Staying Fit
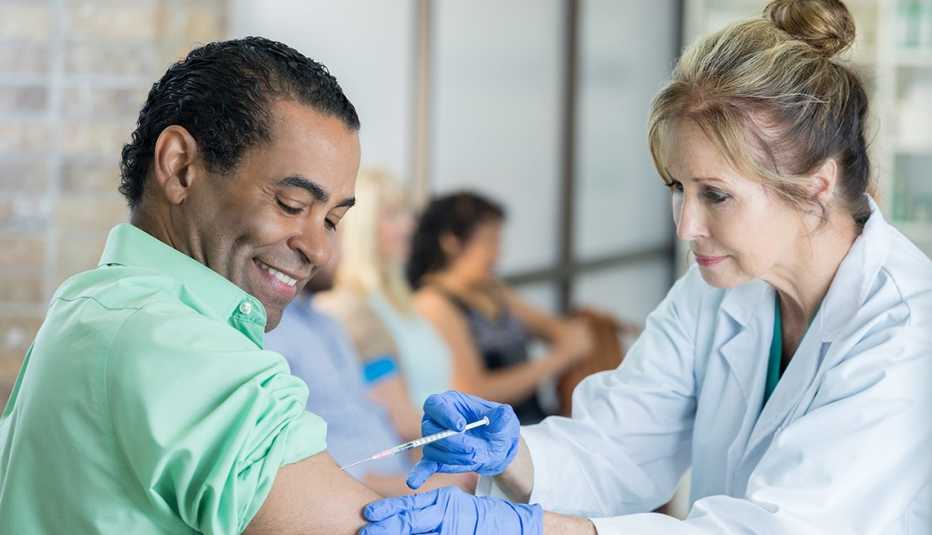
The race to develop a coronavirus vaccine is moving at record speed, and experts predict the finish line is near. Phase 3 clinical trials testing the safety and effectiveness of four vaccine candidates are underway in the U.S., and the federal government is putting plans into place for how the data will be reviewed and how the medicine will be distributed.
But with everything happening so quickly, Americans have questions: Will the shots be safe? How effective will a vaccine be at preventing COVID-19 or lessening the severity of the illness, which so far has killed more than 1.1 million people worldwide?


AARP Membership— $12 for your first year when you sign up for Automatic Renewal
Get instant access to members-only products and hundreds of discounts, a free second membership, and a subscription to AARP the Magazine.
Food and Drug Administration (FDA) Commissioner Stephen Hahn recently spoke with AARP to answer these questions. His responses have been edited for length and clarity.
To date, the fastest vaccine created took four years. We're not even one year into the coronavirus pandemic, and already we have multiple vaccine candidates in late-stage clinical trials. How were we able to fast-track this vaccine? What steps were skipped over or accelerated, and is patient safety being protected in the process?
This is a public health emergency like we haven't seen in many, many years, and so the urgency around this is to find a vaccine that is safe and effective as quickly as possible — that's the goal. There are a number of things that can and have been done to accelerate that process, but I want to emphasize, up front, that no corners are being cut.
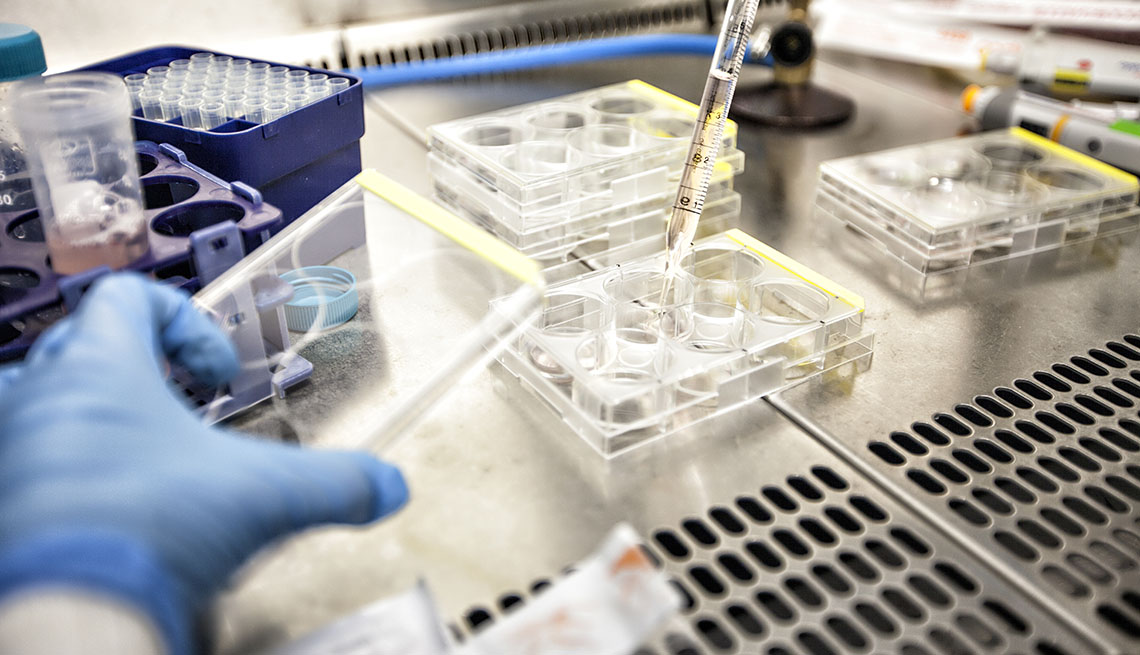
We can start with the clinical-trials aspect of the development: The genetic sequence of the new virus was first identified in January, and soon after, attempts were made to develop a vaccine. That happened very quickly; it doesn't typically happen that quickly. Then, there was a coordination of the preclinical studies so that the different types of vaccines could be studied in animals, and the whole effort quickly moved on to the clinical trials.
Now, what we did at the FDA was we used what's called a rolling review: Typically, we would look at the animal data and then say whether it's okay to proceed to a phase 1 trial. We did that, but we did that in real time with each of the manufacturers. Then, we worked with the manufacturers so they could design what's called a “seamless” clinical trial design, so that when they reached a certain parameter — say, safety in phase 1 — they were permitted to move very quickly to phase 2, which is to look for an immunologic response to the vaccine. The same thing occurred to move to phase 3. You can cut weeks, months, significant amounts of time, using the seamless clinical trial design.
Phase 1: The first phase of the clinical trial process tests the safety of a drug or treatment in a small group of people for the first time. Researchers also determine a safe dosage range and identify side effects.
Phase 2: The next phase tests the drug or treatment in a larger population to see if it is effective. This phase also evaluates safety.
Phase 3: In this phase, a drug or treatment is given to large groups of people. The point is to confirm its effectiveness, monitor side effects, study different populations and different dosages, and collect information that will allow the experimental drug or treatment to be used safely.
Phase 4: This phase takes place after a treatment is approved for use by the FDA. It provides additional information including the treatment or drug's risks, benefits and best use.
Source: FDA
And then, finally, we've been working with the manufacturers around the quality of their manufacturing, the consistency of it. So that if a vaccine were to be authorized or approved, we could immediately know that quality manufacturing is in place. And again, that process normally takes months.