AARP Hearing Center
Could That Pain in Your Gut Be Diverticulitis?
If you are among millions with underlying risk factors, a sudden attack could be in your future

As we age, most of us notice changes such as graying hair and wrinkling skin. But there’s another common, usually harmless change many people never notice: the development of pouches inside the colon.
These pouches, which can turn the smooth inner colon lining into something resembling Swiss cheese, are called diverticula. The condition — which may have multiple causes, including low-fiber diets — is called diverticulosis. And in the United States, more than 30 percent of people in their 50s and more than 70 percent of people older than 80 have it, according to the National Institute of Diabetes and Digestive and Kidney Diseases.
Some people find out they have diverticulosis when they have a routine colonoscopy to screen for cancer. But an unlucky few find out when one day, seemingly out of the blue, they have the unpleasant and painful symptoms of diverticulitis — an inflammation or infection of the pouches.
An attack of diverticulitis is usually “a pretty intense event,” says Lisa Strate, M.D., a professor of medicine at the University of Washington and a gastroenterologist at Harborview Medical Center in Seattle. Fortunately, she says, fewer than 5 percent of people with diverticulosis ever experience diverticulitis. And most people who get sick never have a second attack.
People with diverticulitis also are less likely these days than in the past to be hospitalized or prescribed antibiotics, says Neil Stollman, M.D., a gastroenterologist at Alta Bates Summit Medical Center in Oakland, California, and an associate clinical professor of medicine at the University of California San Francisco. Many people may be surprised to learn that after they recover from the initial attack, they don’t need to limit their diets in ways once thought necessary, he says.
But if you develop symptoms that could be diverticulitis, your immediate concern won’t be what you can eat for the rest of your life; it will be getting relief. These telltale symptoms should send you to your primary care provider or an emergency room for help.
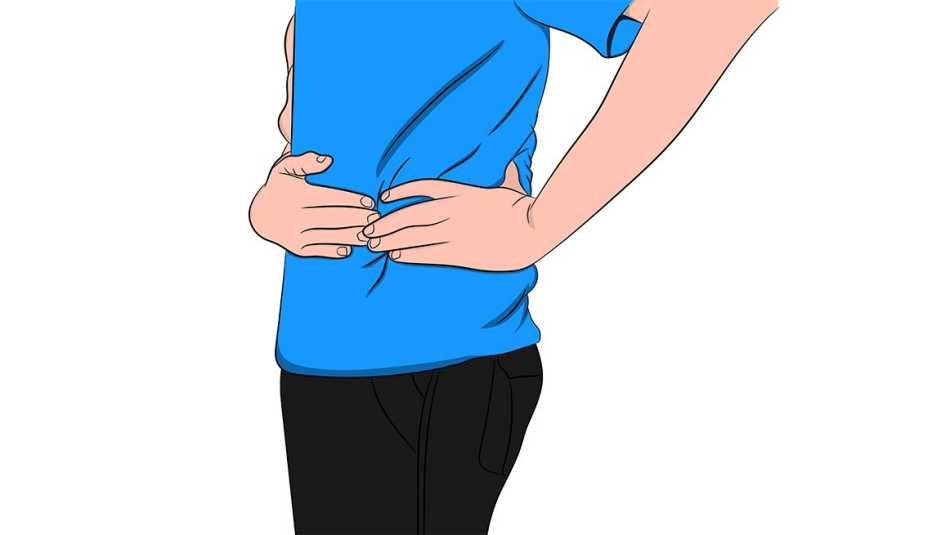
- Pain in your abdomen, usually, but not always, on the left lower side. The pain develops there because that’s the area of the colon most likely to develop pouches, at least among people in the U.S., Strate says. Right-sided diverticulitis is more common in Asia.
- Development of the pain over a day or two. While people who have other conditions, including irritable bowel syndrome, can have gut discomfort on and off for years, diverticulitis pain develops more suddenly, Stollman says.
- A feeling that the pain is worse than usual gassiness or bloating. As the pain escalates, it gets pretty severe, “to the point where people are doubled over,” Stollman says. The affected part of your lower belly also may hurt when you press on it or if you are jarred, for example, during a bumpy car ride, Strate says.
- Additional symptoms that can include fatigue, nausea, a low-grade fever, and diarrhea or constipation. Vomiting, which is usually a sign of trouble higher in your digestive tract, is less likely, according to Strate and Stollman.
Getting diagnosed and treated: What to expect
The symptoms of diverticulitis are so distinct that doctors can often make a correct diagnosis without doing any tests, Strate and Stollman say. That’s especially true if the doctor already knows the patient has diverticulosis. Still, professional groups of gastroenterologists and other doctors recommend some testing to rule out other problems and to verify that diverticulitis is, in fact, the culprit.


The best way to confirm the diagnosis, these groups say, is with a CT scan, which can show diverticular pouches and inflammation. You should also expect blood tests to check for signs of inflammation and infection. After initial treatment and recovery, you might also get a colonoscopy to make sure you don’t have cancer or another problem.
In the past, virtually everyone diagnosed with diverticulitis got antibiotics, because doctors believed the illness was caused by infection. Treatment guidelines no longer recommend that. The reason: Multiple studies have shown that people treated without antibiotics recover just as quickly and with the same complication rate as people who get the medications, Stollman says.
That suggests, he adds, that the underlying problem for most people may be inflammation, not infection. Since antibiotics have risks and side effects, including the disruption of healthy gut bacteria, the downsides often outweigh any possible benefit.
In practice, many people still get antibiotics for diverticulitis, Stollman says. But now it’s an individual decision, based on several factors, including whether you have signs of infection and whether your age and other health conditions put you at high risk for complications.
Most people with diverticulitis start to feel better within a couple of days and recover within 10 to 12 days, Strate says. During that period, doctors usually recommend a liquid diet, gradually transitioning to soft, bland foods. Over-the-counter painkillers containing acetaminophen are OK, but treatment guidelines warn against using nonsteroidal anti-inflammatory drugs, such as ibuprofen and naproxen, because they have been linked to the development of diverticulitis.
Some doctors prescribe anti-spasm medications to control cramping. Old-fashioned soothers such as peppermint and heating pads can also help, Stollman says.
Complications and recurrences
About 12 percent of people with diverticulitis have immediate complications, such as a pus-filled abscess, an infection of the abdominal lining or swelling so severe that it blocks the colon, according to the American Gastroenterological Association. Those people can expect to be hospitalized; some will need surgery. Deaths from diverticulitis are rare, Stollman says, and most often related to surgical complications.
Once the initial crisis passes, patients are eager to know what they can do to prevent a repeat attack. The chance of a second attack within 10 years is about 20 percent, research suggests. Once someone has had two attacks, they are at higher risk for more, and the risk grows with each subsequent episode. For that reason, some people choose to have surgery to remove the affected section of the colon. Research on the most appropriate use of these elective surgeries is ongoing.
No medication or supplement has been shown to prevent recurrences of diverticulitis. And some dietary advice given to patients in the past — most notably that eating nuts, seeds and popcorn increases the risk of diverticulitis — has been proven wrong. People who eat some of those foods actually seem to have a lower risk, research suggests.
Instead, doctors recommend that people at risk for diverticulitis:
- Eat a diet with plenty of fiber (fruits, vegetables, grains and legumes) and with not too much red meat.
- Get plenty of exercise. Vigorous exercise may be especially helpful.
- Maintain a healthy weight.
- Refrain from smoking.
- Avoid non-steroidal anti-inflammatory drugs. An exception: aspirin for heart attack and stroke prevention, if recommended by your doctor.
Some people feel frustrated and guilty when they have repeated attacks despite a healthful lifestyle, Strate says. It can help to know, she says, that about 50 percent of the risk for diverticulitis is genetic.
A diverticular emergency: Bleeding
About 70,000 people in the U.S. each year are hospitalized for what can be an alarming complication of diverticulosis: sudden bleeding from the rectum. Diverticular bleeding occurs when a blood vessel spanning one of the pouches bursts. It’s not usually related to diverticulitis, a different complication caused by inflammation or infection.
Though most people recover, even without treatment, the bleeding can be severe and life-threatening, according to the National Institute of Diabetes and Digestive and Kidney Diseases. Treatment can include blood transfusions and procedures to stop the bleeding. Those procedures can often be done during a colonoscopy performed to confirm the diagnosis.
After an attack of diverticulitis, some people have ongoing symptoms that are less severe, such as bloating and cramping. A leading theory is that the colon becomes more sensitive after diverticulitis, causing symptoms similar to those of irritable bowel syndrome.
Some people with diverticulosis but no history of diverticulitis also report such digestive problems. However, it’s unclear whether their symptoms are caused by the condition, experts say.

































































MORE FROM AARP
8 Warning Signs of Colorectal Cancer
Plus, risks and screening recommendations
Symptoms You Shouldn't Ignore for Health
Digestive symptoms that may indicate serious health issues