Staying Fit
Most people who contract COVID-19, the illness caused by the new coronavirus, are able to heal at home without medical care. But for individuals with more severe cases of the disease, a trip to the hospital may be in order.
What happens when you're there? And what does recovery look like once you leave? Medical experts outline what you can expect if you are hospitalized with a coronavirus infection.


AARP Membership— $12 for your first year when you sign up for Automatic Renewal
Get instant access to members-only products and hundreds of discounts, a free second membership, and a subscription to AARP the Magazine.
Which symptom is sending most people to the hospital?
There isn't a single symptom; doctors are seeing patients with coronavirus infections come in for a number of reasons. Some are going to the hospital with trouble breathing, says geriatrician June McKoy, an associate professor of medicine at the Northwestern University Feinberg School of Medicine. Others are seeking care for weakness caused by gastrointestinal symptoms, including loss of appetite and diarrhea.
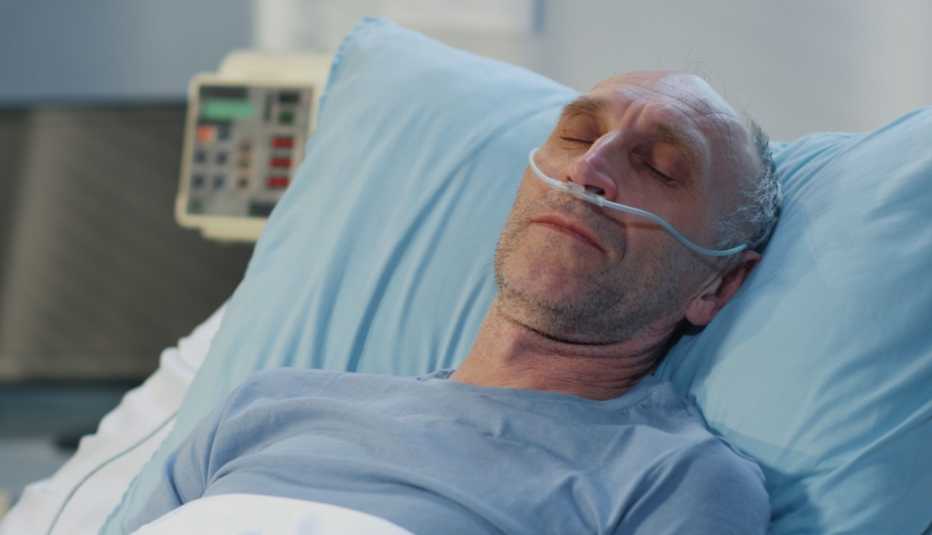
Dizziness, confusion or a sudden change in mental status is another common reason people — especially older adults — head to the hospital. McKoy says one possible explanation for this symptom is that the oxygen levels feeding the brain start to drop, leaving the patient “a little bit befuddled.” In some instances, the onset of dizziness and confusion may cause a person to fall and fracture a bone or two.
"So the presentations are quite atypical,” McKoy says. “The mistake we continue to make is to believe that COVID-19 infection only presents with respiratory symptoms, and that's not true.”
Anyone can get severely ill from a coronavirus infection. However, adults 65 and older and people with chronic health conditions, such as diabetes and heart disease, are at highest risk.
What happens once you are admitted?
Things have changed since the initial surge of the pandemic when most hospitals, especially in the New York City area, “were made up of a lot of ICUs [intensive care units] and patients were coming in in very bad condition,” says Benjamin Salter, an anesthesiologist and assistant professor at Mount Sinai Health System in Manhattan.
Now it's common for hospitals to have “varying levels of COVID-care units,” Salter says, where patients with less critical symptoms receive care — albeit in an isolated area where staff members wear masks and other forms of personal protective equipment. “It's the same as you being admitted to the hospital for a normal, noncritical condition, except that we are going to treat you like you have an airborne disease,” he says.
If your doctor decides that you should be hospitalized for COVID-19 but you are not in need of critical care, you will likely end up in a COVID unit. The type of treatment one receives here depends on the severity of illness.