Staying Fit
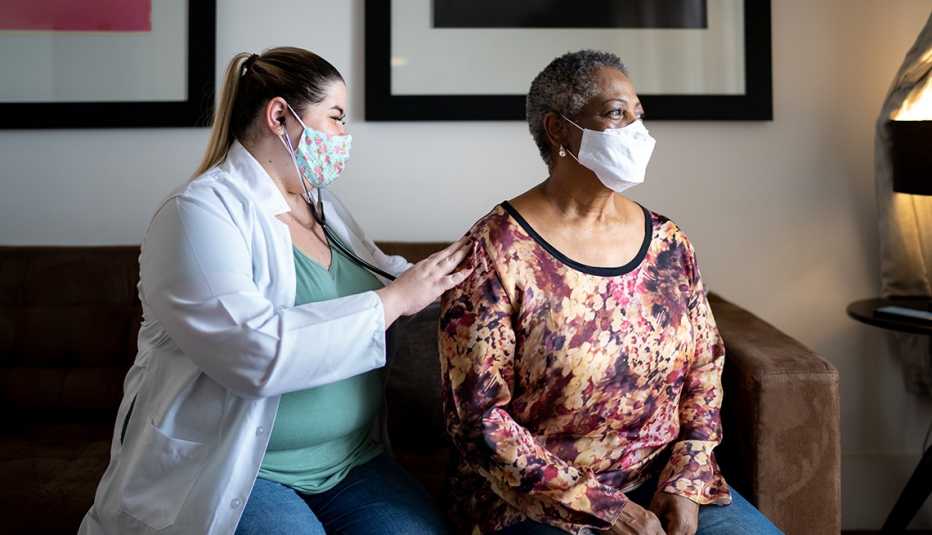
AARP on Thursday called on U.S. nursing homes to require COVID-19 booster shots for their residents and staff, as infection rates among both groups hit new highs and as booster rates in nursing homes lag, particularly in certain states.
“The message from recent data is clear: Nursing home residents and staff need booster shots now,” Susan Reinhard, AARP senior vice president and director of the AARP Public Policy Institute, and Ari Houser, a senior methods adviser at the Institute, wrote in a blog post on Thursday.


AARP Membership— $12 for your first year when you sign up for Automatic Renewal
Get instant access to members-only products and hundreds of discounts, a free second membership, and a subscription to AARP the Magazine.
New weekly data from the Centers for Disease Control and Prevention (CDC) show a rapid surge in cases among nursing home staff beginning late last month. Weekly cases among workers jumped more than 10-fold from the week ending Dec. 19 to the week ending Jan. 9, from some 6,000 to 67,000 new infections. Cases seem to have dropped slightly last week, to 58,000 new inflections, according to data released on Wednesday, but that’s still more than double the cases reported during last winter’s peaks. And that figure is likely an undercount, as data continues to be submitted.
Check the vaccination rates of your nursing home
You can now find vaccination rates of both residents and staff at any Medicare-certified nursing home and compare it with state and national averages on Medicare.gov’s Care Compare website.
- Find a nursing home’s profile via the home page’s search function
- Visit the “Details” section of its profile
- Click the “View COVID-19 Vaccination Rates” button
Resident cases are surging, too. They jumped from roughly 6,000 new infections during the week ending Dec. 26 to 42,000 last week, which is likely an undercount. Those infection rates surpass those of last winter, the deadliest period on record for nursing home residents, when some 40,000 died in just two months.
More than 160,000 nursing home residents and workers nationwide have died from COVID-19, accounting for roughly a fifth of the nation’s total COVID deaths.
While the current rate of resident deaths is well below that of last winter, it is rising. Deaths have recently more than doubled, from around 500 for the week ending Jan. 2 to around 1,000 last week.