Staying Fit
Since declaring monkeypox a national emergency on Aug. 4, the federal government has accelerated efforts to get a limited supply of monkeypox vaccines to Americans most likely to be exposed to the virus, while also urging the public to take precautions against infection.
The U.S. Department of Health and Human Services on Aug. 15 announced it would release 442,000 doses for state, local and territorial health departments, double what it had previously anticipated, thanks to a plan implemented the previous week to stretch the nation’s limited supply of monkeypox vaccine by giving people a smaller dose that research suggests is nearly as effective at preventing infection. More than 630,000 doses have already been shipped, but federal health officials have suggested they would need about 3.2 million shots to vaccinate all those considered at highest risk of monkeypox, according to the Associated Press.
The Centers for Disease Control and Prevention (CDC) says that since mid-May more than 11,890 probable or confirmed cases have been detected in 49 states, Puerto Rico and the District of Columbia. No cases have been reported in Wyoming. The monkeypox virus is spreading mostly through close, intimate contact with someone who has monkeypox, the CDC says.


AARP Membership— $12 for your first year when you sign up for Automatic Renewal
Get instant access to members-only products and hundreds of discounts, a free second membership, and a subscription to AARP the Magazine.
The World Health Organization (WHO) in July declared the outbreak a global emergency — its highest level of alert. Since May, nearly 90 countries have reported more than 31,000 cases of monkeypox.
WHO Director-General Tedros Adhanom Ghebreyesus made the decision to ensure that the world takes the current outbreaks seriously. California, New York, Illinois, New York City and San Francisco have all recently declared monkeypox a public health emergency, according to The New York Times.
Health officials are urging people who suspect they may have the disease to see a physician and get tested. “Many of these global reports of monkeypox cases are occurring within sexual networks,” Inger Damon, M.D., director of the CDC’s Division of High-Consequence Pathogens and Pathology, said in a statement. “However, health care providers should be alert to any rash that has features typical of monkeypox. We’re asking the public to contact their health care provider if they have a new rash and are concerned about monkeypox.”
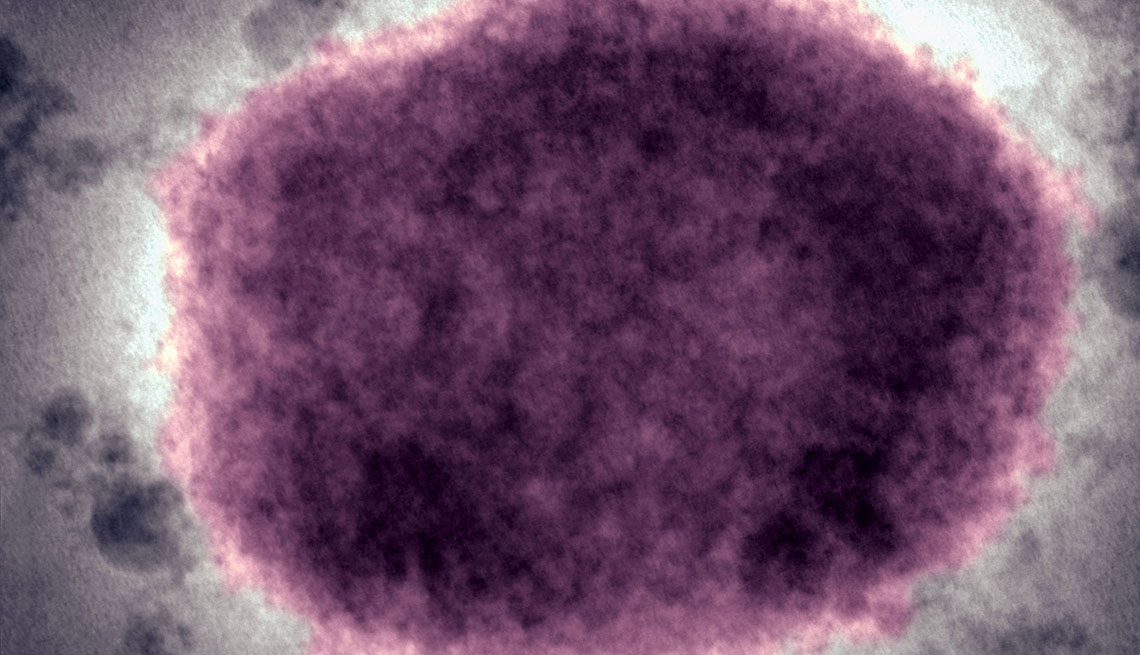
What is it?
A relative of smallpox and cowpox, the monkeypox virus was first discovered in 1958, when two outbreaks of a poxlike disease occurred in colonies of monkeys kept for research, according to the Center for Genome Sciences at the U.S. Army Medical Research Institute of Infectious Diseases. The first human case was recorded in 1970 in the Democratic Republic of the Congo.
The largest previous U.S. outbreak of monkeypox occurred in 2003, when 47 cases were reported in the Midwest among individuals who became ill after having contact with pet prairie dogs that had been housed near a shipment of small mammals from Ghana. Tests confirmed that among those mammals, two African giant pouched rats, nine dormice and three rope squirrels were infected with monkeypox virus, according to the CDC.
What are the symptoms?
Monkeypox symptoms typically begin about a week or two after infection, according to the CDC.