AARP Hearing Center
Nursing Homes’ Flawed Business Model Worsens COVID Crisis
To understand the industry’s shortcomings, look at laws going back 85 years


It’s tempting to heap blame on the owners of America’s nursing homes—to argue that the pursuit of profits led to poor care and so many coronavirus-related deaths.
The reality, however, is more complex.
AARP asked me to explore the business of nursing homes and the culpability of their owners for what has transpired. Clearly most operators reacted to the pandemic as best they could. But what I found was that the industry’s complex and murky financial structure fails to safeguard the health of residents and staff.
While the overall profits reaped by owners are secret, COVID-19 is clearly hurting nursing homes financially. Fully 55 percent of them claim to be losing money, and 72 percent say they may not be able to sustain operations for another year, according to an August survey by the American Health Care Association and the National Center for Assisted Living.
Even the nation’s largest nursing home chain, Genesis HealthCare, says it’s in jeopardy. Genesis, with 360 facilities in 25 states, said in August there was “substantial doubt” about its ability to survive for the next 12 months.
“If there isn’t more money coming in, many members will face decisions about shrinking the number of beds or even closing their doors,” says Katie Smith Sloan, CEO of LeadingAge, an organization that represents nonprofit nursing homes.
Here is what you need to know to understand the business of nursing homes, and to what extent they caused the mess they are in.
The Industry is Vast


The nation’s 15,600 nursing homes generated about $166 billion in revenue in 2017—a little more than what U.S. hotels took in by renting out their rooms. And nursing homes receive about the same amount for most of their residents as nice hotels get for a night’s stay.
But the similarities end there. For example, roughly 30 percent of nursing homes are owned by nonprofit organizations predominantly affiliated with religious groups, ethnic aid societies and social service agencies. They strive to maximize revenue and efficiency, but any unspent revenue is used to improve and expand their facilities and services.
The remaining 70 percent of homes are for-profit — free to pay out income to owners once they cover operating expenses and other obligations. Owners include national chains, regional chains and stand-alone facilities. About 1 in 7 for-profit homes are controlled by private equity investors — something that can be problematic, as I’ll explain shortly.
Medicaid is a Mainstay


To understand nursing homes’ finances, you have to start with their revenue. Three-fifths of the nation’s 1.3 million nursing home residents’ fees are paid by Medicaid, the federal-state insurance program for low-income Americans. These older adults (and people with disabilities) often spend their remaining years in a nursing home, at taxpayers’ expense.
How profitable is the Medicaid business? It depends on whom you ask. The average Medicaid payment, which varies by state, is around $200 per resident per day. But unlike a hotel charging that price, nursing homes have to provide hands-on care that many residents need with their daily activities. They also must provide meals, medical services and more.
Nursing home operators consistently say that $200 doesn’t cover their costs. Industry critics aren’t so quick to agree, citing owners’ opaque finances and multiple income sources (more on that later). “We don’t know whether Medicaid rates are too low or not,” says
Charlene Harrington, a University of California, San Francisco, professor emerita who has studied nursing homes for decades.
What is clear is that the share of this revenue spent on paying and training personnel isn’t enough. The industry’s staff turnover is high, and there’s a critical shortage of people qualified to provide patient care. This detracts from residents’ well-being at any time, but it’s proven especially dangerous in 2020.


And $200 a day isn’t enough to fund a deep well of supplies or to have private rooms available that might reduce the spread of infection. It has been especially inadequate this year, when facilities faced suddenly skyrocketing costs for infection-control supplies and tests.
Well before the coronavirus blindsided the industry, the numbers were bleak. Consider the most recent report of the government’s Medicare Payment Advisory Commission. In 2018, MedPAC found, nursing homes had an operating profit margin of negative 3 percent on patients paid for by Medicaid and other non-Medicare sources. In other words, for every $100 they took in for these residents, they spent $103 on their care — clearly a losing proposition. During the pandemic, no doubt the math got worse.

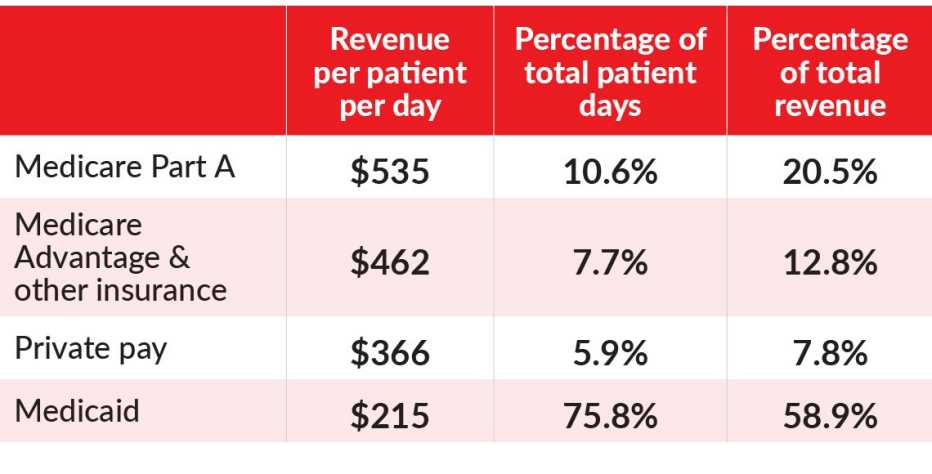
A Lopsided Model
Medicare pays for relatively few nursing home residents, but provides a major portion of the home’s revenue. These figures show 2019 inpatient revenue for Genesis Health Care, the nation’s largest chain.
The Money is in Medicare


If caring for Medicaid residents is such a poor business, how have nursing homes stayed afloat all these years? The answer is, chiefly, Medicare. While Medicare doesn’t pay for long-term nursing home care, it does cover skilled services and therapy for up to 100 days after a patient is discharged from a hospital. And it pays very well. In 2019, for example, Genesis HealthCare received $535 per resident per day from Medicare — about 2½ times the $215 it got for Medicaid patients.
Yes, Medicare residents usually need more care than Medicaid residents. Even so, Medicare is more profitable: For every $100 that nursing homes receive on behalf of these patients, an average of $10 is left over after subtracting the cost of the care — not a loss of $3.
The upshot is that nursing homes rely on a relatively small number of well-paying residents to make up for the money they say they lose on the rest. “It’s not a structure anyone would have designed from the outset,” says R. Tamara Konetzka, a professor of health services research at the University of Chicago.
Not surprisingly, nursing homes strive to admit more Medicare patients to offset what they say are losses on Medicaid. But that can lead to bad care decisions, Konetzka says, such as encouraging nursing homes to send Medicaid residents to the hospital so they can return as higher-paying Medicare patients.
This year, some nursing homes evicted Medicaid residents in favor of COVID-19 patients receiving care at the higher Medicare rate, according to The New York Times and other news outlets. Inappropriate discharges have long been a top complaint to long-term care ombudsmen nationwide; AARP Foundation has fought the practice in the courts.
The Pandemic Has Hurt


This dependence on Medicare patients has proven hazardous for nursing homes this year. Starting in March, hospitals and patients canceled or delayed many elective procedures, and roughly 10 percent fewer Medicare patients were sent to skilled nursing facilities for rehabilitation, according to MedPAC. Overall nursing home occupancy dropped from 83.4 percent to 74.8 percent from March through June, according to the National Investment Center for Seniors Housing & Care, a research group that compiles nursing home data for investors.
Between May and October, the federal government pumped more than $21 billion into the industry in the form of grants, loans and advance Medicare payments. Only $2.5 billion of that had usage stipulations; it’s unknown how much of the aid went to stop the spread of COVID-19. “Nursing homes can use it to shore up their bottom lines if they want to,” says Elaine Ryan, AARP’s vice president of government affairs for state advocacy. “We might never know where the money went.”
Profits and Private Equity Can Eat Into Care


Beyond the problematic payment system, researchers and policymakers question whether the for-profit ownership structure of most nursing homes is the best model for delivering care.
A number of research studies have found that for-profit nursing homes generally have significantly lower staffing levels and quality of care than nonprofit facilities, as measured by the Nursing Home Compare quality star rating system run by the government’s Centers for Medicare & Medicaid Services (CMS).
Of particular concern to industry followers are the estimated 10 percent of America’s nursing homes owned by private equity (PE) investment groups. Bankrolled by institutional investors and wealthy individuals, these PE firms typically buy businesses, make efficiency and/or cost-cutting changes to increase their apparent value, then sell them within three to five years. PE firms often borrow money against the businesses’ assets and receive management fees as well as a share of profits when the enterprises are sold.
Here’s their usual practice as it pertains to nursing homes, according to Harvard University professor of health care policy David Grabowski and other researchers: A firm will buy a nursing home, then place its buildings and other real estate — nursing homes’ most valuable asset— in a separate holding company. Other companies also owned by the investors will start providing management, laundry, supplies and other services to the nursing home. These ownership structures make it hard to figure out who is responsible for the quality of care and how to recover damages if a resident is injured, says Ashvin Gandhi, a health economist at UCLA who has studied private equity and nursing homes.
Once a nursing home starts paying these related companies, says Grabowski, the home may appear to be struggling, while at the same time the owners are making money from their other entities. The nursing home itself ends up saddled with debts incurred to pay off lenders who financed the PE firm’s purchase.
“The main reason these for-profit companies are in the nursing home business is to extract money through management contracts and lease agreements,” UCSF’s Harrington says. “They scream they have no money, but they’ve legally taken money out through all these related-party transactions.”
Deals like these have been going on for more than 20 years. Other for-profit firms have engaged in similar practices, separating out their real estate holdings and striking management and supply deals with related firms.
“Every dollar they squeeze out of a nursing home for profit is a dollar that isn’t going to the care of the residents,” says Patrick Woodall, a senior researcher at Americans for Financial Reform, a national coalition of consumer and civil rights groups.
There is No Quick Fix
Solutions, sadly, seem far off. “People get concerned when stories of poor nursing home care come out,” Konetzka says. “But politicians never run for office on a platform of raising taxes to improve Medicaid reimbursement.”
The industry itself isn’t always eager for change; it often lobbies at both the federal and state levels to oppose long-term care reforms.
Ultimately, a group effort will be necessary, says Bob Kramer, founder of the National Investment Center for Seniors Housing & Care: “It will take partnerships between the federal government, states, the long-term care industry and insurers to change the system and ensure that people can afford the care they need.”
When Private Equity Takes Over
Private equity (PE) firms pool cash from individual investors to buy businesses from which they hope to extract greater profits or reorganize to sell pieces of the business at a profit. These firms often borrow heavily to fund acquisitions. And, as noted, PE firms have gotten deeply involved in the nursing home industry.
But it’s difficult to see exactly how PE takeovers of nursing homes affect their operations and finances because the new owners are, well, private. But a 2017 research paper — likely the very first in-depth academic case study of a private equity deal in this industry — sheds some light on the consequences, both positive and negative.
In 2006, the PE firm Fillmore Capital acquired Beverly Enterprises, a publicly traded operator of more than 300 nursing homes and assisted living facilities in 21 states. Along with renaming the company Golden Living, here are some of the changes the new owners made, according to coauthors Aline Bos and Charlene Harrington, a University of California, San Francisco, professor emerita who has studied nursing homes for decades:
- Split the company into an operating company, Golden Horizons, and a real estate firm, Geary Property Holdings.
- Further split Golden Horizons into Golden Living, owner of the nursing home chain, and Golden Ventures, a provider of administrative services.
- Divided the nursing home chain into individual limited liability companies for each of the properties.
- Launched a pharmacy services company, AlixaRx, with Golden Living as its initial customer. “AlixaRx will be wildly profitable,” said Ronald Silva, then and now the CEO of San Francisco-based Fillmore Capital Partners and chairman of Golden Living’s parent company.
- Significantly reduced per-resident staffing hours to lower-than-industry levels in its California nursing homes, cutting hours for licensed practical nurses and nursing assistants. Subsequent staff increases didn’t keep pace with national trends.
- Increased the amount of local managers’ compensation based on “financial performance and clinical excellence” rather than base pay. “They can almost double their salary,” said Neil Kurtz, M.D., Golden Living’s CEO at the time.
To its credit, the researchers found, Golden Living increased staffing hours for registered nurses, boosted employee training and benefits, and accelerated investments in information and communication technology. But, the researchers wrote, “the private equity-owned company did not improve quality of care.”
After the takeover, Golden Living faced numerous legal and regulatory actions in different states alleging problems with its facilities. In a 2015 lawsuit, for instance, the Pennsylvania attorney general alleged understaffing and failure to provide basic services to residents, and said state inspectors were deceived at 25 of the company’s 36 Pennsylvania facilities.
“We’re a mission-driven, social investing firm and we tried to change post-acute care by purchasing Beverly,” said CEO Silva in an interview this fall. “But I failed to do what I set out to do in many respects. The Golden Living board made a decision — because of various pressures on the nursing home sector and reputational issues — that other providers could do a better job providing care than we could.”
So 10 years after its acquisition, the company in 2016 started getting out of directly operating the homes, Silva said, leasing them to local and regional “tenant operators.” Golden Living now leases its nearly 200 remaining nursing home properties to 22 different operators in 12 states, while continuing to provide pharmacy and therapy services to some of the facilities through its subsidiary companies. It also provides clinical consulting services.
But Golden Living’s facilities continued to face financial and quality problems after shifting their management to others. Skyline Healthcare, a New Jersey-based operator to which Golden Living leased 60 of its facilities, was forced by regulators in four different states to give up management because of failure to pay staff and vendors, among other problems. At one Kansas facility, a vendor that hadn’t been paid reportedly stopped delivering food, so staff had to buy bread for the nursing home residents out of petty cash. Golden Living has since sold most of the former Skyline facilities and retains only 20 of them, with different operators in place, Silva said.
“I put total blame on Golden Living for not doing due diligence on whom they were leasing dozens of nursing homes to,” said Stephen Monroe, managing editor of “SeniorCare Investor” and a partner at Irving Levin Associates, which tracks private equity deals. “That was one of the more stupid transactions I’ve seen in the nursing home industry. Ron Silva was desperate to get out of the operating business and pushed hard to get out, but they bet on the wrong horse.”
Asked recently to update her assessment of Golden Living and other private equity owners, Harrington, the coauthor of the study about the nursing home purchase, responded, “I wouldn’t say Golden Living is worse; they’re all bad.” She added: “They’re investing to make money and aren’t producing adequate quality. That’s the bottom line.”
Editor’s note: An earlier version of this article incorrectly stated that Neil Kurtz was still CEO of Golden Living.
NEXT: What 2 Very Different Nursing Homes Learned From Fighting COVID-19

































































More From AARP