Staying Fit
How many times in the past year have you used the phrase “when COVID is over…"? Unfortunately, while COVID-19 may well become a less serious threat, a future free of the coronavirus isn't on the near horizon, experts say — even with a vaccine. “We're pretty sure that this virus is something we're going to have to live with for the foreseeable future,” says William Schaffner, M.D., professor of infectious diseases at Vanderbilt University Medical Center.
Why COVID-19 is likely here to stay
History shows that it's nearly impossible to eradicate any infectious disease, says John Wherry, director of the Institute for Immunology at the University of Pennsylvania. Humans have only managed to do it once, with smallpox. Other viral diseases, like measles, have been nearly eliminated in the U.S. through vaccination, because the shots induce something called “sterilizing immunity.” That means that vaccinated people can't get infected or spread the disease.


AARP Membership— $12 for your first year when you sign up for Automatic Renewal
Get instant access to members-only products and hundreds of discounts, a free second membership, and a subscription to AARP the Magazine.
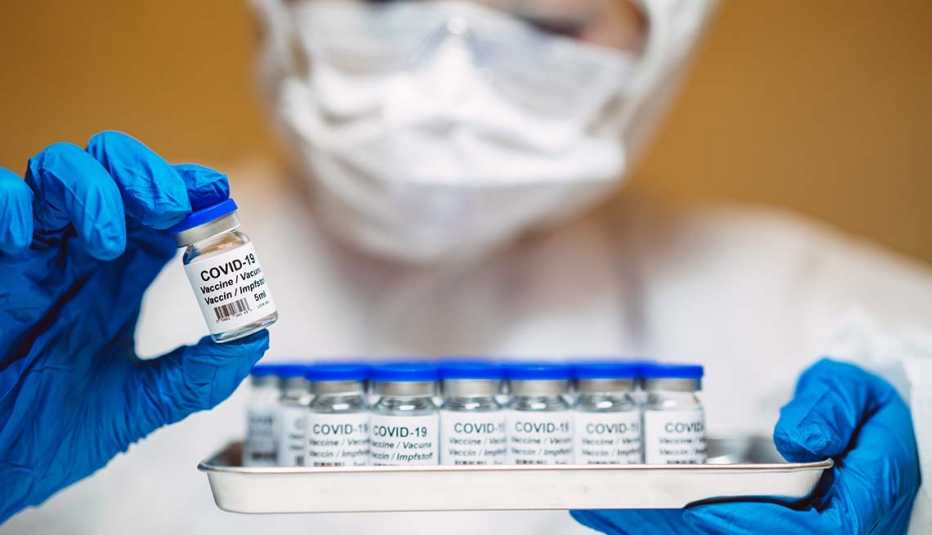
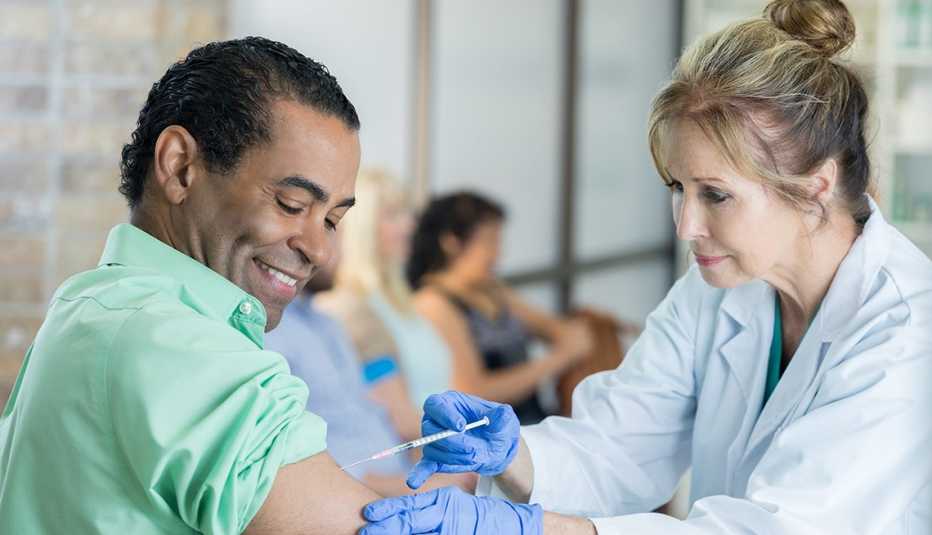
That's not the case with COVID-19, says Clare Rock, M.D., associate professor of medicine in the Division of Infectious Diseases at Johns Hopkins School of Medicine. As she explains, both the COVID and influenza vaccines “don't produce that sterilizing immunity, which means people can still get mild infections. Although we still don't know whether they can pass infections on to others.” The COVID-19 vaccine has been shown to be highly effective at preventing illness and protecting people from serious complications or hospitalization. So a major downtick in deaths and hospitalizations is expected as more and more people roll up their sleeves. Still, “this is not a vaccine that's going to eradicate COVID,” Rock says.
And there are other factors, like how many people choose to get vaccinated or whether variants of the virus emerge that are resistant to the vaccines, which could influence the persistence of the disease. Every time the virus spreads from person to person, it accumulates changes in its genetic code.
"More virus replication leads to more variants,” Wherry says. “The vast majority of those variants are dead ends, but you're playing a game of Russian roulette. The more bullets there are in the gun, the more likely something bad is going to happen.” The big worry, of course, is that a variant arrives that can bypass vaccine-induced immunity.