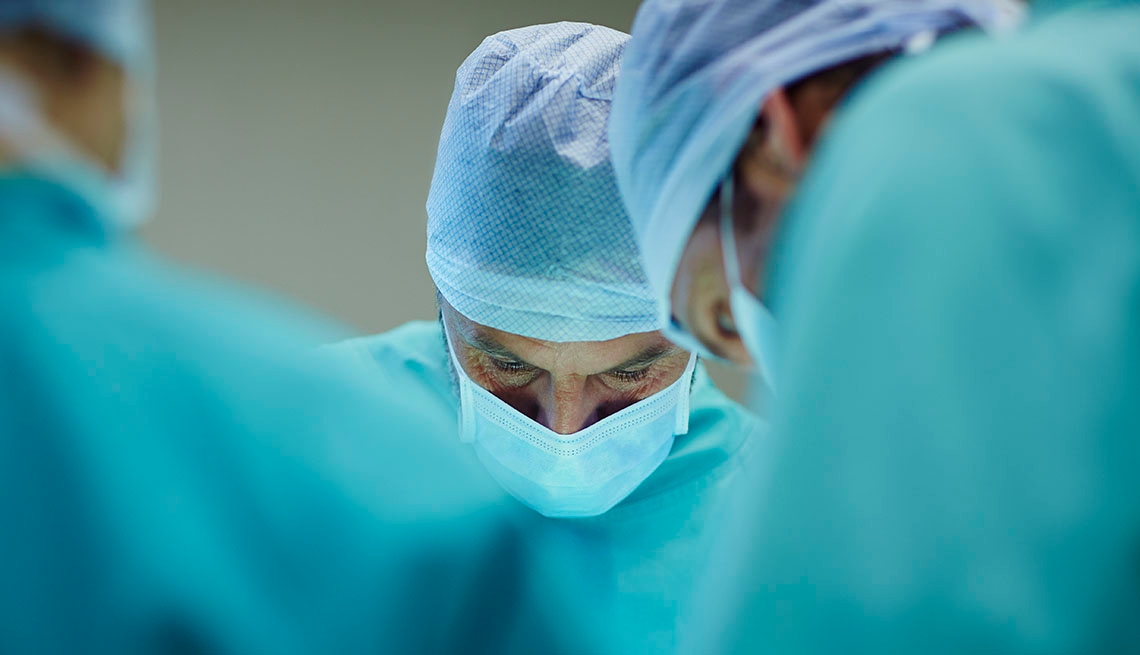
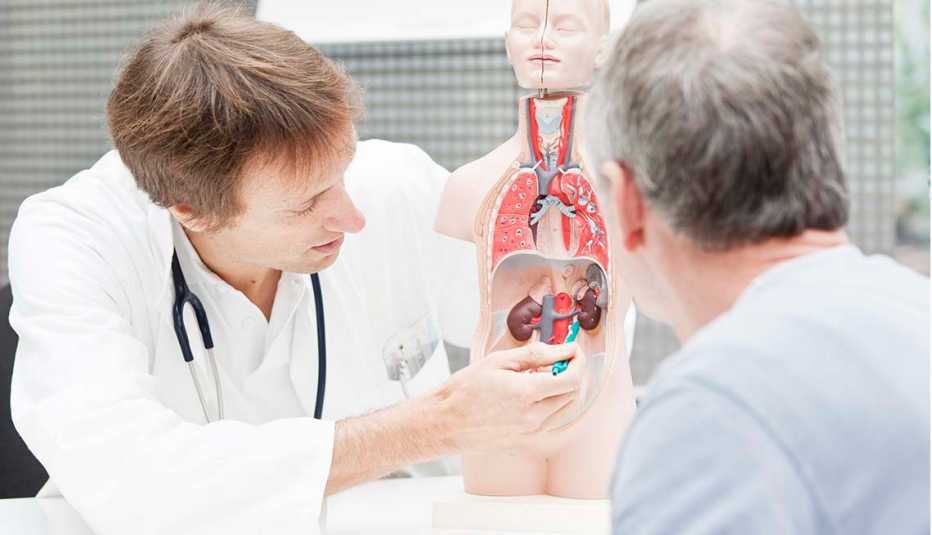
Under this program, concerns specific to elderly patients would be addressed before they’re even wheeled into the operating room. Patients would be screened for geriatric vulnerabilities, among them frailty and cognitive issues, such as pre-delirium and dementia. Exercise and nutritional programs are put in place to help ensure patients are stronger after surgery and able to recuperate more quickly. Geriatric-friendly rooms are equipped with skid-free floors, clocks with large, easy-to-read numbers and beds outfitted with railings high enough to keep patients safe.
“Patients who are 75 years of age and older are at the greatest risk for functional decline and have the highest chance of needing to go to a nursing home or rehab center after their hospital stay,” says Tom Robinson, chief of surgery at the VA Eastern Colorado Health Care System, one of eight hospitals that have tested the standards. Now a team of nurses at the Denver VA hospital makes daily rounds, checks on elderly patients and makes sure that the care that’s being delivered is in line with their health care goals. They take steps to prevent delirium and get the patient up and moving around to prevent further complications such as falls, because they’re unsteady, and pressure ulcers, from being in bed too long.
They also carefully monitor the patient’s medication. “Many older people are on five or more medications to begin with,” Rosenthal says. “During the surgical process, more may be introduced, which should be used cautiously, if at all, in older patients since some can promote confusion.”
Under the GSV Program, care continues after the patient has been discharged. “When we think about surgery, too often we think short term — the operation and post-operative care,” says Clifford Ko, professor of surgery and health services at the UCLA Schools of Medicine and Public Health, and director of the ACS National Surgical Quality Improvement Program. “What we need to focus on, perhaps even more, is post-discharge. How is the person doing after they leave the hospital? How are they functioning?”
At Denver’s VA hospital, more patients are able to return home, rather than being moved to a facility. One example: A 92-year-old man who had a tumor removed from his tongue. Even before his surgery, a proactive team of providers went to assess his house and set up safety features, such as handrails, so he would be able to maintain his independence. When he was discharged, social workers were ready for him and sent a nurse to his house to give him extra assistance.
The standards for this kind of care have been posted on the ACS website for hospitals to review before the enrollment opens in October. Feedback from hospitals that have tested the standards has been positive. “One of our beta pilots is planning on enrolling all of their hospitals,” says Rosenthal. “I think the teams have bought into the idea that this is bringing order to how older patients are cared for, and that everyone understands what is important to them.”
Once a hospital enrolls, there will be site visits to ensure that standards are being met. Seniors and their families will be able to go to the ACS website to see which hospitals are in the program and are successful. “Hopefully, it will give them some level of assurance,” says Ko. “They can feel confident about the hospital they’re going to for treatment.”