AARP Hearing Center


Fall is synonymous with the start of flu season, and experts are beginning to prepare for what could be another bad year.
Tracking influenza activity in the Southern Hemisphere usually “allows some degree of predictability” for what we can expect in the U.S., explains Gregory Poland, M.D., professor of medicine and director of the Vaccine Research Group at Mayo Clinic. And Australia — though not as bad as last year — is coming off a bit of a rough flu season, with an earlier-than-usual spike in illness, according to the country’s July surveillance report.
That doesn’t necessarily mean we will see the same, Poland says. There’s a lot of variability with the virus, and global health officials say it’s still too soon to predict the severity of the season in the Northern Hemisphere. “But even a normal flu year is still something to worry about,” says Michael A. Ben-Aderet, M.D., an infectious disease physician at Cedars Sinai, pointing to the tens of thousands of deaths and hundreds of thousands of hospitalizations that occur in the U.S. each year.
It’s estimated that the U.S. saw as many as 650,000 hospitalizations and as many as 58,000 deaths due to flu during the 2022-2023 season.
And with a swell of COVID-19 cases and hospitalizations, experts are taking the opportunity to remind people of some measures that can minimize illness and lower the likelihood that we experience another “tripledemic,” since “we’ll probably see, at some point, all three viruses circulating at the same time,” Ben-Aderet says, referring to influenza, COVID-19 and RSV (respiratory syncytial virus).
Flu shot can help blunt the burden
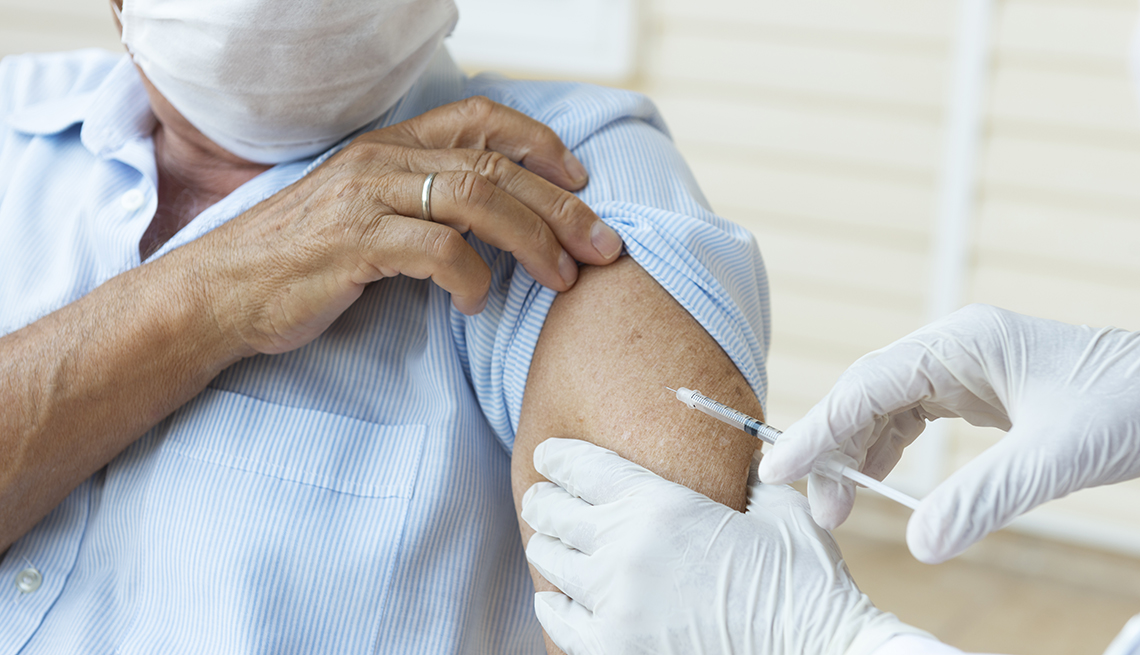
One way to avoid a bad flu year is to get the flu shot, which lowers your risk of getting infected or severely sick from an influenza infection. The problem, Poland says, is that “we’re seeing a general but measurable decline in people’s acceptance of vaccines overall.” And that trend could affect flu activity and severity this fall and winter.
Flu vaccination is especially important for older adults, who are at higher risk of complications from the virus. (It’s estimated that 70 to 85 percent of flu-related deaths and 50 to 70 percent of flu-related hospitalizations occur in people 65 and older.) In fact, older adults need what’s known as a high-dose flu shot, which packs extra protection.































































)
)













More From AARP
3 Shots This Fall: What to Know About COVID, RSV and Flu Vaccines
Advice on when — and how often — to get themFlu Hospitalization Risk Higher for Minorities
Health experts urge all adults to get the flu shot this yearSuperfoods for Flu Season
What to eat or drink to build a stronger defense this winter