AARP Hearing Center


Shingles is sneaky. It’s caused by the same virus as chickenpox, varicella-zoster, which lies dormant for decades in the body, ready to pounce.
“Our body gets it under control, but it never fully goes away and lives in our nerves,” says Dr. Ian Neel, an associate professor of medicine and clinical lead of the Geriatric Medicine Consult Services at Senior Behavioral Health at UC San Diego Health. “But as we age, our immune system wanes, and it puts us at higher risk of this virus breaking out of its cage and reactivating.”
In the U.S., 1 in 3 people will get shingles, usually after age 50, with the risk of complications climbing sharply after age 60. Since the risk rises with age, half of those who live to 85 will experience at least one episode.
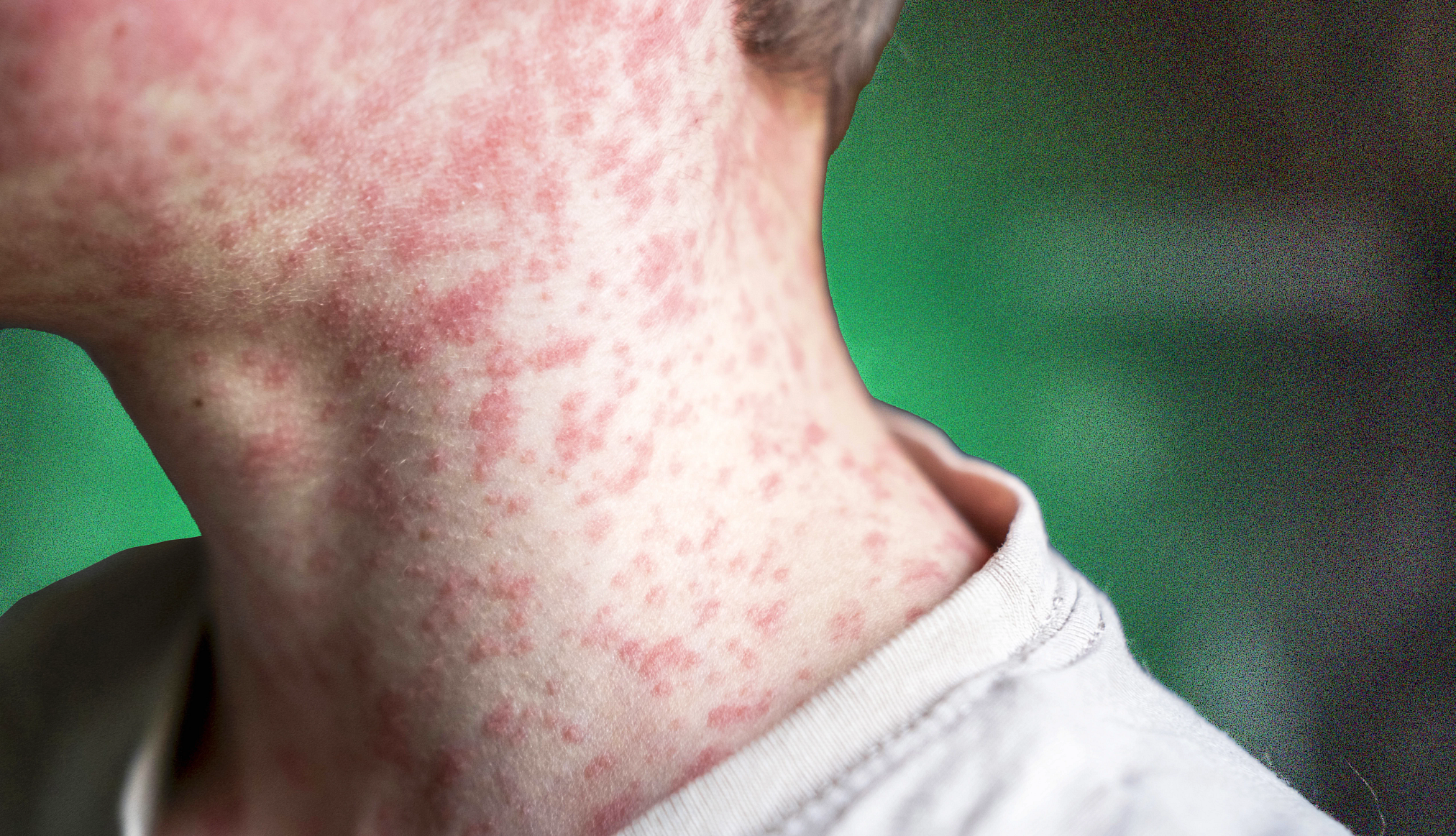
Shingles’ most common symptom is an angry, blistering rash. And about 10 to 18 percent of people who develop that rash will also experience a complication known as postherpetic neuralgia, a condition that affects the nerve fibers and skin, causing burning—and sometimes incapacitating — pain that can last for months (or even years) after the rash disappears.
“Shingles rarely kills you,” says Dr. William Schaffner, a professor of preventive medicine and infectious diseases at the Vanderbilt University Medical Center in Nashville, Tennessee. “But it can make you wish you were dead.”
Enter Shingrix, a vaccine approved by the U.S. Food and Drug Administration in 2017. Unlike Zostavax, its predecessor, Shingrix is “spectacularly effective,” Schaffner says.
The numbers support his claim. The two-dose course of Shingrix is 97 percent successful at preventing shingles in people in their 50s and 60s, and 91 percent successful for those in their 70s and older. (That protection stays at over 85 percent in people 70-plus for four years after they get the vaccination.)
What’s more, studies suggest the vaccine may also lower the risk of shingles-related strokes in older adults. Plus, it may have additional health benefits. (Read more below.)





































































))
))






)
)






More on Health
Should You Be Worried About Measles?
New cases are being reported. Here's what you need to know.
Can Getting Vaccinated Lower Dementia Risk?
There’s growing evidence that getting your shots can lower dementia risk
Smart Guide to Vaccines for Adults Over 50
A comprehensive guide to vaccines and their benefits
Recommended for You