AARP Hearing Center

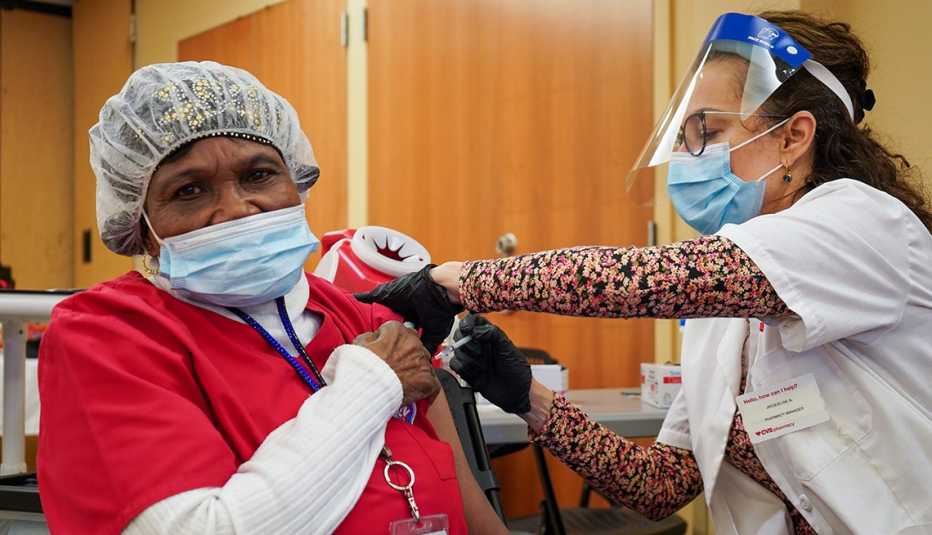
In early August, after months of deliberation, Christian Living Communities announced it was requiring all workers at its six long-term care communities in Colorado to be fully vaccinated against COVID-19. If employees didn’t get the shots — or a valid religious or medical exemption — by Oct. 1, they’d no longer have a job.
At most of the facilities, the mandate had the intended effect: vaccinations ticked up. But at one facility in rural Colorado, many workers wouldn’t budge. So the nonprofit chain pushed the deadline out to the end of October.
“We can’t have no team members,” said Jill Vitale-Aussem, president and chief executive officer of Christian Living Communities, who worried that many workers at the facilities would walk. “Yes, we have a risk with them being unvaccinated, but we also have a huge risk if we don’t have them to care for the residents.”
“It’s hard,” she said. “There are risks both ways.”
As they did at Christian Living Communities facilities, vaccine mandates at nursing homes around the country appear to be pushing vaccinations up. The national vaccination rate for nursing home staff jumped from 67 to 74 percent between mid-September and mid-October, according to an AARP analysis of government data, as a wave of nursing home chains, individual facilities and states activated the requirements for workers. That’s the largest monthly increase since AARP began tracking COVID-19 vaccination data in June.
A federal mandate for most staff in health care facilities that receive Medicare or Medicaid dollars, which includes nursing homes, will also take effect in early January.
But even as the mandates appear to be working, many long-term care operators say they are intensifying staffing shortages. That’s especially true in pockets of the country where vaccine hesitancy is high. While shortages and high turnover have long plagued the long-term care workforce, the pandemic has exacerbated them, raising more concerns about inadequate care for residents. The pandemic has killed more than 186,000 residents and staff of long-term care facilities, including nursing homes, assisted living facilities and other settings, representing more than a quarter of all U.S. coronavirus deaths.
Almost a third of the nation’s 15,000-plus nursing homes recently reported a shortage of nurses or aides, according to AARP’s analysis, representing the worst monthly shortfall since the government began collecting COVID-19 data from nursing homes in May 2020. In Maine, Washington and Minnesota, more than 60 percent of facilities reported shortages. In Alaska, 81 percent did.
A recent survey of 1,200 senior care providers by the American Health Care Association and National Center for Assisted Living (AHCA/NCAL), which lobbies on behalf of more than 14,000 nursing homes and long-term care facilities nationwide, paints an even bleaker picture: 99 percent of nursing homes and 96 percent of assisted living facilities said they didn’t have enough workers. And more than a third of nursing homes said they were very concerned that the issue might force them to close.
“While we support the overall intent of this [federal] policy, we are concerned that the execution will exacerbate an already dire workforce crisis in long-term care,” Mark Parkinson, president and chief executive officer of AHCA/NCAL, said of the federal mandate.
A building wave of vaccine mandates
Requirements that long-term care staffers get inoculated have been scattered. A few private companies acted early, handing them down to employees as soon as residents and staff were prioritized for COVID-19 vaccines at the end of last year. When vaccine availability increased and more data emerged on the safety and efficacy of shots, more companies followed suit.
After California introduced the first statewide vaccine mandate for health care workers, including those in nursing homes, in early August, more states jumped on board. Now around half of all states have active mandates of some kind, though many offer regular testing and masking as an alternative to full vaccination.
President Biden announced in mid-August that all U.S. nursing homes that receive federal Medicare and Medicaid funding — the vast majority of facilities — must require their workers to be fully vaccinated against COVID-19. The move followed AARP calls for requiring nursing home staff and residents to be vaccinated. More recently, the Biden administration announced a Jan. 4 deadline for worker compliance, with no option to test out. Assisted living, memory care and other long-term care facilities are regulated by the states and are not subject to the federal mandate.
The mandates have clearly prompted more vaccinations. As of mid-October, staff vaccination rates exceeded 90 percent in Connecticut, Washington, D.C., Massachusetts, Maine and Rhode Island, where vaccinate-or-terminate policies have been adopted. Rates also exceeded 90 percent in California and Hawaii, which have a regular test-out alternatives to full vaccination.









































































More on caregiving
Nursing Homes are Filled with Empty Beds, Raising More Concerns About Care
Ravaged by COVID-19, facilities with high vacancy are strugglingAction Needed Now on Long-Term Care Reform
America's outdated care system is in dire need of an overhaulChoosing the Right Long-Term Care Facility
Research location, staffing, cleanliness protocols and much more