Staying Fit


Over 80 percent of those diagnosed with cancer nationally are 55 years of age or older, according to the American Cancer Society. But thanks to all the advances in cancer care over the last decade, many are living long, full lives despite their diagnoses.
“Age is really just a number, and there’s no reason why older patients can’t reap the benefits of all these recent medical breakthroughs,” says Richard L. Schilsky, M.D., the chief medical officer of the American Society of Clinical Oncology (ASCO).


AARP Membership— $12 for your first year when you sign up for Automatic Renewal
Get instant access to members-only products and hundreds of discounts, a free second membership, and a subscription to AARP the Magazine.
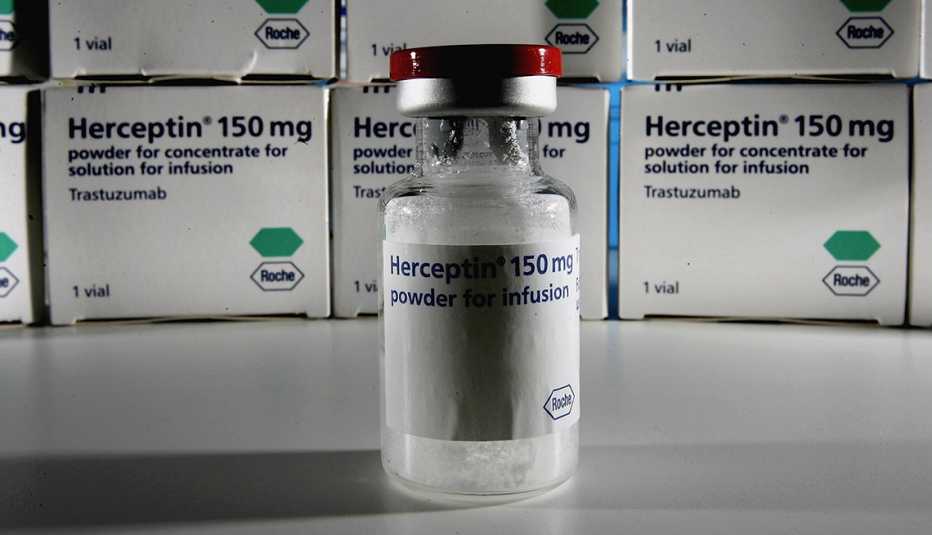
New forms of cancer treatment such as immunotherapy, for example, mean that older adults may live for many years with types of cancer traditionally considered deadly. Here’s what some of the nation’s leading cancer specialists are most excited about for the upcoming decade.

Revolutionizing clinical trials
Only about 3 percent of cancer patients in the United States enroll in a clinical trial. These numbers are even lower in older adults, who have traditionally been excluded from such trials due to pre-existing conditions like type 2 diabetes or high blood pressure. “Even if you’re otherwise healthy, as you age, there’s a good chance that something’s going on that may disqualify you, such as mildly impaired liver or kidney function,” says Ishwaria Subbiah, M.D., assistant professor of Palliative Care at MD Anderson Cancer Center in Houston, Texas.
Many older adults have been essentially denied access to being part of a clinical trial. And such participation can, on occasion, do more than just move forward research. In some cases, cancer drugs being tested in clinical trials “were given fast-track approval by the FDA, which means they were approved soon after clinical trials were finished,” explains Subbiah.
This past March, the FDA issued a new guidance document on broadening cancer clinical trial eligibility criteria. “This will really encourage and motivate trial sponsors to scrutinize their entry criteria to see if it’s really necessary to be so strict with that particular drug,” says Subbiah. “If a medication being tested is metabolized through the liver, for example, then there’s no reason why someone with mildly impaired kidney function can’t participate in that trial. This has the potential to be a real game changer for older adults.”
Over the next decade, clinical trials will also likely become more accessible to older adults with mobility issues or other challenges that make it tough for them to participate. “In the past, clinical trials have been conducted at large medical centers that made people travel to them for every check-up visit,” explains Subbiah. Many major cancer centers and pharmaceutical companies are exploring ways to make it easier on patients, including arranging transportation and housing, and even exploring the possibility of patients being able to check in with the center remotely.

Liquid biopsies
When a patient has a suspicious lump that might mean cancer, their physician usually performs a tissue biopsy, where they take a sample of the lump and examine cells under the microscope to determine if they’re potentially cancerous. But this type of testing may occur late in the game, after the cancer’s already had a chance to grow and spread. Now, major cancer centers are exploring DNA-based liquid biopsies — blood tests where a patient’s blood is analyzed for types of tumor material such as mutated DNA, RNA or proteins. This may mean, one day, that people could be diagnosed with cancer earlier than they would be by more traditional methods such as imaging tests.


































































More From AARP
The Next Frontier in Alzheimer’s Research
Exploring eye scans, gene editing and sound training