AARP Hearing Center
| Warmer days don’t just mean the arrival of spring. If you have seasonal allergies, warm weather may also signal the arrival of watery eyes, sneezing, congestion, headache and maybe even a cough.
With the continuing pandemic and allergy season starting earlier than usual in many parts of the country, there may be times when you’re not sure if your symptoms are due to allergies or to COVID-19.
It’s an understandable concern because they share many symptoms, says Panagis Galiatsatos, M.D., a physician in the Division of Pulmonary and Critical Care Medicine at Johns Hopkins Medicine. Overlapping symptoms include headache, sore throat, congestion, runny nose and cough.
The U.S. Centers for Disease Control and Prevention (CDC) offers this Venn diagram that shows the symptoms unique to each condition, and which symptoms they share:
Coronavirus vs. allergy symptoms

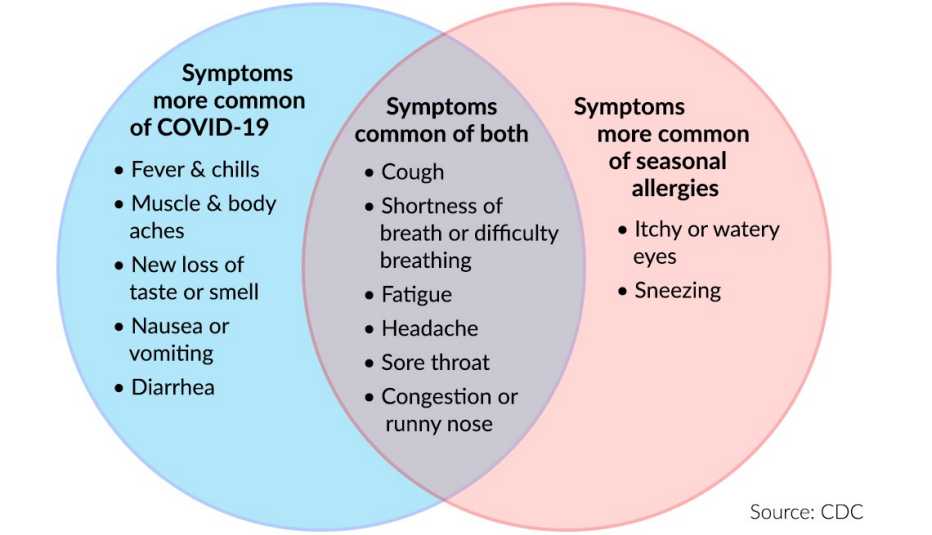
How can you tell the difference between seasonal allergies and COVID-19 symptoms? If you have a fever and chills, that can indicate an infection, so you should definitely get a coronavirus test, Galiatsatos says. The same goes if you lose your sense of taste or smell.
Allergies are rarely associated with a fever. They usually affect your upper respiratory system, Galiatsatos says, so you’re more likely to have itchy, watery eyes and a runny nose.
“Most people with seasonal allergies know their symptoms; it’s almost like a Spidey sense,” Galiatsatos adds. “If it’s what you feel every year, it’s probably not COVID.”
Milwaukee allergist Gary Steven, M.D., recommends paying attention to what makes your symptoms worse. “If you're fine when you're indoors and the windows are closed, but then you go out on a dry, windy day and start sneezing your head off, yes, that's an allergy.”
If you’re still uncertain, though, there’s no downside to getting a COVID-19 test.








































































