVID BA.2.86 Variant
The new strain has health experts concerned