AARP Hearing Center

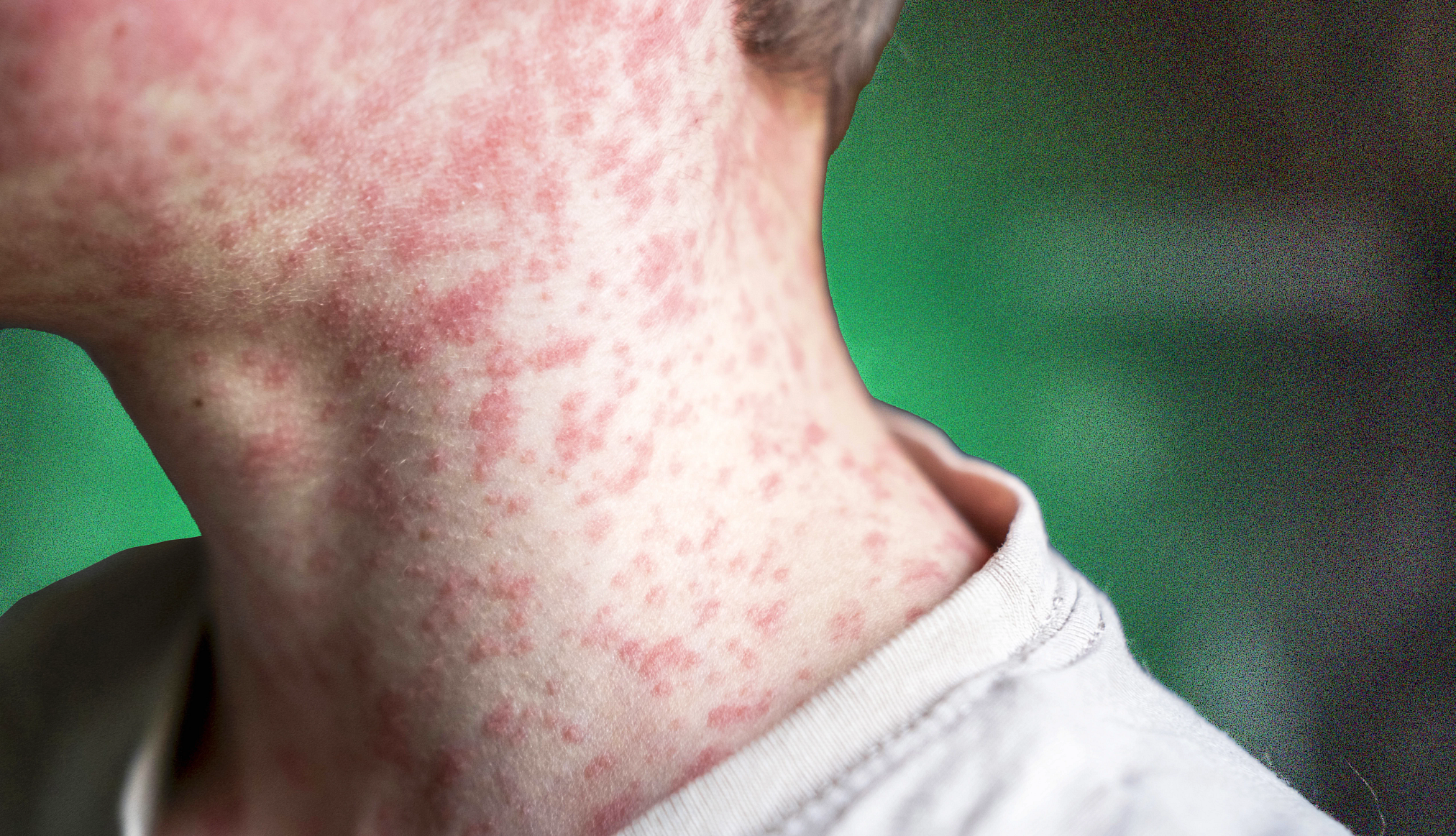
After reaching 2,276 confirmed cases in 2025, measles continues to spread in the United States. More than 730 cases have been reported so far this year, most stemming from a large outbreak in South Carolina. Public health experts say if sustained rates of transmission continue, the U.S. could lose its elimination status, which it has held since 2000.
The vast majority of cases reported this year and last — which had the highest number of cases on record in more than three decades — have occurred in unvaccinated individuals or people of unknown vaccine status, according to the Centers for Disease Control and Prevention (CDC).
Here are five things you need to know about the current situation, including vaccine advice for older adults.
1. Measles is highly contagious
If the current tally of cases doesn’t seem particularly alarming compared to other infections and illnesses, know that “even one case of measles is something that we should all sit up and pay attention to,” says Patricia A. Stinchfield, a nurse practitioner and immediate past-president of the National Foundation for Infectious Diseases. “And the reason for that is, it is the most contagious and easily transmissible virus that we have.”
Like many other viruses, measles spreads through droplets released into the air when an infected person coughs or sneezes.
But unlike other common viruses, measles is so contagious that up to 90 percent of people who are close to an infected person will become infected if they are not immune to the virus, according to the CDC.
“It doesn’t have to be a cough right in your face,” Stinchfield says. Tiny virus particles can survive in the air for two hours, where they “circulate around and bounce over to this person and that person, and before you know it, you’ve exposed a lot of people,” she says.
What’s more, a person infected with measles can spread the virus four days before the most obvious symptom — a telltale rash — appears, and for four days after.
2. Many older adults have immunity — but some may need the vaccine
With the current outbreak, you might be wondering: Do I need the measles vaccine?





































































))
))






)
)






More From AARP
Do You Need the RSV Vaccine This Fall?
The shot could help to keep you out of the hospitalThese Are the 8 Vaccines You Need After 50
Are you up to date on all the recommended vaccines?
Ask Dr. Adam: How Can I Boost My Immune System?
Help strengthen your body’s defenses against illness this winterRecommended for You