AARP Hearing Center

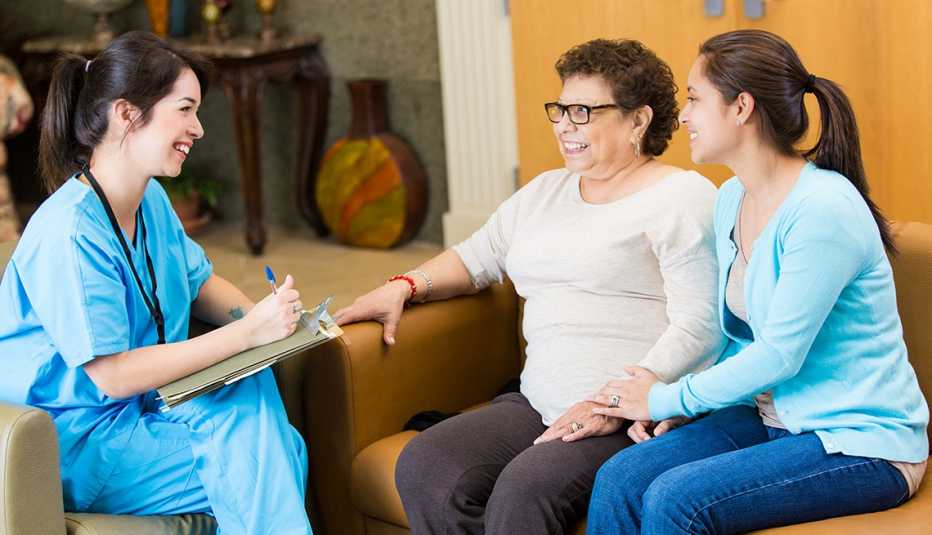
For 20 years, I've studied caregiving. In 2010, I became a family caregiver for my mother and, soon after, a professional caregiver advocate. My life revolves around caregivers, so I read and watch everything I can about the world of caregiving.
At some point, I couldn't help notice how the media portrayed caregivers. They matched what has traditionally been described as the "average” caregiver. Female. Middle-aged. Middle class. And white.
I observed that most movies, shows and books about caregiving depict white families in white neighborhoods (think: Steel Magnolias, The Notebook). Usually, they're wealthy. They have nice gardens and lakes with docks and in-home nurses. And, often, relatives who can take weeks off of work to visit while the family decides whether to send their loved one to a nursing home (that they can pay for!). I am a white, female, middle class woman, and those depictions do not represent my caregiving experiences. In fact, I don't believe they represent most caregiver experiences.
Improve the research
It's not just how caregivers are portrayed. It's also how they are studied. In the past, caregiving research centered around Caucasian caregivers. There was a "major deficit” in research regarding nonwhite caregivers. Over time, there has been an evolving body of scientific and social research that explores the needs and experiences of all variations and circumstances of caregiving. And yet, the common depictions of caregivers and outreach efforts to the caregiving population has not yet caught up to the reality of caregiving in America and certainly not to the reality of the upcoming caregiving cliff. AARP has recognized the need to speak to diverse communities and has created guides catered to Chinese, Spanish, Asian American, LGBT and military caregivers.






































































More From AARP
Caregivers Need More Support
Medical professionals often don't ask how they can help
Latinos Realizing That Hospice Fits With Their End-of-Life Philosophy
Compassionate medical care focuses on the dignity and desires of each patient