AARP Hearing Center
Do You Need a Bone Scan?
Catching and treating weakening bones can be lifesaving in older adults

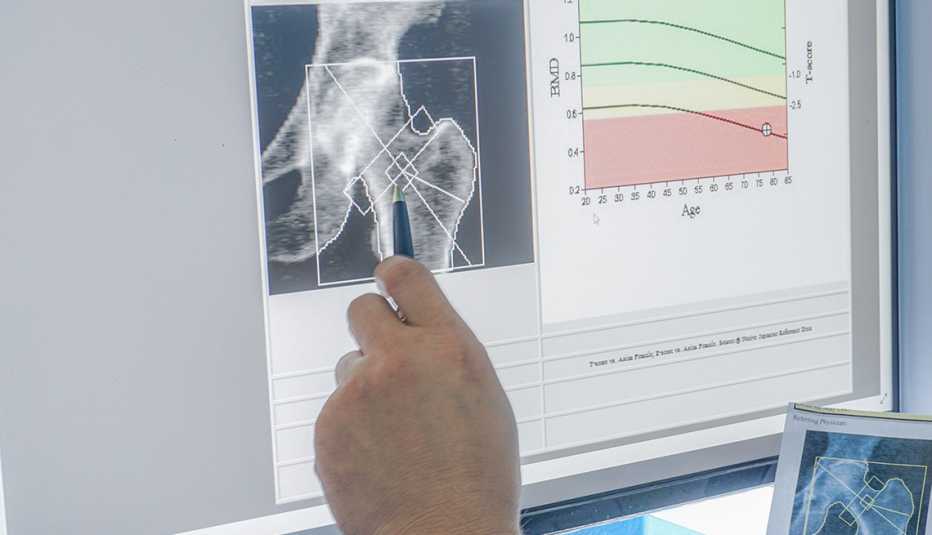
Like many other health screenings, scans that check for osteoporosis, a disease marked by weak and brittle bones, fell by the wayside during the pandemic, according to a 2021 study published in the Journal of Clinical Endocrinology and Metabolism. But the condition itself doesn’t take any time off.
One in 2 women and up to 1 in 4 men will break a bone due to osteoporosis, according to the National Osteoporosis Foundation. A woman’s risk of fracture is equal to her combined risk of breast, uterine and ovarian cancer, and a man is more likely to break a bone due to osteoporosis than he is to get prostate cancer.
Some of these fractures can be life-altering, even deadly. About a quarter of hip fracture patients end up in nursing homes, and 24 percent of hip fracture patients 50 and over die within a year after the fracture.
But there’s an easy way to figure out if you’re at risk for an osteoporosis-related fracture: have a bone density test, which measures how strong your bones are, says Robert Adler, M.D., an endocrinologist at Virginia Commonwealth University in Richmond, Virginia.
When should you get your first bone density scan?
The answer depends on your gender, Adler says. Age is also an important factor.
For women:
Groups like the United States Preventative Services Task Force, the Bone Health and Osteoporosis Foundation and the North American Menopause Society all recommend osteoporosis screening for postmenopausal women who are 65 or older. But you may need to get that first scan earlier if you have any of the following risk factors.
- You’re a current or former smoker
- You use steroid medications like prednisone
- You’re underweight
- You have rheumatoid arthritis
- You’ve had a nontraumatic bone fracture (you’ve broken a bone after you fell from less than standing height)
- You regularly have at least three alcoholic drinks a day
- You have a chronic condition such as diabetes, thyroid disease or liver disease, or you went through early menopause.
If you don’t check any of these boxes, there’s no need to get that initial screen earlier. “There’s almost a knee-jerk reflex among many providers to order a bone density scan [before age 65], since we do know that osteoporosis and fractures are more common after menopause,” Adler says. But there’s no evidence that it helps, he notes.
For men:
Men can get osteoporosis, too, and its effects can be deadlier than in women. But there are no clear guidelines as to when men should get screened.


The Bone Health and Osteoporosis Foundation recommends that all men have a baseline bone density test at age 70, and even earlier (between the ages of 50 and 69) if they have risk factors, like the ones mentioned above. Other research, however, suggests that may not be necessary, Adler says.
A 2018 study published in Mayo Clinic Proceedings found that bone density tests in men ages 65 to 99 didn’t reduce risk of fracture unless they were 80 or older or had other risk factors such as being on steroids or having low testosterone. Adler recommends his male patients get a scan at age 80, or between 70 or 80 if they have any risk factors.
Which test is best?
There are three types of bone density tests.
Dual-energy X-ray absorptiometry. A DEXA scan is considered the gold standard when it comes to bone density tests, says osteoporosis expert Clifford Rosen, M.D., director of clinical and translational research at the Maine Medical Center’s Research Institute. It’s a specialized kind of X-ray that provides a very precise measurement of bone density at sites like your spine, hip and forearm. When it’s time for a follow-up exam, Rosen recommends going to the same center to ensure accuracy. Bone density measurements are easier to compare if they’re done on the same model.
Quantitative computerized tomography. This is a type of CT scan that measures bone density in the spine. While it’s very accurate, it’s expensive and requires a higher radiation dose than a DEXA scan.
Ultrasonography. While your doctor can use ultrasound to measure the bone density of your heel, it’s not routinely recommended because there aren’t guidelines that use ultrasound to diagnose osteoporosis. It may be done in areas where DEXA scans aren’t widely available.
Researchers are also exploring whether chest or abdominal CT scans can be used to calculate bone density. “It may be an alternative way to get this information for someone who hasn’t had a DEXA scan, but had a CT scan for something else,” Adler explains.
What Your Results Mean
After you have a bone density scan, you’ll be given what’s known as a T score. This compares the condition of your bones with a young healthy person. The lower your score, the higher your risk is for a fracture. Here’s a quick look at what these results mean.
Normal bone density. If you fall into this category, your T-score is between +1 and -1. You’ll still need to take steps to prevent bone loss, like getting enough calcium and vitamin D and doing weight-bearing exercise.
Low bone mass (osteopenia). If your T-score is between -1.1 and -2.4, you don’t have osteoporosis yet, but are at risk. Your doctor will talk to you about steps you can take to prevent osteoporosis, which includes lifestyle changes and sometimes even medications.
Osteoporosis. This is a T-score of -2.5 or less. Your doctor will usually recommend osteoporosis medications, calcium and vitamin D supplements, along with an exercise program.
What about follow-up scans?
If you do have osteoporosis, your doctor will most likely want you to have a repeat scan in two years.
“We want to see if there is evidence that the medication you’re on is working, and it’s also a good time to have a conversation with your provider about whether you’ve been able to adhere to therapy,” Adler says. Your doctor may also recommend repeat testing in two years even if you don’t have osteoporosis but have a medical condition that puts you at increased risk of a fracture.
If you have osteopenia, most experts recommend that you have a repeat test in three to five years, to make sure the condition isn’t progressing.
There are no set recommendations on how often to have a repeat bone scan if your original one was normal. But in general, it’s still a good idea to have a repeat scan in about five years, Rosen advises.
“Women on average lose about 1 percent of their bone every year, which is significant,” he explains. If you break a bone before your five-year follow-up, get another bone mineral density test. Research from the Bone Health and Osteoporosis Foundation has found that only 5 percent of men and 9 percent of women using traditional Medicare received a bone mineral density test within six months following a new fracture. “You don’t want to go on to have a second, more serious fracture that lands you in a nursing home,” Rosen stresses.

































































MORE ON HEALTH
7 Arm Workouts for Building Strength
This easy upper-body workout may help you feel (and look) stronger