AARP Hearing Center
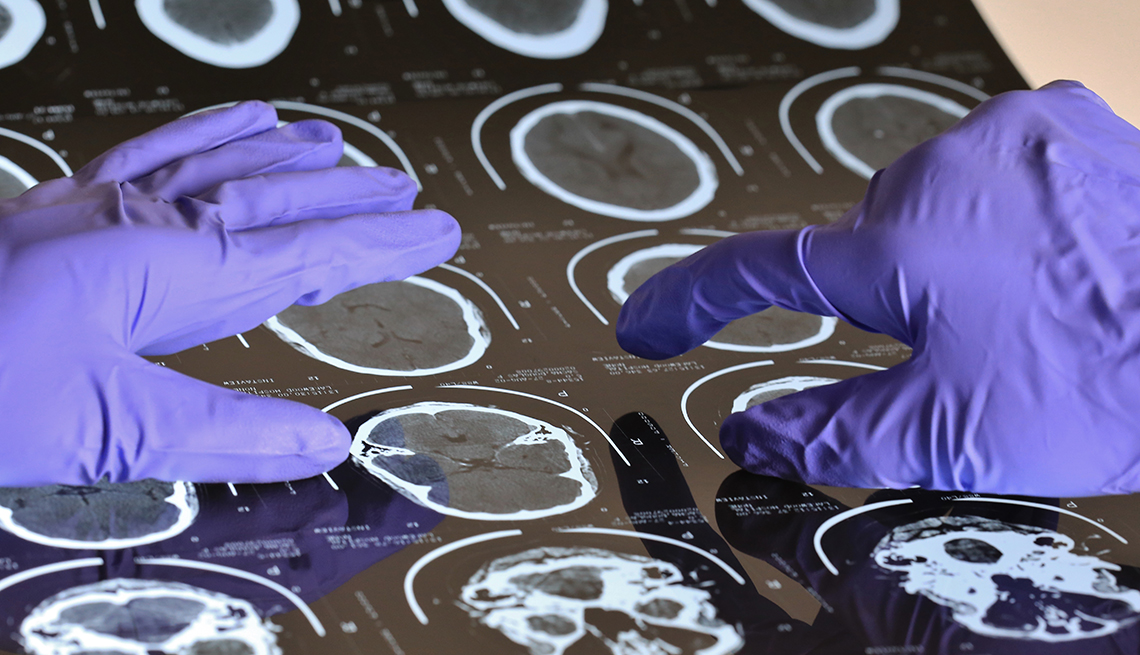
One of the most mysterious and frightening consequences of COVID-19 is its impact on the brain.
Over 80 percent of hospitalized COVID-19 patients have neurological symptoms, a Northwestern Medicine health system study found. Even patients who have mild cases of COVID-19 have reported memory loss, trouble focusing and other related problems that can last for months.
Now, some scientists say there is compelling evidence that the negative effects of the virus could last even longer, possibly creating a surge of cases of dementia and cognitive decline years down the road.
"It's possible — I'd even say it's probable — that having COVID-19 will increase your risk of dementia,” said Gabriel de Erausquin, M.D., a professor of neurology at the University of Texas Health Science Center at San Antonio. “We just don't have enough information yet to answer that question with certainty.”
A global study to find answers
De Erausquin and other researchers have launched a large-scale, global study to investigate the short- and long-term impact of COVID-19 on the brain, including the ways in which it may contribute to Alzheimer's disease and other dementias.
"We want to be out in front of this to minimize the impact, predict who is most at risk and try to identify behaviors or other factors which can help us reduce the impact in older patients,” de Erausquin said.
With funding from the Alzheimer's Association and technical guidance from the World Health Organization (WHO), the study will track more than 40,000 patients age 50 and older, with the first results expected in early 2022.
"The creation of an international group of scientists to further study the virus’ impact on the brain and share information is critically important,” said Sarah Lenz Lock, executive director of AARP's Global Council on Brain Health. “We also need to learn how to better avoid the risks and mitigate the harms of the virus to reduce cognitive decline and dementia in the future."