Staying Fit

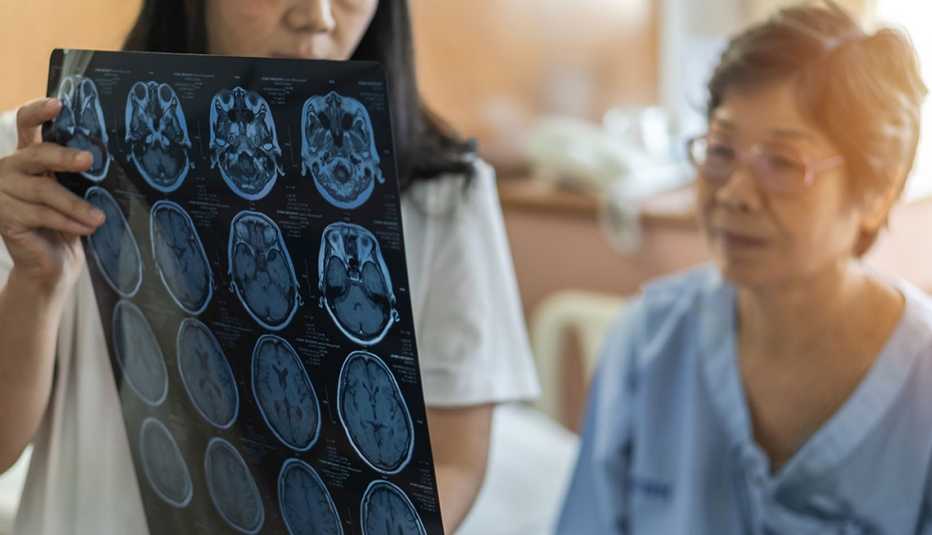
Blacks, Hispanics and Asians are less likely to receive a timely diagnosis of early dementia than whites, according to a study of California Medicare claims.
"Our findings highlight substantial gaps in diagnostic care among racially diverse older adults that are likely associated with underrepresentation in clinical trials and inequities in treatment,” the researchers wrote in a study published in JAMA Neurology. “Major policy and practice efforts are necessary to address these gaps via targeted interventions for vulnerable populations.”


AARP Membership— $12 for your first year when you sign up for Automatic Renewal
Get instant access to members-only products and hundreds of discounts, a free second membership, and a subscription to AARP the Magazine.
Researchers analyzed claims filed by 10,472 Medicare fee-for-service beneficiaries who received a diagnosis of either incident mild cognitive impairment (MCI) or dementia in the first six months of 2015 in California. While 23.3 percent of white beneficiaries received a first diagnosis of MCI, that was true of just 12.3 percent of Asians, 15.8 percent of Hispanics and 18.2 percent of Blacks.
They also found that Asians were significantly less likely to receive as comprehensive a diagnostic screening as whites, for example, with only 28.8 percent of Asians receiving a specialist evaluation compared to 35.4 percent of whites.
Early intervention important
Two of the study researchers, Katherine Possin, an associate professor of neurology at the Global Brain Health Institute at the University of California San Francisco (UCSF), and Elena Tsoy, a postdoctoral fellow in neuropsychology at UCSF's Memory and Aging Center, explained via email the importance of early intervention when it comes to brain health.
"When dementia diagnosis is delayed, there are missed opportunities for good care. This includes the identification of reversible causes, timely treatment of cognitive symptoms, and supportive care for families. With new treatments for Alzheimer's disease and other dementias on the horizon, these delays in diagnosis — if left unaddressed — will further deepen inequities in treatment,” they said.

































































More on health
Dementia's Gender Disparity: Report Uncovers Unique Challenges Facing Women
Plus, tips on how to reduce dementia risks and ease the caregiving burdenThe Alzheimer's Drugs Showing Early Promise
Along with Eli Lily’s donanemab, researchers say several new therapies offer hope