AARP Hearing Center
The urgent call for more people to get a flu shot in advance of this year’s flu season comes against a discouraging backdrop of already low vaccination rates in the U.S. The annual vaccination rate among older adults ages 50+ stands at just 56 percent, even as the Centers for Disease Control and Prevention calls out this group as having much to gain from an annual flu shot. The rate was 50 percent 10 years ago, showing only a modest increase over the past decade.

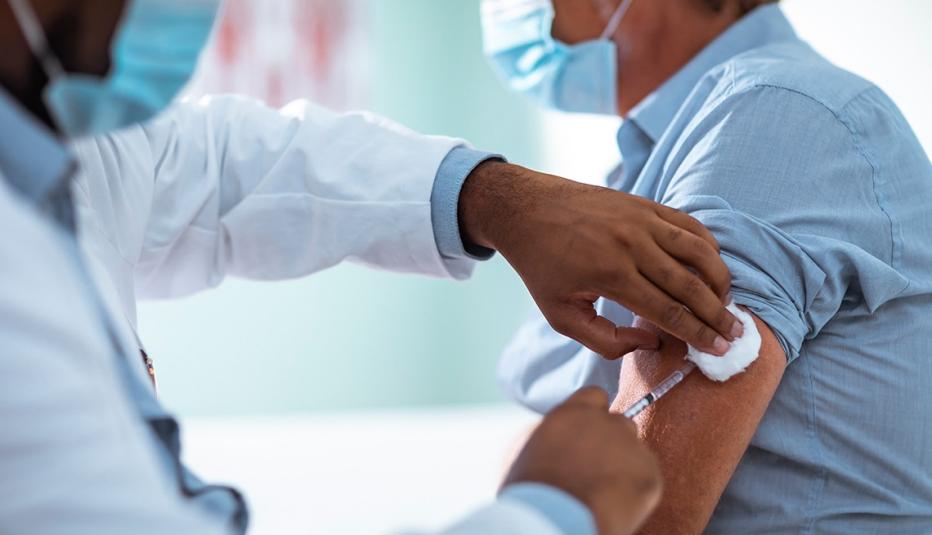
Of course, the call is particularly urgent this year because of the COVID-19 pandemic. Older adults, the group most at risk for serious illness and death from COVID-19, are, in effort to avoid contagion, postponing routine medical visits and pharmacy trips, both of which are opportunities to get an annual influenza vaccine. But if vaccination uptake rates do not improve, cases of the flu could further strain hospitals dealing with COVID-19 cases.
Behind the Low Vaccination Rates
Multiple factors contribute to flu vaccination uptake rates. A recent AARP survey of adults 50 and older showed that attitudes and beliefs that drive personal choice were the highest ranking factors behind foregoing an annual flu shot. Respondents cited a lack of interest (44 percent), concern about possible side effects (38 percent), concern about safety and efficacy (38 percent), a belief that the flu vaccine isn’t needed (31 percent), and previous flu experience (28 percent) as the strongest factors.
Data also reveals disparities by both race and ethnicity, a reality having implications when considering strategies to increase vaccination rates. Over the past decade, older adults identifying as White or non-Hispanic were consistently more likely to be vaccinated against the flu than their Black or Hispanic counterparts. Lower immunization adherence among certain racial and ethnic groups may, in part, be rooted in systemic barriers that prevent some individuals from accessing preventive services and contribute to a lack of trust in the health care system. Lack of access to health care providers, costs associated with flu vaccines, as well as missing, inconsistent, and/or misleading information also pose significant barriers to vaccination.
The Numbers Across Groups
- In 2018, flu vaccinations in adults ages 50 to 64 were 18 percent higher in Whites than Blacks and 15 percent higher in non-Hispanics than Hispanics.
- In 2018, flu vaccinations in adults ages 65 and older were 17 percent higher in Whites than Blacks and 10 percent higher in non-Hispanics than Hispanics
- Older adults with private insurance were most likely among their age cohort to receive a vaccine – 46 percent for persons ages 50 to 64 and 69 percent for those 65 and older.
- Older adults with Medicaid coverage were least likely among those with insurance coverage to receive a vaccine – 44 percent for adults ages 50 to 64 and 50 percent for those 65 and older.
- Of the 9 percent of uninsured adults ages 50 to 64, less than a quarter received a vaccination in 2018.
- Fully 3.8 million uninsured adults ages 50 to 64 went without a vaccine in 2018.
- Among adults age 50, the highest vaccination rates are connected to some form of Medicare coverage.
- Further analysis could show the extent to which Medicare’s benefits influence vaccination.
Conclusion
Year after year, around 50 million older adults go without a flu vaccine, a figure that takes on added importance in the context of the COVID-19 pandemic. We may see vaccination rates remain steady or dip during the 2020-21 flu season and beyond unless policy makers take active and concrete measures to address these new challenges as well as historic barriers that continue to affect flu vaccination rates.








































































