AARP Hearing Center

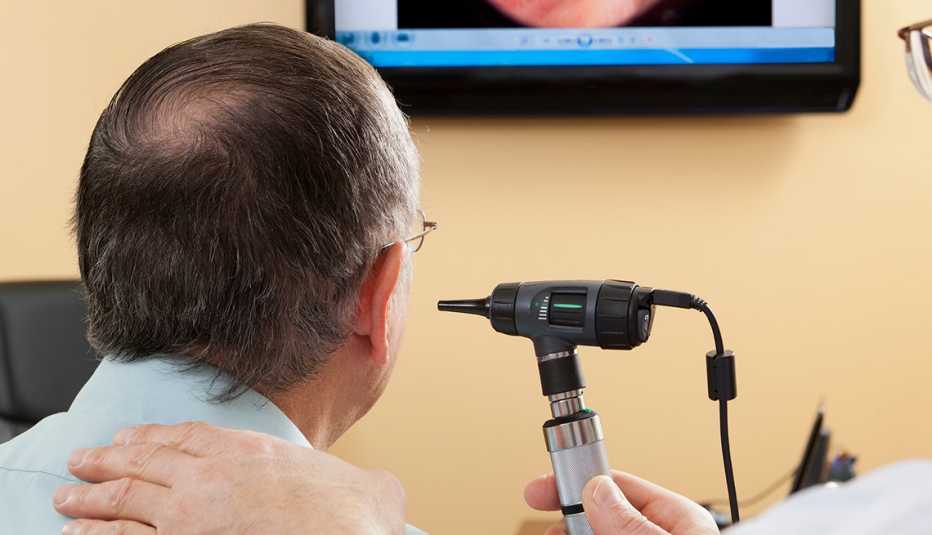
COVID-19 has been linked to a variety of unusual symptoms and long-term complications, and issues related to hearing are not exempt from the list.
It’s common for some changes in hearing to accompany any viral infection of the upper respiratory tract, says Elias Michaelides, M.D., codirector of the Cochlear Implant Program and medical director for outpatient otorhinolaryngology and audiology at Rush University Medical Center in Chicago. That’s because the mucous membranes tend to “get very stuffy” and, as a result, “sometimes fluid can build up behind the eardrums,” he says. This symptom, however, does not cause permanent damage “and often will just clear up on its own” once the infection has passed.
But anecdotal reports and a handful of studies that have emerged since the beginning of the pandemic suggest an association between more persistent hearing problems and COVID-19. For example, researchers from the University of Manchester combed through nearly 60 case reports on the topic and found that about 15 percent of COVID-19 patients experienced tinnitus, or ringing in the ears, after diagnosis, while roughly 8 percent reported hearing loss and 7 percent noted vertigo. The report was published in the International Journal of Audiology in March 2021. An earlier study printed in the same journal found that about 13 percent of patients reported a change in hearing and/ or tinnitus since their COVID diagnosis.
Researchers from the Massachusetts Institute of Technology have also discovered that the virus that causes COVID-19 (SARS-CoV-2) can directly infect cells in the inner ear, which could explain the hearing and balance issues in some COVID-19 patients. And a team from Johns Hopkins School of Medicine found evidence of the virus in the middle ear of COVID-19 patients in an autopsy study, published in 2020 in JAMA Otolaryngology — Head & Neck Surgery.
Despite these findings, experts caution there’s not enough evidence to draw a direct link between a SARS-CoV-2 infection and hearing problems. “But I think it’s an important question to be asking,” says Sarah Sydlowski, audiology director of the Hearing Implant Program at the Cleveland Clinic.
Medications, COVID complications can add to hearing issues
Medical care muddies the waters when it comes to better understanding a possible connection between SARS-CoV-2 and hearing. For starters, a number of factors related to being critically ill can drive hearing loss, especially in older patients, researchers point out. And several drugs currently (and previously) used to treat patients with COVID-19 — including remdesivir, as well as chloroquine and hydroxychloroquine — are ototoxic, meaning they can cause damage to the ear.






































































More on Health
How to Ramp Up Protection in Omicron Wave
CDC Chief offers advice on masks, testing and boosters
How, When and Where Older Adults Can Get COVID-19 Vaccines and Boosters
Boosters are now recommended for many people two or six months after the first round of shotsCheck Out the AARP Hearing Center
Check Out the AARP Hearing Center