AARP Hearing Center


Pat Cutillo suffers from chronic hypertension. The 85-year-old retired teacher no longer automatically has to make the 10-mile trip to the nearest emergency room when her blood pressure gets dangerously high because she can call her primary doctor’s office 24/7 to get immediate help.
Christine Meyer is Cutillo’s internist. About seven years ago Meyer, whose practice is based in Exton, Pennsylvania, a Philadelphia suburb, joined a Medicare accountable care organization, also called an ACO. These groups were created to coordinate the care of patients, including those enrolled in original Medicare. Providers who join an ACO commit to improving their patients’ health while also keeping costs down. If they do, they earn financial incentives.
The extra money Meyer gets by meeting her ACO savings and quality goals has enabled her to afford to expand her practice’s services. She has added hours, including at night and on weekends. She’s hired more clinicians and support staff. And she created what she calls the BAT phone. BAT stands for “before all that.” Meyer gives the BAT phone number to her sickest patients, those who might have to resort to going to an emergency room if they feel ill when her office isn’t open or who are worried that their symptoms could be life-threatening. But “before all that,” Meyer suggests they call the BAT phone. Meyer’s office manager, Claree Nanacasse, keeps the phone with her at all times. Meyer estimates that Nanacasse gets three or four BAT phone calls a day.


Cutillo was given the BAT phone number after her blood pressure spiked and she ended up in the emergency room. “It’s made a tremendous difference for me,” she says. “You know when things aren’t working right, I think you have a tendency to overreact. So when I’m not able to control what’s happening to me, I feel myself reacting to that, and then that brings up my blood pressure even more.”
Having the BAT phone number eases anxiety and provides a tremendous sense of security. “I know that someone is there that can help me immediately,” Cutillo says. She recalled one incident when she called the BAT phone, explained what was wrong, and within minutes Nanacasse called back after consulting one of the clinicians in Meyer’s office. Cutillo was instructed to take an additional dose of her blood pressure medicine and call back in an hour to let them know how she was doing. She avoided an emergency room visit — and Medicare avoided a pricey ER bill.
Another time, Cutillo’s blood pressure dipped after a change in her medication. She felt light-headed and fatigued. Cutillo again used the BAT phone and was told to drink some water, eat something salty and elevate her feet above her heart. A half hour later, her pressure stabilized. Nanacasse followed up with Cutillo to see how she was doing and to advise her on what dose of her medicine to take that evening. “This makes you feel that they’re really on top of this condition,” Cutillo says. “It’s kept me out of the emergency room.”

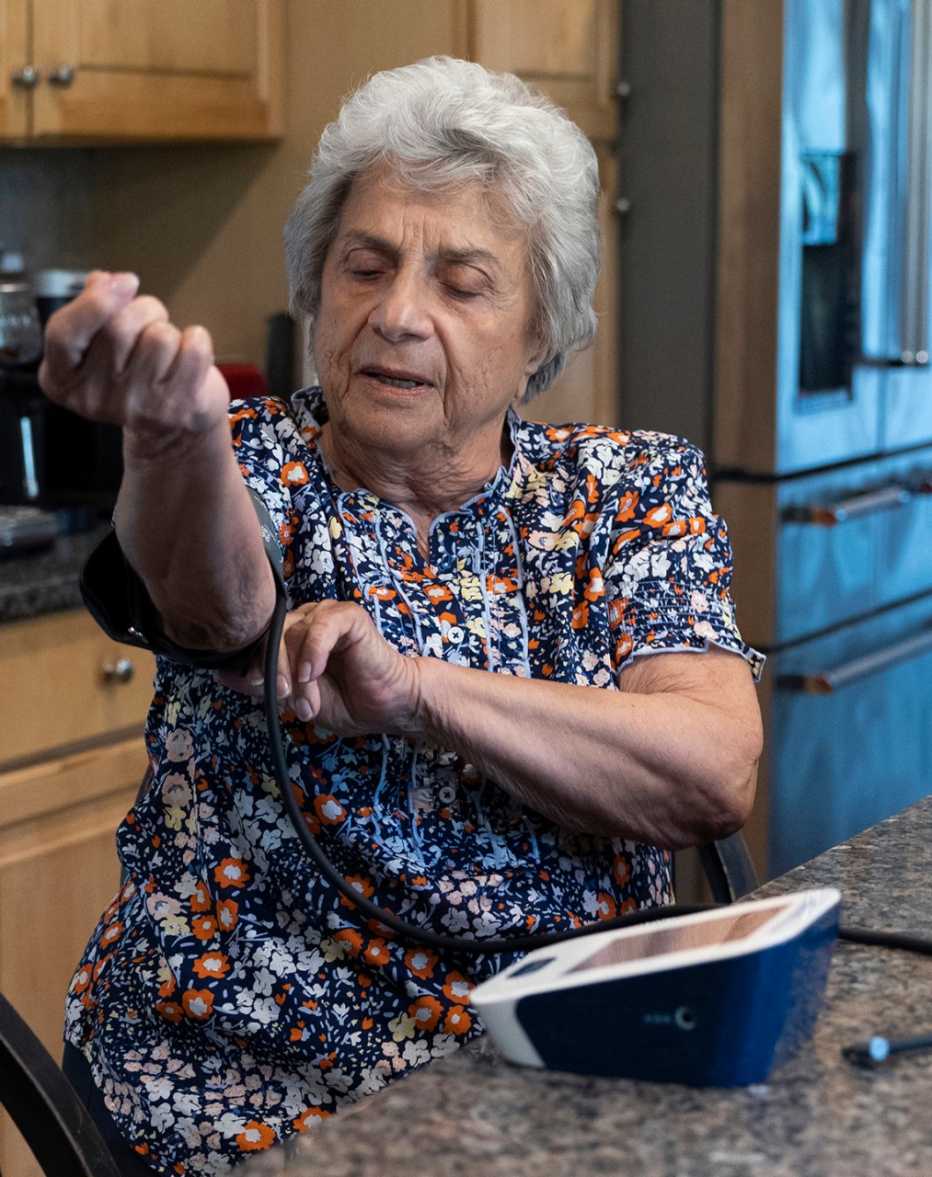
How ACOs work
Nationwide, nearly 14 million of the 66.5 million Medicare beneficiaries get their care from providers affiliated with ACOs, a 3 percent increase in ACO participation over 2023. The latest federal data shows that nearly half of all original Medicare enrollees are now connected to an ACO. ACOs don’t provide the care. Their job is to give physicians the tools they need to better coordinate a patient’s health care and reduce costs.
The Centers for Medicare & Medicaid Services (CMS) has set a goal of having all Medicare enrollees be part of a coordinated care arrangement by 2030. “More coordination between an individual’s health care providers can prevent medical errors and drug interactions while also saving time, money and frustration for the patient,” says Meena Seshamani, M.D., CMS’s deputy administrator and director of the Center for Medicare. In 2021, according to CMS, ACOs in Medicare’s Shared Savings Program, which includes 11 million beneficiaries, saved $2 billion.
ACOs have agreements with Medicare to get data on the claims of the patients of providers who belong to the ACO. The reports that doctors receive include everything from which patients got the preventive screenings they need — such as mammograms and colonoscopies — to which patients went to the hospital.
“We have so much information at our fingertips that we didn’t have before,” Meyer says. “We’re able to see who our sickest patients are. We’re able to see who the patients are that aren’t getting the routine care they need for their diabetes.”


Armed with this information, doctors can follow up with patients who may have missed a screening or whose data shows they need help managing a particular illness.










































































More on Health
Health Spending to Outpace U.S. Economic Growth
Medicare projects the nation's health expenditures will rise 5.4 percent annually over next decade
Feds Crack Down on Medicare Advantage Marketing
Celebrity endorsers must identify whom they represent and not mislead potential MA enrollees
The Big Choice: Original Medicare vs. Medicare Advantage
Which path you take will determine how you get your medical care — and how much it costs