AARP Hearing Center
I Had Cancer: Do I Need a Third COVID Vaccine Shot Now?
Many, but not all, patients and survivors qualify for an extra dose. Here’s how to decide

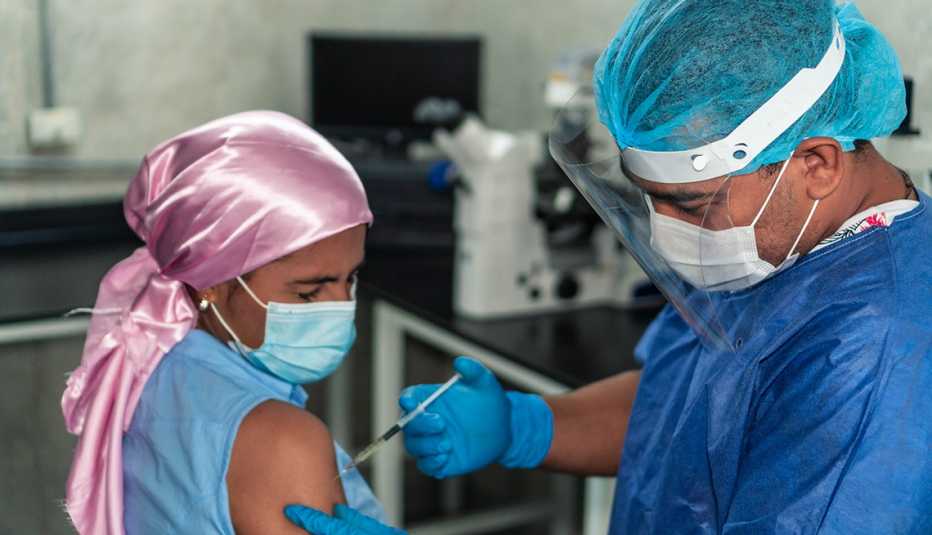
Gary Schiller has been inundated with inquiries from cancer patients about whether they should get an additional dose of the Pfizer-BioNTech or Moderna COVID-19 vaccines.
"There is not a day that goes by that we don't get multiple questions,” said Schiller, M.D., a professor of hematology-oncology and director of the bone marrow and stem cell transplant unit at the University of California, Los Angeles (UCLA).
Other health care providers echo similar experiences, including Meghan Baker, M.D., a hospital epidemiologist who works with immunocompromised patients at Dana-Farber Cancer Institute and Brigham and Women's Hospital in Boston. Ever since federal health officials announced on Aug. 13 that people with moderately to severely weakened immune systems should get a third dose of the mRNA vaccines, she has been trying to keep up with patient questions and requests.
The reason: Many, but not all, cancer patients and survivors are considered immunocompromised. And studies show that the typical two-dose vaccine series doesn't produce the same high level of protection in immunocompromised individuals that it does in people with healthy immune systems. But a third shot — not to be confused with the forthcoming booster shot for the general population — gives the immune system the jump it needs to mount a stronger defense against COVID-19. This is especially important for a population already at greater risk for serious illness from COVID-19 as the highly contagious delta variant burns through the U.S.
Who is considered immunocompromised?
Anyone receiving active treatment for tumors or cancers of the blood should get a third shot of the Pfizer or Moderna vaccines at least four weeks after the second shot, according to the Centers for Disease Control and Prevention (CDC). What does that mean, exactly?
"When you say tumors or cancers of the blood, that will pretty much cover all different types of cancer,” Baker explains. And active treatment generally pertains to patients who are “seeing their oncologist on a regular basis,” she adds. So if you are currently seeking care for cancer, talk to your doctor about getting a third shot.
Who Needs an Additional COVID-19 Vaccine?
Currently, CDC is recommending that moderately to severely immunocompromised people receive an additional dose. This includes people who have:
- Been receiving active cancer treatment for tumors or cancers of the blood
- Received an organ transplant and are taking medicine to suppress the immune system
- Received a stem cell transplant within the last two years or take medicine to suppress the immune system
- Moderate or severe primary immunodeficiency (such as DiGeorge syndrome, Wiskott-Aldrich syndrome)
- Advanced or untreated HIV infection
- Active treatment with high-dose corticosteroids or other drugs that may suppress your immune response
Source: CDC


Some individuals who are past the active treatment phase, however, are also considered immunocompromised and may benefit from a third vaccine dose. The experts at the University of Texas’ MD Anderson Cancer Center tell AARP that individuals who have completed immunosuppressive cancer therapy in the past year are eligible for an additional shot. (Immunosuppressive therapy includes chemotherapy, radiation, high-dose corticosteroids and other drugs that impair the immune system, including rituximab.)
And people who have had a stem cell transplant or have received CAR T therapy — a treatment where some immune system cells are manipulated so they will attack cancer cells — within the last two years qualify for a third vaccine dose as well, writes Mini Kamboj, M.D., chief medical epidemiologist at Memorial Sloan Kettering Cancer Center in New York. Cancer patients who received an organ transplant and are taking medicines that suppress the immune system also meet the criteria.
However, if you have a solid tumor that is under observation only or if it was treated with an intervention such as hormone therapy, targeted therapy or surgery, you may not be considered immunocompromised, Kamboj notes. Some types of radiation are also less likely to impact the immune system. But everyone's case is different, and “the definition of immunocompromised is difficult” to define, Schiller says.
That's why the CDC recommends talking to your doctor about whether a third dose is appropriate. If it is, your health care provider can help determine the best time to get the shot to ensure it gives you the optimal immune response.
What to expect if you get a third shot
Pharmacies, health care centers, hospitals and other locations offering the COVID-19 vaccines can administer the third dose. A doctor’s note is not required, and like the first two shots, there is also no out-of-pocket cost to receive the third one.
Just keep in mind that more is not necessarily better, even for people with weakened immune systems. The CDC warns that individuals should not receive more than a total of three mRNA vaccine doses at this time. The agency is also advising people to get the same vaccine they had the first time — in other words, don't mix and match the Pfizer and Moderna vaccines if you can help it. However, “if the mRNA vaccine product given for the first two doses is not available or is unknown, either mRNA COVID-19 vaccine product may be administered,” the CDC says.
If you were originally vaccinated with the one-shot Johnson & Johnson vaccine, also known as the Janssen vaccine, you'll have to hold off on getting an additional dose for now. Health officials say they are waiting on more data before issuing a recommendation on extra doses for immunocompromised people.
Schiller says people who get a third shot shouldn't expect any new or concerning side effects — and they may even experience diminished symptoms the third time around. Reported reactions are in line with those observed in the two-dose series, the CDC says. Fatigue and pain at the injection site are the most commonly cited side effects of a third dose and, overall, most symptoms are mild to moderate.
And remember: While an extra shot may offer better protection against COVID-19 in people who are immunocompromised, it is not a suit of armor. Preventive measures such as mask wearing, physical distancing, hand washing and avoiding poorly ventilated indoor areas are still recommended — “especially considering the number of cases of COVID that are in the community right now,” Baker says. People who are immunocompromised should also encourage their close contacts to get vaccinated, she adds.


































































MORE ON HEALTH
Pandemic Habits and Breast Cancer Concerns
Experts express concern about women drinking and eating more while exercising less