Staying Fit
COVID-19 infections in U.S. nursing homes quadrupled between mid-April and mid-May, and the death rate in the facilities is rising once again, a new monthly AARP analysis of federal data shows. At the same time, uptake of COVID-19 booster shots has slowed, leaving some 330,000 residents and more than a million workers without an extra shot.
AARP’s analysis found that the rates of U.S. nursing home residents and workers testing positive for COVID-19 during the period between mid-April and mid-May are comparable to those recorded during COVID-19’s first summer in 2020, when vaccines weren’t available, and during the peak of the delta wave, in the summer and fall of 2021. The infection rate among residents jumped from around 1 in every 200 during the four weeks ending on April 17 to 1 in every 44 for the four weeks ending on May 22. Infection rates among workers were similar.


AARP Membership— $12 for your first year when you sign up for Automatic Renewal
Get instant access to members-only products and hundreds of discounts, a free second membership, and a subscription to AARP the Magazine.
COVID-19 deaths among residents also increased, from around 300 nationally during the four weeks ending in mid-April to more than 500 for the four weeks ending in mid-May. Reports from the Centers for Disease Control and Prevention (CDC), which include data from two additional weeks beyond AARP’s analysis, show that resident deaths have continued to rise since then. And the figure is likely to be revised upwards in coming weeks, as nursing homes submit more data.
Booster uptake in nursing homes, meanwhile, has slowed to a crawl. About 72 percent of residents and 48 percent of staff nationwide had received at least one booster dose as of mid-May, up slightly from 70 percent and 46 percent, respectively, as of mid-April. Those slight upticks represent the lowest monthly increases since booster data became available last fall.

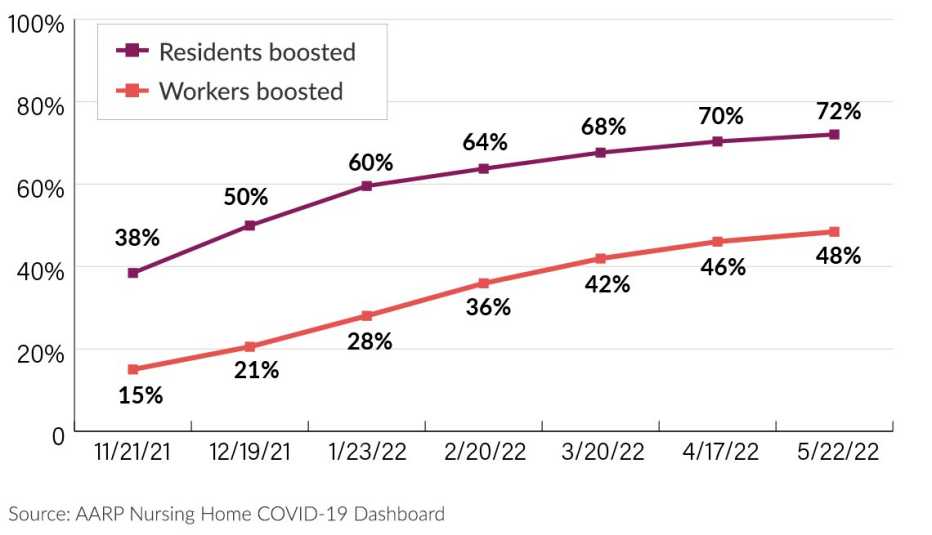
Booster rates slow among U.S. nursing home population
“They’re by far the smallest jumps we’ve seen,” says AARP’s Ari Houser, a senior methods adviser and coauthor of AARP’s monthly analyses. “Which is worrying, because they’re still well below where they should be, particularly in some states.”
Florida, the state with the fourth highest population of nursing home residents, reported that just 57 percent of residents had been boosted as of mid-May — the lowest rate in the country. Mississippi and Missouri reported that only 27 percent of workers had been boosted.
Massachusetts, South Dakota and Vermont, meanwhile, reported that 88 percent of residents had received an extra dose — the highest rates in the country. Massachusetts, which is requiring nursing home workers to be boosted, reported that 96 percent had received an extra shot. California and Connecticut, which have similar mandates for workers, reported booster rates of 86 and 89 percent, respectively.

































































More on caregiving
AARP Answers: Nursing Homes and the Coronavirus
The latest on evolving rules, visiting loved ones, your rights and more10 COVID-19 Questions to Ask a Nursing Home
Guidance for caregivers during the COVID-19 pandemicNursing Aides With Direct Resident Contact Least Likely to Be Vaccinated
Study suggests unvaccinated staff can spark outbreaks, even if residents have shots