Staying Fit

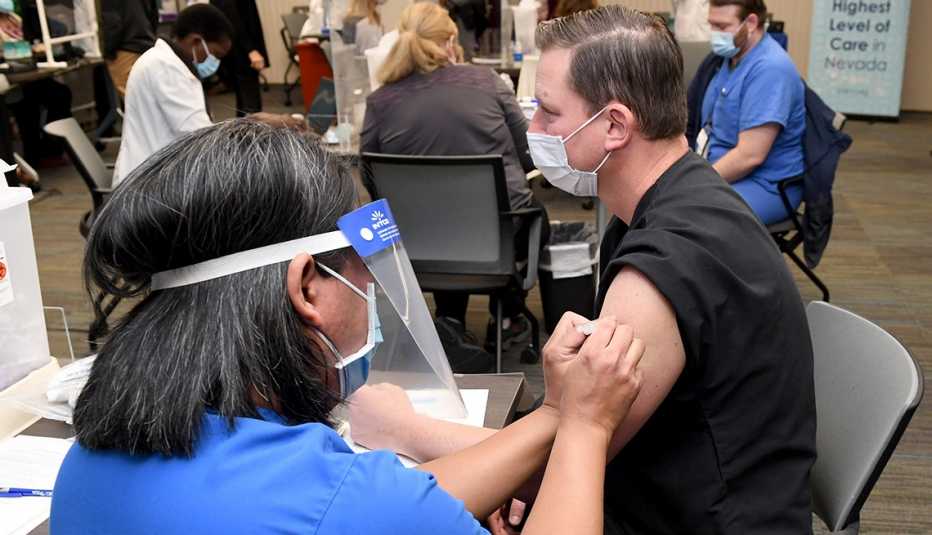
People age 75 and older and frontline essential workers, including police officers, firefighters, teachers, grocery store staff and U.S. Postal Service employees, should be next in line to get a COVID-19 vaccine, a federal advisory panel recommended on Dec. 20.
By a 13-1 vote, the Advisory Committee on Immunization Practices (ACIP) also recommended to the Centers for Disease Control and Prevention (CDC) that people ages 65 to 74, people ages 16 to 64 with high-risk conditions and other essential workers follow in what's being called Phase 1c, behind Americans 75-plus and frontline essential employees in Phase 1b. Whether or not to include all people 65 and older in Phase 1b consumed much of the debate during ACIP's five-hour meeting.


AARP Membership— $12 for your first year when you sign up for Automatic Renewal
Get instant access to members-only products and hundreds of discounts, a free second membership, and a subscription to AARP the Magazine.
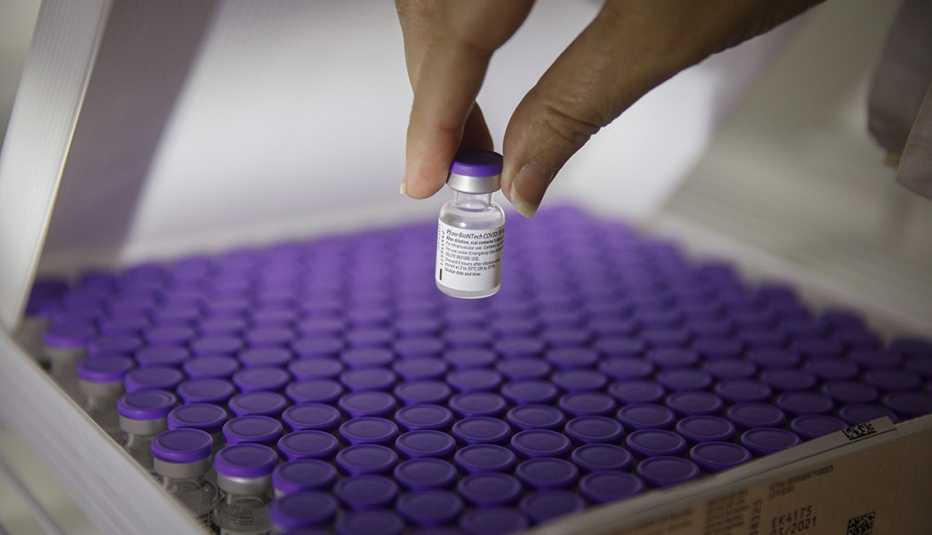
The first priority group of 24 million Americans, designated as Phase 1a, began getting inoculated last week with the Pfizer-BioNTech vaccine. This category includes health care workers and residents and staff of nursing homes. Nearly 6 million doses of the Moderna vaccine, which received its emergency use authorization (EUA) from the U.S. Food and Drug Administration (FDA) on Dec. 18, have already begun to ship.
Vaccine Priority Groups
Phase 1a (24 million people):
- Health care personnel
- Long-term care facility residents
Phase 1b (49 million people):
- Frontline essential workers
- People 75 and older
Phase 1c (129 million people):
- People ages 65-74
- People ages 16-64 with high-risk conditions
- Other essential workers
Phase 2:
- People 16 and older not in Phase 1
Source: CDC

Under the ACIP recommendation, the second priority group, dubbed 1b, would include 19 million elderly people 75-plus and 30 million essential frontline workers. They would begin to get their shots after those in group 1a who wanted to be vaccinated were taken care of. Then after group 1b has been vaccinated, 129 million people in group 1c would come next. ACIP says that group should include 28 million Americans ages 65 to 74, 20 million other essential workers and 81 million people ages 16 to 64 who have high risk factors for the coronavirus.
"I voted no,” said ACIP member Henry Bernstein, a physician at Northwell Children's Medical Center on Long Island, New York, “because I feel that the science regarding COVID-19 morbidity and mortality” is similar among those between 65 years old and 74 years old and those over 75. Several other committee members questioned splitting the two older age groups. Pablo Sanchez, a doctor at the Research Institute at Nationwide Children's Hospital in Columbus, Ohio, said that although he voted yes, he also really felt “strongly that the elderly and those with high-risk medical conditions should be up front, over some essential workers who may be younger."
"We're are trying to thread the needle here,” said Peter Szilagyi, a doctor at UCLA. And Beth Bell, a physician at the University of Washington in Seattle, said she wished “we didn't have to be here making allocation recommendations. And that instead we had enough vaccine to provide it to everybody in the country who wants it."

































































More on Health
What the End of the COVID Emergencies Means
It will affect how many people access and pay for tests and treatments
What to Know About the Coronavirus Vaccines
Questions continue as millions of Americans get immunized
What You Need to Know About the Coronavirus
The latest news on COVID-19 and answers to frequently asked questions