Staying Fit
No period on record has been more deadly for American nursing homes, where more than 158,000 residents have died from COVID-19, than last winter. Roughly 1 in 45 nursing home residents died in a four-week window between early December 2020 and early January 2021; around 24,000 residents perished.
Those months were “so terribly tragic,” says Lori Smetanka, executive director of the nonprofit National Consumer Voice for Quality Long-Term Care. “We can't go back there.”


AARP Membership— $12 for your first year when you sign up for Automatic Renewal
Get instant access to members-only products and hundreds of discounts, a free second membership, and a subscription to AARP the Magazine.
But experts warn that an array of new risks for the highly vulnerable nursing home population — including the current record-high community transmission, lagging booster rates, severe staffing shortages, a pause on President Joe Biden’s vaccine mandate for health care workers and even the return of visitors — could result in another major surge of illness and carnage this winter.
Even though nursing homes have much more effective tools to tackle the virus today than last winter, including vaccines and boosters, better masking, new treatments and more knowledge of how COVID-19 spreads, there are also signs of more trouble emerging.
Check the vaccination rates of your nursing home
You can now find vaccination rates of both residents and staff at any Medicare-certified nursing home and compare it with state and national averages on Medicare.gov’s Care Compare website.
- Find a nursing home’s profile via the home page’s search function
- Visit the “Details” section of its profile
- Click the “View COVID-19 Vaccination Rates” button
The risks are “a recipe for a disaster,” says Michael Wasserman, a geriatrician and past president of the California Association of Long Term Care Medicine. “And if we all don’t act right now to address them, another disaster is, I’m sorry to say, what’s going to unfold.”
Rapidly rising cases
The spread of COVID-19 in nursing homes tends to follow spread in the surrounding community. “You can do as much as you can to try and keep the virus out of nursing homes, but the more transmission there is in the community, the more chances there are for the virus to sneak in,” Justin Lessler, an associate professor of epidemiology at the Johns Hopkins Bloomberg School of Public Health, told AARP earlier in the pandemic.
Cases in the broader U.S. population have skyrocketed in recent weeks, due mostly to the highly transmissible omicron variant. The country is averaging more than 700,000 new infections per day, almost triple the average daily peak of last winter. But deaths have increased only slightly, suggesting that omicron may cause less severe illness than other forms of the virus.
Doctors are saying that the vast majority of hospitalized omicron patients in ICUs are either unvaccinated or have severely compromised immune systems. While 87 percent of nursing home residents are vaccinated, most are immunocompromised, with chronic medical conditions.
Nursing homes remained relatively unscathed during the first few weeks of omicron’s spread. But recent data from the Centers for Disease Control and Prevention (CDC) show that’s changing fast, with weekly cases among residents increasing more than seven-fold between the weeks ending Dec. 19 and Jan. 9 — from 4,300 to 32,000 nationally. The latest weekly infection rate is just shy of the worst infection rate on record, reported last winter.
Infections among nursing home staff are even worse, increasing almost ten-fold — from 6,000 cases to 57,000 nationally — during the same period. The latest weekly staff infection rate is roughly double the worst rate recorded last winter, and the latest weekly number of staff deaths, 67, is the second-highest recorded in the pandemic. That may foretell what’s in store for residents, says Harvard health policy professor David Grabowski, a leading researcher on COVID-19 in nursing homes.
“Staff COVID cases are the canary in the coal mine,” he recently tweeted, adding last week that nursing home cases are going to continue to “increase dramatically in coming weeks.”
For now, resident deaths are up only slightly, according to the CDC data. Whether that changes “hinges on how well full [vaccination] and boosters protect nursing home residents from omicron,” Grabowski writes. “Getting boosters for as many nursing home residents needs to be a national priority.”
Lagging booster rates
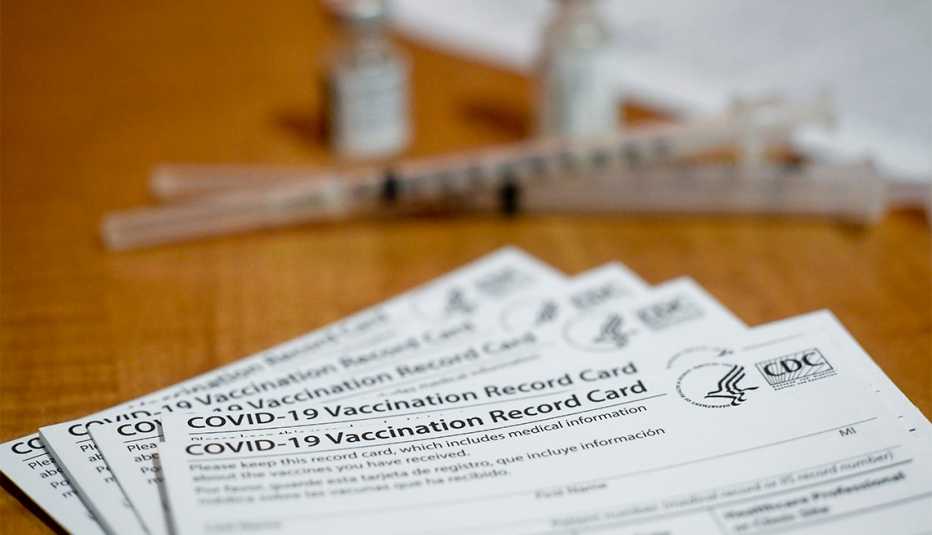
When COVID-19 vaccines became available in the U.S. in December 2020, nursing home residents were some of the first to receive the jabs. A federal vaccination campaign, which sent squads from CVS and Walgreens into most of the nation’s nursing homes, had most residents fully vaccinated by the end of March.
But studies last summer showed that vaccination becomes less effective over time, especially in people 65 and older. The CDC soon began recommending boosters for nursing home residents. This time, however, there would be no federal campaign to administer the boosters, leaving states or facilities responsible.