AARP Hearing Center


Roughly 104,960 Americans will be diagnosed with melanoma this year, according to the American Cancer Society, making it one of the most common types of cancer in the U.S., especially among older adults who have endured decades of sun exposure and whose immune systems aren’t as robust as they once were. In women ages 50 and older, rates of new cases continue to increase by almost 3 percent each year.
The good news: Melanoma is highly curable if it’s caught early. Do you know what to look for?
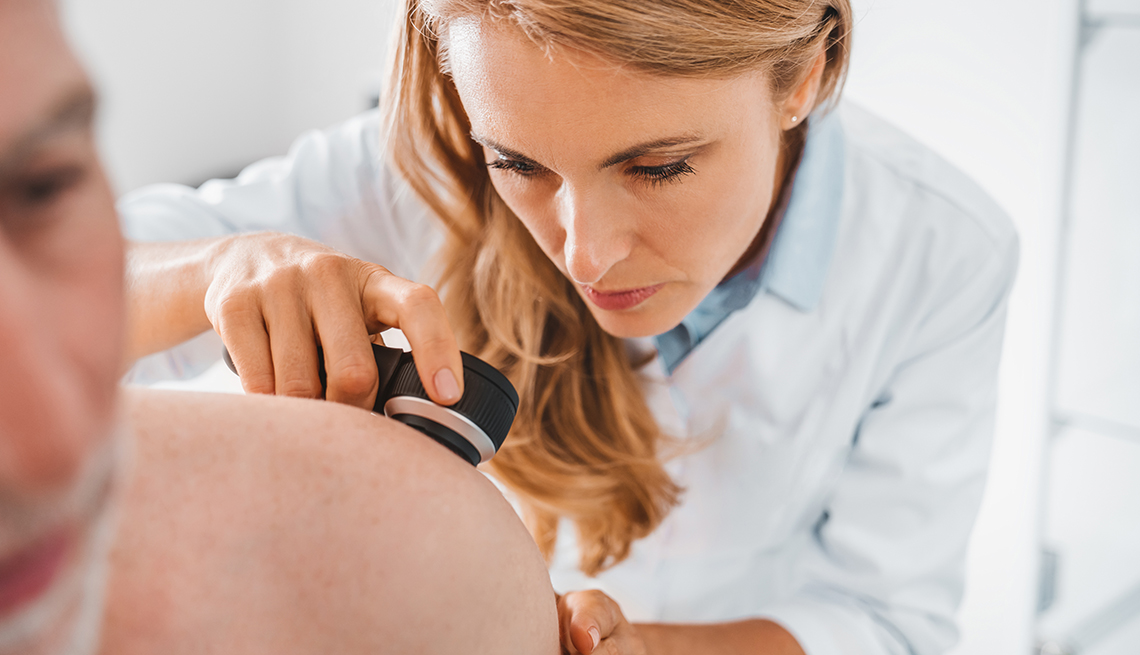
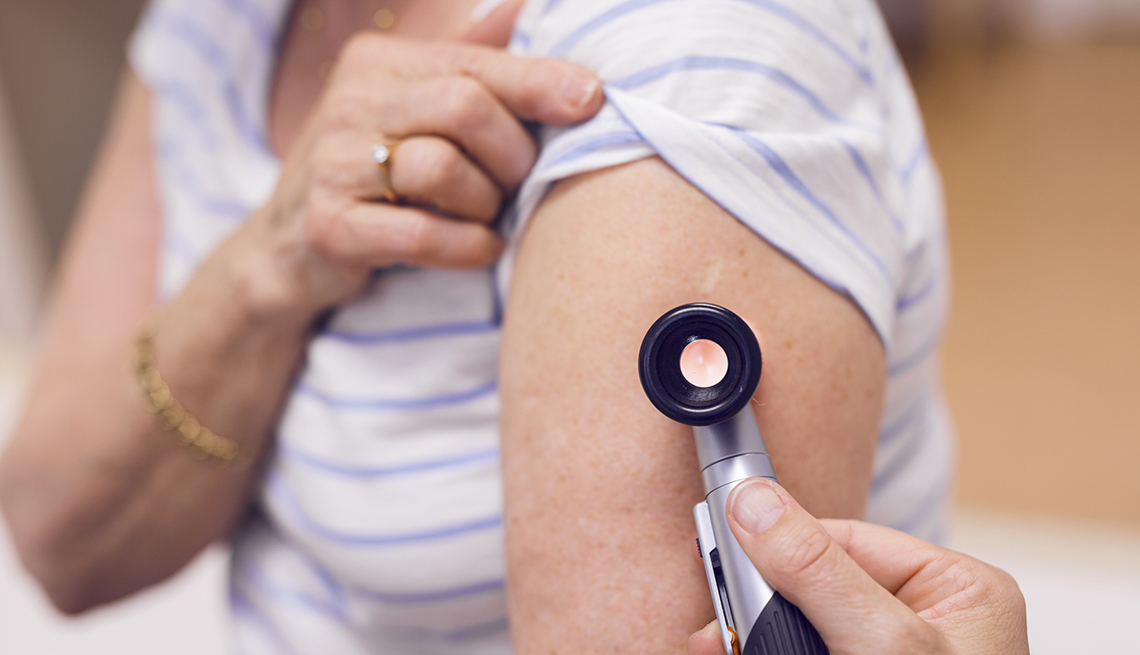
The hallmarks of melanoma are asymmetrical or rough-looking moles without clearly defined borders. A spot on the skin that continues to grow in size or change is another indication, and a once-monthly body scan is an easy way to keep tabs on any of these concerning characteristics.
But there are also some more unusual signs that could signal the presence of the skin cancer.
“Melanoma is such a rule breaker,” says Elizabeth Buchbinder, M.D., an oncologist at the Dana-Farber Cancer Institute in Boston and an assistant professor at Harvard Medical School. Little moles can cause big trouble, and new spots can grow and spread quickly, she adds. “And so knowing what to look out for is super important.”
Here are four warning signs of melanoma you need to know about so that no spot goes unnoticed.
1. The ‘ugly duckling’
People who have lots of moles are at increased risk for melanoma. That doesn’t mean, however, that you need to panic over every mark on your body. Pay attention to the moles that stand out — those that are darker than the rest, have changed recently or are more oddly shaped. Buchbinder calls these “ugly ducklings.”
“If you have a bunch of dark moles, but you have 50 of them, they’re not all melanomas,” she says. “But if you have one mole that really looks different than the others, and it’s kind of that ugly duckling, that’s the one that you really want to get looked at and checked.”
With women, melanomas most commonly appear on the arms and legs. Men need to pay special attention to their head, neck, back and trunk. Still, those aren’t the only places this type of skin cancer can pop up.


















































































More From AARP
Can You Safely Get Vitamin D From the Sun?
A few minutes in the sun might have benefits, but risks include skin cancer, wrinkles
AARP Smart Guide to Sun Protection
SPF is just one important factor — here are more tools that can help in preventing damage from harmful rays
7 Skin Conditions That Need Medical Attention
They may not signal skin cancer, but they could still spell trouble