Staying Fit

It's official: Hydroxychloroquine is a bust. After months of hype, disappointing clinical trials ultimately led to the Food and Drug Administration (FDA) revoking the drug's emergency use authorization last week. Some physicians weren't surprised: Many had stopped using it long before the FDA announcement, as research failing to support its efficacy for COVID-19 was beginning to mount.
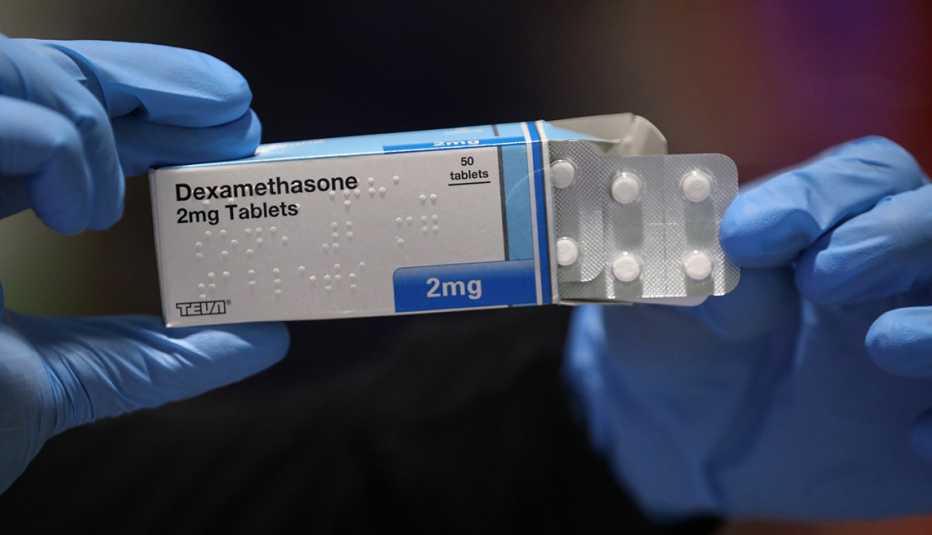
The day after FDA stopped cold the use of hydroxychloroquine, British researchers at Oxford University announced their success treating high-risk COVID-19 patients with a common steroid, dexamethasone. According to their as-yet published research, the drug, already used for conditions such as arthritis or skin disorders, appears to be the first treatment to significantly lower the risk of death for patients on ventilators. For those on oxygen, it cut deaths by even more.


AARP Membership— $12 for your first year when you sign up for Automatic Renewal
Get instant access to members-only products and hundreds of discounts, a free second membership, and a subscription to AARP the Magazine.
In the ongoing day-to-day treatment of COVID-19, doctors say that most people who contract the virus don't need anything beyond a fever-reducer like acetaminophen, plenty of rest and maybe some chicken soup. Figuring out how to best treat the smaller yet significant group that becomes very ill, however, remains challenging.
"We really have not identified anything that's effective and should be used on a routine basis,” says Neil Schluger, M.D., chief of the Division of Pulmonary, Allergy and Critical Care Medicine at Columbia University Irving Medical Center. He states that for those who need hospitalization, “mostly what we're doing is giving oxygen and making sure patients have adequate hydration and nutrition."
About 80 percent of the time, this kind of “supportive care” is sufficient, he says. Those in the unlucky 20 percent (who tend to be older than 60 with underlying conditions) will likely receive one or more of the following treatments.
Mechanical ventilation
When patients develop one of the most deadly aspects of COVID-19, acute respiratory distress syndrome, “the only proven therapy that changes the outcome is low-volume ventilation,” says Ivan Rosas, M.D., chief of the pulmonary, critical care and sleep medicine section in the Department of Medicine at Baylor College of Medicine. Patients who require a ventilator — which pumps oxygen into lungs and removes carbon dioxide — first have to be intubated, which entails putting a tube down the throat and into the windpipe.
Although ventilators don't treat the underlying infection, they can sometimes keep a patient alive long enough to recover while their immune system and/or drugs fight off the virus. “We've had 82-year-olds on ventilators who we've gotten off ventilators,” Schluger says.
That said, younger patients tend to face much better survival odds on the machines than those over 80 do, according to research that includes a recent Lancet study. Physicians are increasingly attempting to keep more older patients off ventilators with an approach that combines proning (see below) and a specific type of oxygen delivery known as nasal cannuluas.

































































More on health