AARP Hearing Center
If you qualify for Medicare before age 65, your ability to get a Medigap policy depends on the state where you live.
Medicare supplement policies, also known as Medigap, help pay Medicare’s deductibles, copayments and other out-of-pocket costs. People 65 and older can get any Medigap policy available in their area at the best rates if they buy at certain times — such as within six months after signing up for Medicare Part B.
Roadblocks if you’re younger. Those federal protections don’t apply to people who are younger than 65 and qualify for Medicare because of kidney failure, also known as end-stage renal disease (ESRD), or another disability. This is where state protections can kick in.
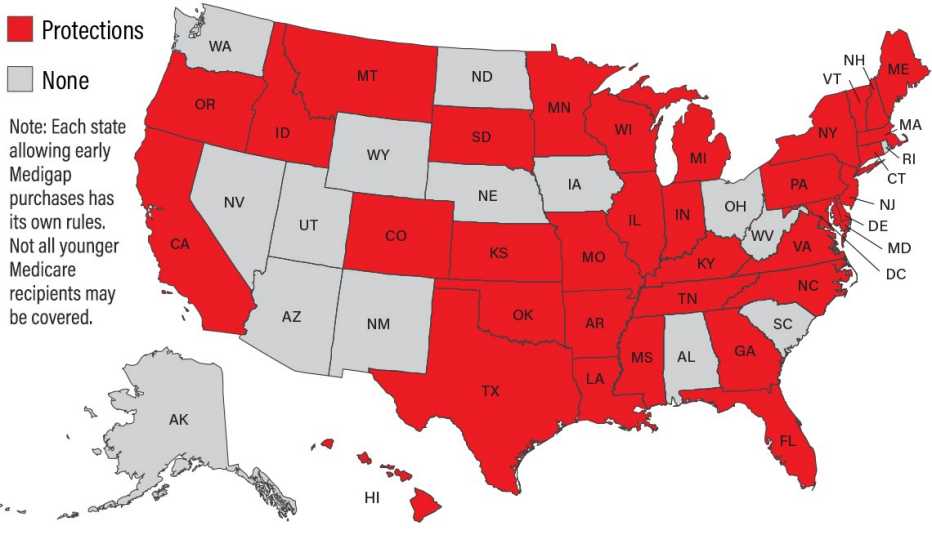
Thirty-four states now require Medigap insurers to offer at least one policy to Medicare recipients younger than 65. Some insurers may limit coverage to one or two plans, and only to people with certain conditions.
Without a Medigap policy or other supplemental coverage, such as employer or retiree health insurance, you may have to pay Medicare’s deductibles and copayments yourself, which can add up quickly, depending on your medical condition.
An example. Even though Medicare Part B covers outpatient dialysis for people with kidney failure, without other supplemental coverage you’ll have to pay 20 percent of the cost — called Part B coinsurance. The American Kidney Fund estimates that Part B coinsurance can cost dialysis patients $10,000 or more out of pocket each year. To make matters worse, not having supplemental coverage could jeopardize your chance to get on a kidney transplant list.
What are state rules for Medigap under age 65?
Medigap coverage rules for those younger than 65 vary considerably by state.
- Fifteen states and the District of Columbia don’t require insurers to offer Medigap policies to people enrolled in Medicare who are younger than 65. In 2022, they are Alabama, Alaska, Arizona, Iowa, Nebraska, Nevada, New Mexico, North Dakota, Ohio, Rhode Island, South Carolina, Utah, Washington, West Virginia and Wyoming.







































































More on Medicare
New Medicare Benefits for Chronic Conditions
What to consider during open enrollmentMedicare Savings Programs Can Save Enrollees Thousands
AARP Foundation helps older adults sign up
The Big Choice: Original Medicare vs. Medicare Advantage
Which path you take will determine how you get your medical care — and how much it costs