AARP Hearing Center
What Happens to Nursing Home Workers Who Missed COVID-19 Vaccinations?
More long-term staff members want a shot, but access is suddenly more limited

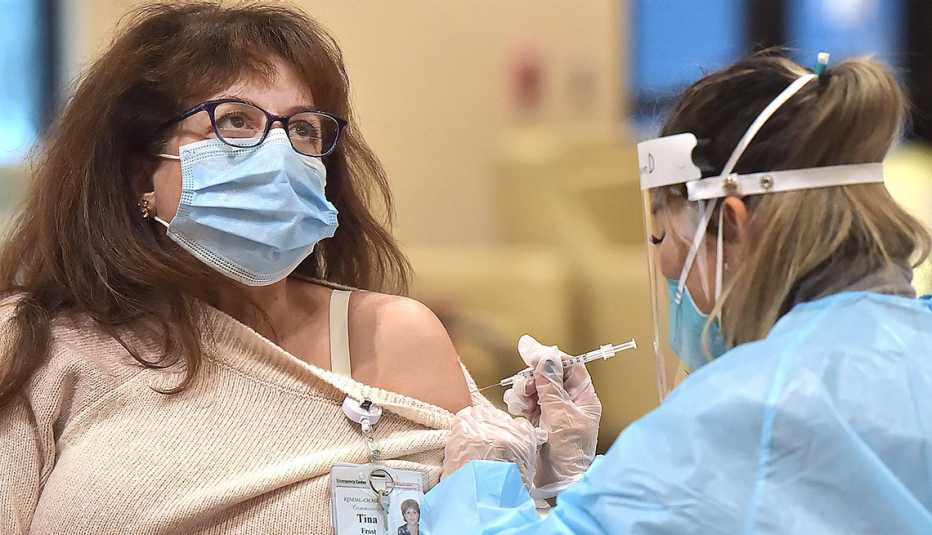
COVID-19 has rampaged through nursing homes and other long-term-care facilities, leaving a death toll near 180,000 and counting. So when the first coronavirus vaccines became available at the end of last year, nursing home residents and staff were first in line, given top priority along with emergency responders and health care providers.
The federal government contracted with CVS and Walgreens to administer three vaccination clinics for residents and staff at nearly every nursing home in the U.S. That effort, called the Pharmacy Partnership for Long-Term Care Program, wraps up this month.
So how do new nursing home residents and workers who missed the onsite clinics get vaccinated now? For residents, plans are in the works to make sure they get the shots. But so far, many of those plans don't include the staff members who care for them.
Responsibility for vaccinations now falls to individual facilities, said Katherine Grusich, a spokeswoman for the U.S. Centers for Disease Control and Prevention (CDC). The federal government is giving COVID-19 vaccines to local health departments and to the specialized long-term care pharmacies that provide facilities with other medications, although the CDC doesn't require nursing homes to give residents the vaccines. Even the federal Centers for Medicare & Medicaid Services (CMS), which regulates nursing homes, “does not currently require nursing homes to offer COVID-19 vaccines to residents and staff,” a CMS spokesperson said.
Nevertheless, most residents have been fully vaccinated and cases of the virus and resulting deaths have dropped dramatically in recent months. Uptake among nursing home staff members, meanwhile, has been much lower: In facilities covered in a study last month in the Journal of the American Medical Association, 78 percent of residents were vaccinated, compared to only 38 percent of employees.
That's a problem, since people going in and out of nursing homes can bring the virus with them, even if they don't have symptoms. Workers can become vectors of virus spread. The good news is that vaccine hesitancy among workers looks to be fading. “We saw a lot of staff decline the vaccine at the first visit but then choose to do it at the latter clinics,” said David Grabowski, a professor of health care policy at Harvard Medical School, describing the three federally backed clinics at facilities.
But once nursing homes have had their three clinics, he said, “there's no [federal] plan to circle back."
‘A lot of us were scared at first'

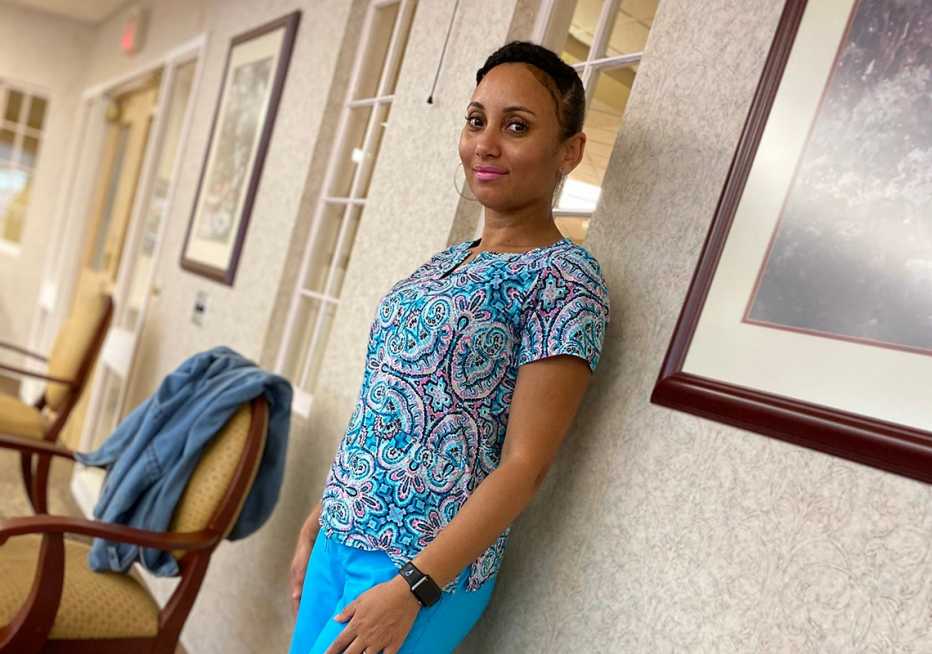
Many nursing home employees, who are generally poorly paid and often work without benefits like sick leave, were initially skeptical of COVID-19 vaccines. “A lot of us were scared at first because we didn't get enough information,” said Adelina Ramos, a certified nursing assistant at a Rhode Island nursing home. She spoke to AARP after testifying before the Senate Finance Committee last week about how nursing homes have responded to the pandemic.


Eventually, the administration at Ramos’ nursing home suggested that employees with questions about the vaccine call a phone number to reach one of the facility's doctors. Administrators also met with union representatives to discuss vaccinations.
"But as health care workers, we don't have a lot of time and we rarely get a break,” Ramos said. “Most of us work double eight-hour shifts or multiple jobs to get by.” Some still don't trust their employers or the new presidential administration in Washington, she said.
Ramos said many of her coworkers “didn't want to be the guinea pigs, so they were waiting to see who goes first and see how their reactions were.” She did her own research before she was convinced the vaccine was safe and is now working as a union delegate with the Service Employees International Union District 1199 New England, to educate coworkers about her experience and encourage them to get it.
The American Health Care Association and National Center for Assisted Living, which represents more than 14,000 nursing homes and long-term care facilities, and LeadingAge, representing more than 5,000 nonprofit nursing homes and other providers, have set a goal of vaccinating 75 percent of the nation's roughly 1.5 million nursing home staff members by June 30.
Patchwork of state systems
Nursing home employees still have priority status for vaccine appointments, as recommended by the CDC. But it may not mean much. States are allowed to put them into the pool with every other person who's eligible for a vaccine appointment. Connecticut is among a handful of states taking that approach.
Other states have different plans and rules.
New Jersey, for example, is working on a plan to deliver vaccines to residents and staff in nursing homes. Until it gets off the ground, they “can access vaccines on their own anywhere where appointments in the state are available,” the state's health commissioner, Judith Persichilli, said this week. But getting access hasn't been easy.
"Many nursing home workers in New Jersey are still in need of vaccination, and some have expressed frustration in being unable to find appointments through their counties’ online portals or private vaccination sites,” says Milly Silva, executive vice president of 1199 SEIU United Healthcare Workers East, a union representing about 8,000 nursing home employees at 80 facilities in New Jersey. “Part of this is likely due to technology and language barriers among this diverse and low-wage workforce."
Since the federal vaccine clinics ended, Rhode Island officials hired two ambulance companies whose emergency medical technicians will administer vaccines to residents in their nursing homes, said Kathleen Heren, the Rhode Island long-term care ombudsman, who advocates for long-term care consumers. But the plan doesn't include employees.
Next door, in Massachusetts, nursing homes are also vaccinating new residents but not employees. SEIU's United Healthcare Workers East, which represents nearly 3,000 nursing home workers in the state, is in conversations with the state health department and facility owners “about how to ensure that new employees are able to possibly get vaccinated at the same time,” said Marlishia Aho, an SEIU regional communications manager.
Megan O'Reilly, AARP's vice president for government affairs, federal health and family, said nursing facilities and states need to protect residents and staff against the virus: “We would urge that facilities and states work together to make sure that residents and staff continue to have access to the vaccine."
Ohio appears to be one of the few states doing that, launching a COVID-19 vaccine maintenance program for staff members and residents who want the vaccine after the end of the federal vaccination effort. Employees and residents who declined the vaccine earlier will be able to get it at their facility, along with any new arrivals. Residents get first priority.
"We need to continue making the vaccine available to residents and employees at our nursing homes and assisted living facilities,” Ohio Gov. Mike DeWine said this month, “because we must continue to protect our most vulnerable population of older Ohioans against COVID-19.”

































































More From AARP
Nursing Home Staff Shortages and Vaccines
But an AARP analysis of federal data shows that staff vaccinations are up significantly