AARP Hearing Center
2 Years of COVID: What Comes Next?
Even with the arrival of omicron, science has shown the smart path forward


If there’s one thing we can safely say after two years of living under COVID-19, it’s this: Science isn’t perfect, but it works.
Public health experts made some mistakes before the true nature of the virus was known, from the initial guidance to forgo wearing masks in public to the advice on wiping down groceries and mail. Indeed, at the start of the pandemic, few experts believed it would be as bad as it’s been, says Cameron Wolfe, M.D., an infectious disease specialist and associate professor at the Duke University School of Medicine.
In February 2020, U.S. doctors who deal with “high-consequence pathogens” and disaster medicine were predicting a worst-case scenario of 500,000 U.S. deaths. But they were wrong. As of this writing, the death toll from COVID has surpassed 834,000 Americans, with more than 59 million infected. Roughly 93 percent of those who have died were 50 or older.
But after two years of both triumphs and missteps, a lot of us have grown frustrated with science. Vaccines are miracles — or they’re not. “Long COVID” is a thing — or it’s not. Omicron, delta and other variants have thrown our best planning and predictions into chaos time and again. And across the country, public health practices are more and more driven by politics, media and culture rather than by science.
It’s confusing. And depressing. And as a result, COVID fatigue has become a real danger to our collective health.
“People are tired of the public health interventions,” says Andrew Badley, M.D., chair of the Mayo Clinic’s COVID-19 Research Task Force. “Masking and social distancing and handwashing and not going to crowded settings. Some people are doing that less and less, and I think that contributes to the spread.” Because we’re letting our guard down, “I think we will be seeing patients with severe COVID disease for years to come,” he says.
So as the two-year anniversary of COVID rolls around, let’s take a step back, get a solid look at just where we are, and answer some serious questions about the future of COVID and how to make 2022 as healthy, safe and productive as it can be.
1. If COVID vaccines are “90 percent effective,” how come so many vaccinated people get sick?
Until the omicron variant emerged, “breakthrough” infections in immunized individuals were rare, according to the Centers for Disease Control and Prevention (CDC), and they happened primarily in those who were immunocompromised. It appears that omicron has a greater ability to circumnavigate the initial vaccine series than other variants. Omicron makes it even more urgent not just to get vaccinated but to add a booster if you have not already done so, and to take extra precautions, especially if you’re over 65 or dealing with any chronic health conditions.
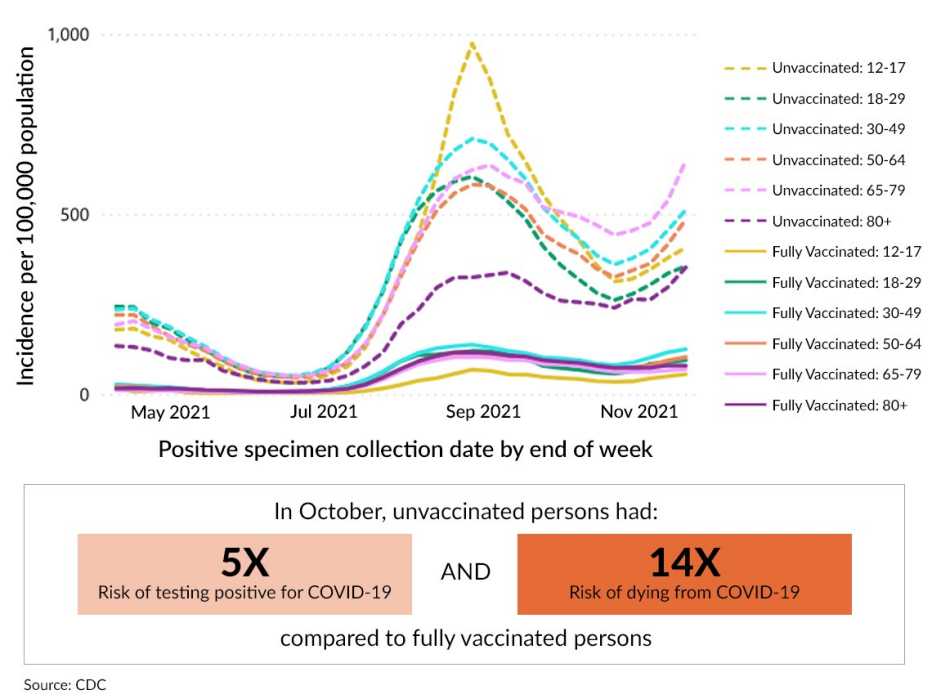
Here are the CDC statistics to keep in mind: Compared to people who are fully vaccinated with a booster, unvaccinated people are 10 times more likely to catch COVID and 20 times more likely to die from it. And for those 50 and older, the risk of forgoing vaccination is even greater.
The fact is, all vaccines — measles, shingles, influenza, pneumonia, what have you — vary in their effectiveness, says Paul Duprex, director of the Center for Vaccine Research at the University of Pittsburgh.
“The goal set for COVID-19 vaccines to be considered effective was 50 percent; they surprised us by hitting over 90 percent.” By comparison, our annual flu shots come in at around 40 to 60 percent each year. So the range of effectiveness of the COVID vaccines really is remarkable.
“Your immune system is like a football team,” says Panagis Galiatsatos, M.D., a pulmonologist and critical care specialist at the Johns Hopkins University School of Medicine. “You practice all week, but you have no idea what exactly you’ll be up against on Sunday. Even with the strongest players, you don’t know how well you’ll play against a team you’ve never seen before. A vaccine gives your football team the opponent’s playbook. So you’re gonna go out there and be more effective.”
That doesn’t mean the other team can’t occasionally win or that you can’t still get sick. But getting vaccinated dramatically stacks the odds in your favor and makes any illness you do experience much less severe.
Rates of COVID-19 Cases by Vaccination Status and Age Group
An interactive version of the CDC's chart is available here.

2. Why do we need COVID boosters? Is this proof that the vaccines don’t work?
It’s entirely normal for antibodies generated by vaccines to wane over time and require a boost, as anyone who’s gotten a tetanus shot after a puncture wound can attest. “What we know is that even after two COVID immunizations, our antibody levels drop; that’s why we need boosters,” Duprex says. “Likewise, when variants like omicron come along, these antibodies don’t seem to be as effective. That’s a double hit which leads to drops in vaccine effectiveness. This virus isn’t going away ... boosters are very likely here to stay.” The booster restores the vaccine to about 80 percent effectiveness against omicron.
Even natural immunity fades with time, as in the case of chicken pox: After a childhood bout of chicken pox, our immune system keeps the virus in check for decades. But after age 50, the immune system begins to fatigue, which is why we vaccinate for shingles — the disease caused by a reemergence of the chicken pox virus.
The fact is that the virus is changing, and our approach to it has to change as well. Omicron has shown itself to be more capable of evading vaccine-granted immunity given by the first two jabs, but boosters appear to be effective against it. That’s why getting a booster — and protecting yourself if your health is compromised — is so critical. The CDC now recommends the Pfizer-BioNTech booster five months after your last dose, rather than the original six months.
3. Do new COVID pills “cure” the disease?


“Do drugs work as effectively as vaccination? Heck no,” says Duke’s Wolfe. But they’re still a potentially important development.

Two strong antiviral drugs developed to fight COVID have received emergency use authorization from the FDA. Merck’s molnupiravir has been shown to lower the risk of severe symptoms and death by 30 percent. Meanwhile, Pfizer revealed study results in November showing its drug Paxlovid reduced hospitalizations and deaths by 89 percent. Even better news: Both come in easy-to-take pill form, although supplies at present are limited.
The drugs are designed to be taken by people experiencing mild to moderate symptoms within the first few days of the disease cycle. The pills work in a different way than monoclonal antibodies, until now the go-to COVID treatment, but the outcome is the same: They prevent the virus from replicating in the human body and thus keep symptoms of the disease from escalating.
These drugs are serious medical advances, not just because of their effectiveness, but because of their convenience. Other inexpensive and plentiful treatments are beginning to show promise as well. Preliminary research, for example, has shown that the cholesterol drug fenofibrate may help prevent the COVID spike protein from binding with human cells, reducing infection. Meanwhile, the antidepressant fluvoxamine has also shown promise in preventing an immune system overreaction — out-of-control inflammation — and could lower the risk of hospitalization and death.
These drugs are cheap, plentiful and established — though neither is widely used for COVID just yet. But the better bet is to follow safety precautions and avoid infection in the first place, Wolfe says.
4. Why aren’t we at herd immunity yet?
“Herd immunity” occurs when a large enough portion of a community becomes immune to a disease that its spread from person to person becomes unlikely. How high that portion needs to be is based largely on how contagious the disease is; the more easily it spreads, the more people you need to be immune to contain it. Measles is highly contagious, so roughly 94 percent of a population needs to be immune to shut off the chain of transmission.
As to COVID, science hasn’t yet determined the threshold, but estimates put it at north of 90 percent of the population. For the older population, vaccination hasn’t been an issue — though you’d think it was, based on public debate. As of early January, 88 percent of those 65-plus were fully vaccinated, and nearly 60 percent had gotten a booster. But the fully vaccinated population over age 18 is only about 73 percent. That’s helpful, but not enough for herd immunity. Plus, rates vary from state to state or even county to county. So even if we reach herd immunity in some parts of the country, that immunity won’t hold. As long as we have areas of lower vaccination rates, we will still have COVID spread.
So what keeps people from getting a shot? A 2021 study by the Ad Council found a combination of distrust of institutions like government and the pharma industry; doubts about vaccines’ effectiveness; safety concerns, particularly around future pregnancies; and the feeling among younger people that they simply weren’t at real risk.
“Some parts of the country have had high vaccination rates and reasonable cooperation with masks and risk-reduction strategies and have benefited by a decline in COVID,” says Sten Vermund, M.D., dean of Yale University’s School of Public Health. “Places that don’t are experiencing continued transmission.”
In some cases, vaccine mandates have helped people who need a nudge. Doctors speak of two categories of unvaccinated people: the vaccine resistant (“No way I’m getting a shot!”) and vaccine hesitant. The hesitant can be convinced, Vermund says. “Principles can be very strongly held or mildly held. Some will never agree regardless of the consequences and are willing to lose a job. Other people don’t have as deeply held a view. That’s where we’re making progress.”
The numbers bear this out — and that’s why vaccine mandates, as unpopular as they may be, have been so effective. When United Airlines issued a mandate for all employees, fewer than 1 percent faced dismissal for noncompliance. Novant Health, a hospital system in North Carolina with 35,000 employees, had to dismiss only 175 for noncompliance. In Washington state, less than 3 percent of the 63,000-person state workforce chose to quit or be fired rather than get the vaccine.
“It’s like car insurance,” Wolfe says. “If we didn’t make it mandatory, a lot of people wouldn’t get it because it costs money and we all think we’re great drivers who will never have a car crash.” The vaccine resistant may never get that shot, even though 50 million people have gotten COVID. But vaccine mandates so far have helped “insure” millions against future infection. That’s good progress.
5. What is long COVID — and how do I know if I’m at risk?
We’ve learned much about this novel virus over the past two years, but one aspect that continues to confound doctors is “long COVID,” in which certain patients suffer from symptoms for months after the infection has run its course.
Many other viral diseases — from chicken pox to polio to influenza — have been shown to have “long haul” effects, as do bacterial diseases like Lyme. But long COVID may be far more common than anyone thought.
A large study in PLOS Medicine of more than 273,000 COVID survivors found that 37 percent had one or more symptoms of long COVID three to six months after infection. And the risk of long COVID symptoms rose with age, with 61 percent of the 65-plus group having symptoms like breathing difficulty from lung damage, cognitive issues (brain fog and memory), muscle pain and fatigue. The risk was higher in people who’d had a more severe bout of the illness. Other common long-term symptoms include headache, anxiety/depression and pain in the chest or throat that people may not even attribute to COVID.
The overall cause remains a mystery, but researchers are making inroads. A new study of deceased COVID patients by the National Institutes of Health found the COVID virus can infect specific organs — such as the heart, lungs or brain — and persist there for months. But there is still much to learn.
“We don’t yet have a great understanding of what this is, how it occurs and what the treatment should be,” Badley says. “I think in 2022, we’ll begin to get a handle on those.” What makes it especially challenging is identifying which symptoms are actually long COVID and which aren’t. “It’s very nebulous,” Wolfe says. “I can predict with some accuracy who’s going to get sick enough with COVID to wind up in the hospital. It’s proportional to your age, your weight, to how bad your heart or lungs are at the beginning, how bad your diabetic control is. I have yet to find a good way of predicting who gets long COVID. I have no idea how that pans out.”
If you have had COVID and have ongoing symptoms, Badley suggests talking to your doctor immediately. Everyone presents differently, and the long-term effects of COVID remain a mystery. But there’s another reason to talk to your doctor: Your symptoms might not be COVID-related.
“Many people deferred routine health care maintenance during the COVID era,” Badley says. “Some of these symptoms we’re seeing after recovery could be unrelated health issues.”
Lung and neurological issues are particularly worrisome, as they may require a specialist’s care.Vaccines may play a part here, as well. A U.K. study in The Lancet found that long COVID risk was reduced by half in vaccinated folks who developed breakthrough infections. Also, though anecdotal, a Yale research team found that receiving the vaccine reduced long COVID symptoms in 40 percent of people surveyed — possibly because the inoculation took out some remaining viral factors.
Bottom line: Ask yourself, “Am I worse off health-wise than I was before COVID?” If yes, call the doctor.
6. Is omicron really a game changer?
The delta variant was responsible for the massive outbreak in the summer of 2021, and omicron has caused a much greater spike. But while these variants seem to be more communicable than the original virus, those who are fully vaccinated and had a booster are still far less likely to experience a severe infection.
“The more viral replication you have in the community or in an individual, the more likely you are to see mutations occur. So absolutely, I believe we will see new variants moving forward,” Badley says.
But even if a vaccine-resistant variant does emerge, “the vaccine manufacturers can develop new vaccines to these new strains very, very quickly because they know exactly how to do it,” Yale’s Vermund says. An omicron-specific vaccine has not been necessary, but if the situation changes in the months or years to come, experts suggest a new mRNA vaccine could be created within a few months.
7. I’m vaccinated. Is there anything else I can do?
First off, get your flu vaccine (it’s not too late) and a COVID booster if it’s been five months since your second Pfizer shot (six months if you got the Moderna series; two months if you got the Johnson & Johnson vaccine). The two vaccines can be given simultaneously (you might want to get one in each arm) and function so peacefully together that drugmakers are working on a single flu-COVID combo vaccine that could be available in autumn 2022. The goal is to stay healthy and out of the hospital — and prevention is your best weapon, Badley says the first “flurona” case of someone having the flu and COVID at the same time has been confirmed in Israel.“
"Last year, we were pretty good at distancing and masking and handwashing,” he adds. “Now in many places, that’s relaxed and the opportunity for influenza spread will be back to where it was pre-pandemic.” So while you’re probably tired of wearing a mask, experts say you should wear one in indoor public spaces.
And continue to follow the advice of your health care provider. Just as vaccines against other diseases need periodic boosting, COVID boosters may become a regular part of your health plan.
8. What will 2022 bring?
One way to analyze what might happen later this year is to look at what the people who have the most skin in this game are planning. In this case, that’s health insurance companies. Insurers offering health plans via the Affordable Care Act marketplaces must file plan offerings for 2022 to justify their premiums. Most ACA marketplace insurers are predicting COVID-19 will have no effect on their 2022 costs.
That’s a bold and optimistic statement about the future of this pandemic. But the virus is still out there. COVID is still most dangerous for people 50 and older, and real safety has remained elusive.
“I think we’re going to get there [in 2022] in certain parts of the country,” Vermund says. “I think you’re going to have a very favorable circumstance because you have very high vaccine rates. In places where we’re only getting 40 or 50 percent of adults vaccinated, that’s a long way from herd immunity. And if people similarly resist vaccination for their children, you’re going to have a big chunk of the population in whom the virus is going to continue to circulate.”
Wolfe, a native Australian, has faith in Americans. “I’d be wrong to say I’m not optimistic. We know so much more than we knew a year ago. We have far better treatments. We understand distancing and masking. People can do it. We’re absolutely better than we were a year ago.”
A Mask Hater’s Guide to Masking
Two years later, masks remain a critical weapon for keeping COVID in check. “We know how this spreads,” says Johns Hopkins’ Panagis Galiatsatos, M.D. “You have to breathe it in after someone actively breathes it out. The vaccines work even better if you inherit a small viral load. And if you should breathe in the virus, you’ll get a smaller viral load if both you and the other person are masked.”
Mask rules for early 2022 are:
Vaccinated
If you’ve had a booster in the past two months, have no chronic health issues, and are under age 65, you could consider going without a mask:
- When attending an outdoor event
- When gathering indoors with others who have been fully vaccinated or had negative COVID tests in the past two days
- But mask up when indoors with the general public. The transmissibility of the omicron variant means overall risk is elevated. AND … if you feel unsafe in any situation, make the smart move and don a mask.
Unvaccinated
If you’re over 50 and have not been fully vaccinated, consider yourself at high risk —even if you’ve had COVID in the past. You still need to wear a mask:
- Anywhere indoors in public, or outdoors when in crowds
- Particularly in hospitals, nursing homes or other facilities housing vulnerable populations
- When entering areas where mask mandates are in place.
Just think of masks this way: “I look at wearing masks no differently than wearing a helmet to enjoy a motorcycle ride,” Galiatsatos says. “You are just being safe."


































































More on health
How the Pandemic Will Be Different in 2022
Expect new treatments, more testing and additional variantsGetting a Lifesaving COVID-19 Vaccination
Vaccines crucial for people 50-plus amid COVID-19 risks