AARP Hearing Center

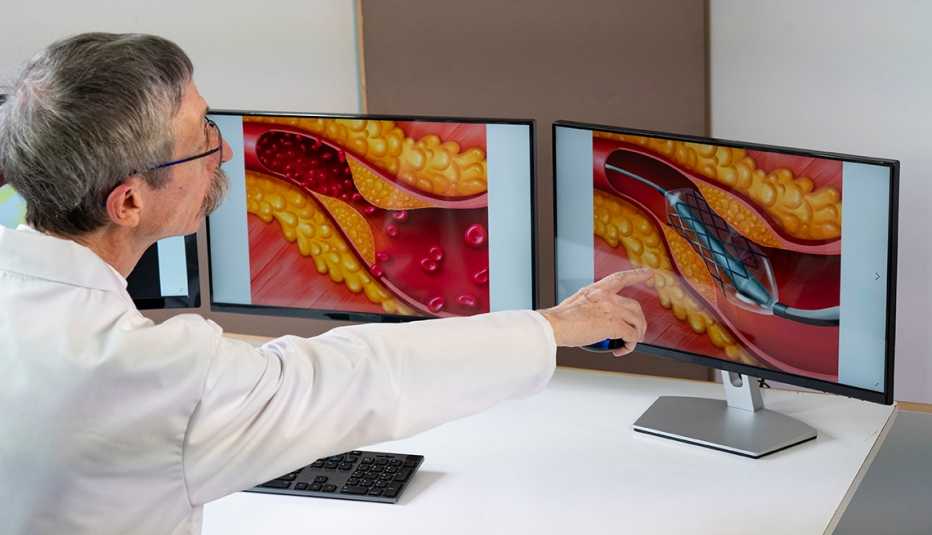
Almost a million Americans each year get a stent — a tiny mesh tube, typically metal, that props open a clogged artery. If you have heart disease, your doctor may recommend one for you, too. But whether you need it is another question.
While the research is clear that stents save lives if inserted during a heart attack, “for most patients with stable heart disease, there's no good evidence that it can save their life or improve their symptoms any more than medication and lifestyle changes,” says Frederick Welt, M.D., chair of the American College of Cardiology's Interventional Section. That evidence includes a major study, published last year in the New England Journal of Medicine, which found that people with heart disease who were treated with medications and lifestyle advice were no more at risk of a heart attack or death than those who got a stent.
That doesn't mean you should avoid stents entirely — again, under the right circumstances, they can save your life, says Welt. Here's the latest thinking on when you need one, and when you don't.
Early days of stents
Stenting, which first became widely available in the 1980s, gained steam when it became clear that it was an effective emergency treatment for heart attacks. In this procedure, also known as an angioplasty, a thin balloon is inflated in the narrowed artery and a stent is inserted to keep the vessel open.
From there, doctors assumed that stents would help with other blockages due to heart disease. “It seemed to make sense intuitively, because the coronary arteries provide blood and oxygen to the heart muscle, and if they're narrowed because of plaque, you can develop symptoms of heart disease such as shortness of breath or chest pain,” explains Rita Redberg, M.D., a preventive cardiologist at the University of California San Francisco and editor of JAMA Internal Medicine.






































































More on health
7 Heart Numbers That Could Reveal Health Risks
Do you know the chances of having a heart attack or stroke? These measurements offer important cluesReal People, Real Heart Attack Stories
Readers react with their own tales of survival in their own wordsYour Cardiovascular Health After 50
How can I keep my heart in top shape?