Staying Fit


This very morning, in tens of millions of houses and apartments across the land, a spouse, child or friend will offer a steady hand to an older or infirm loved one, getting her dressed and fed, organizing pills, taking medical readings, setting him up for the day ahead. Later on, these caregivers might pay their loved one’s bills, deal with insurance claims, even do their shopping. Only when all that is handled can they live their own lives.
To reveal the full span of their devotion, challenge and frustration, AARP interviewed dozens of caregivers. Here’s a glimpse of life from their perspective.


AARP Membership— $12 for your first year when you sign up for Automatic Renewal
Get instant access to members-only products and hundreds of discounts, a free second membership, and a subscription to AARP the Magazine.
First signs
Bryan Kramer (52; he has been caring full-time for his now 54-year-old wife at home in Hemet, California, since May 2016): It was Friday the 13th and I got a call at work from my sister-in-law saying she couldn’t get into our house. I knew my wife was home so I rushed over. The door would only open about 2 inches because my wife was on the floor. Norma was alive, but she’d had a massive stroke — at the age of 48.
Janet Lenius (57; she has gradually taken on more caregiving responsibilities at home in Minneapolis as her 90-year-old mom’s health has declined): It wasn’t one thing; it was lots of things. Pneumonia, a heart condition, hospitalizations, mild cognitive impairment that kept getting worse. My mother’s car got stuck in a puddle one day and she opened the door and it flooded. That’s when she stopped driving completely. Her circle kept getting smaller. I had to step in.
Laura Crews (64; a hired aide helps by day, but she takes over caregiving after work for her husband, 67, who has frontotemporal dementia, at their home in the Seattle area): For a while after the diagnosis, Don didn’t need care every minute. But then I’d come home and find bizarre things. He broke a plate and tried to glue it with Gorilla Glue and got glue everywhere. Another day he took it upon himself to repair the deck by drilling in random screws. I was horrified. Don was a Boeing engineer but now he didn’t have any idea what he was doing. Somebody had to watch him.
Amy Goyer (61; AARP’s national family and caregiving expert, has been a caregiver since age 20 for various family members): I’m the youngest of four girls, I wasn’t married, I didn’t have children, I worked in health care. It was only natural that when an older relative needed help putting up a Christmas tree or fixing an old Victrola, I’d say, “I’ll just go check on things.”
Carol McCarrick (64; she has worked full-time while also caring for her husband, 70, at home in Kerrville, Texas, since 2013): Steve worked full-time, and on the side rode horses, took 150-mile bike rides, taught classes. One day he came in and just dropped from an aneurysm. We live in rural Texas. He had to be airlifted. If I wasn’t there, he would have died.

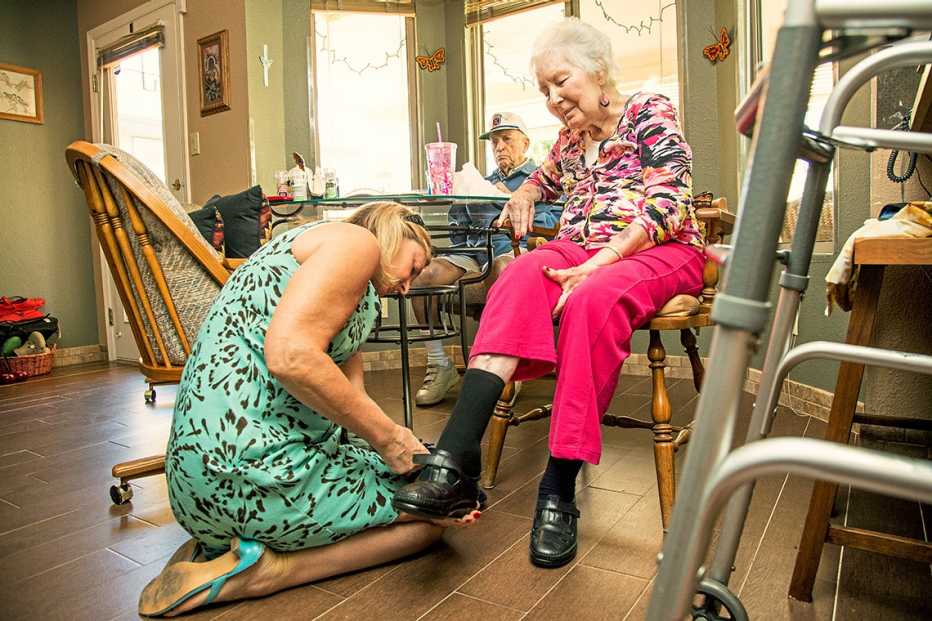
Karen Mason (62; she cares for her disabled adult daughter at home in Forrest City, Arkansas): Tasha, my daughter, was born with cerebral palsy. Taking care of her wasn’t a choice. It’s been my reality every day for 37 years.
Jeanie Olinger (61; she has overseen care full-time for her 37-year-old son in Longview, Texas, since his 2008 car accident. She also cared for her aunt at home and in a nursing home until her aunt’s death last September): I remember going for a walk as they bathed Chris at the hospital. He was 24 and had suffered brain injuries they said would be permanent. I realized this was going to be a long journey but I committed to it. In that instant, I let go of whatever I thought the future looked like. I came back and sat at his bedside and just said, “Bubba, I cannot walk this for you, but I can walk it with you.”
The confusion of care options
Laura Crews: I didn’t know what to do, honestly. I just started searching online for “caregiver.” You see all these choices: adult day care, in-home care, nursing facilities, assisted living, continuing care. You call places and everybody says, “Yes, yes, we can help.” But I never really felt good about these conversations. Everything felt like a sales pitch. Then my neighbor said, “Hey, I know this older lady who might help.” She’s been with us ever since.
Karen Mason: You piece it together. Family, hired help, respite care. No way was I putting my daughter in a nursing home. When I was younger, I worked as a visiting nurse in some of the finest facilities money can buy. Chandeliers, baby grand pianos. But the care was deplorable. I had a patient dying of cancer. Queen Anne bedroom set and all that. But they didn’t change her sheets. She couldn’t feed herself but they’d leave food and walk away.


Zander Keig (55; he is a Latino trans man and Coast Guard veteran caring for his Marine Corps veteran father, who’s 81, in Orlando, Florida): I got Dad enrolled in the geriatric clinic at the local VA but the wait was seven months to get him into adult day care. He moved in with my wife and me but at a certain point, we noticed things — like Dad no longer understood how to operate the microwave and couldn’t be left alone all day. We found an inpatient facility nearby with six bedrooms. That looked great but it was $3,000 a month and dad was only getting $1,740 a month from Social Security. We simply couldn’t afford it. We ended up having to put him in a much larger independent-plus program at an assisted living facility with hundreds of people about 2½ hours away.
Rachel Hiles (35; she lives in Kansas City, Missouri, and cared for her grandmother until she died in January at age 85): We never had a conversation before any of this. I wish we had. My single mom passed away. I’m an only child and my grandma’s an only child so my grandma’s care fell to me. Right before COVID, she got pneumonia and went into the hospital. There was this defining moment when I had two choices: Take her home or send her to rehab. Neither was perfect. But I knew if she went to rehab, she’d probably end up staying there.
Steve Cogburn (69; he cared for his wife, who had heart disease and dementia, for eight years at home and in hospitals around Holyoke, Colorado, until her death in 2020): In our rural area there was no home health care. Zero. The closest was about 50 miles away. They would send an aide out twice a week for one hour a day to either bathe her or to wash clothes or clean the bathroom and that served no useful purpose to me whatsoever. It was all on me.
Carol McCarrick: You wouldn't believe how many people asked me in the beginning if I was going to stay with Steve, and I was, like, well, why wouldn’t I? Even his neurologist told me I should put him in a home. I just wasn’t going to do that. You think you know about love but you really don’t until you have to take care of somebody.
The financial maneuvering
Laura Crews: Right now we’re OK, but who knows? Don has a pension from Boeing, he’s getting Social Security, I’m still working. But most of my salary and then some goes to the lady who watches him during the day. I’ve had to buy a hospital bed, a lift chair. I pay an extraordinary amount for an expensive medication he needs. I wish we would have gotten long-term care insurance. My biggest worry is that if I can’t take care of Don and have to put him in a nursing home, that would whittle down our savings really fast.
Carol McCarrick: That little helicopter ride was $25,000. While Steve was in the ICU, I had to have the house completely redone. Doors enlarged, bathrooms overhauled, carpets up. It took all our savings, about $80,000, before he could even come home. Steve was eight months from full retirement at his state job and I begged them for full benefits, for his pension and all that, but they wouldn’t go for it. So, now, instead of thinking about retirement in a year, I’m working 10 hours a day as a social worker so I can pay for caretakers.



































































More From AARP
Medicare, Medicaid and Long-Term Care
What the programs cover, and what they don’tThe Unique Challenges of Dementia Caregiving
Tips on how to manage such often-difficult careReal Problems, Real Solutions to the Long-Term Care Crisis
Making at-home care work for America starts with tackling these 6 challenges