Staying Fit
Difficulty breathing, hospitals at capacity, social distancing and a world racing to create a vaccine conjure up memories of what life was like back in the 1950s for polio survivor Shirley Griffin.
"COVID is comparable, in my opinion, with polio because we really don't know anything about it,” says Griffin, 78. “It was a very scary time because you weren't supposed to get in a swimming pool or even be around anybody."


AARP Membership— $12 for your first year when you sign up for Automatic Renewal
Get instant access to members-only products and hundreds of discounts, a free second membership, and a subscription to AARP the Magazine.
Griffin was 9 years old when she was diagnosed, along with her brother, who was 11, in 1951, four years before the first polio vaccine became available. Since the local hospitals near her home in Lufkin, Texas, were full, the siblings had to recover at home. Alcohol rubs and ice were used to treat fevers that Griffin was told reached 105 degrees.
"The pains began in the legs,” she recalls. “The pain was unbelievable. And when you watch your mother rub your legs for hours with the tears coming down her cheeks, it's a little difficult to take.”
What is polio?
Poliomyelitis, or polio for short, is a potentially life-threatening viral disease. Most people who get infected with the poliovirus (about 70 percent) will not show any signs, according to the Centers for Disease Control and Prevention (CDC). About a quarter display flulike symptoms. A small portion of those infected, however, develop more serious complications, such as paresthesia (feeling of pins and needles in the legs), meningitis (an infection of the lining of the brain and/or spinal cord), weakness in the limbs or paralysis.
The polio virus is highly contagious. It's spread from person to person primarily through contact with feces of the infected and less commonly through respiratory droplets from a sneeze or cough.

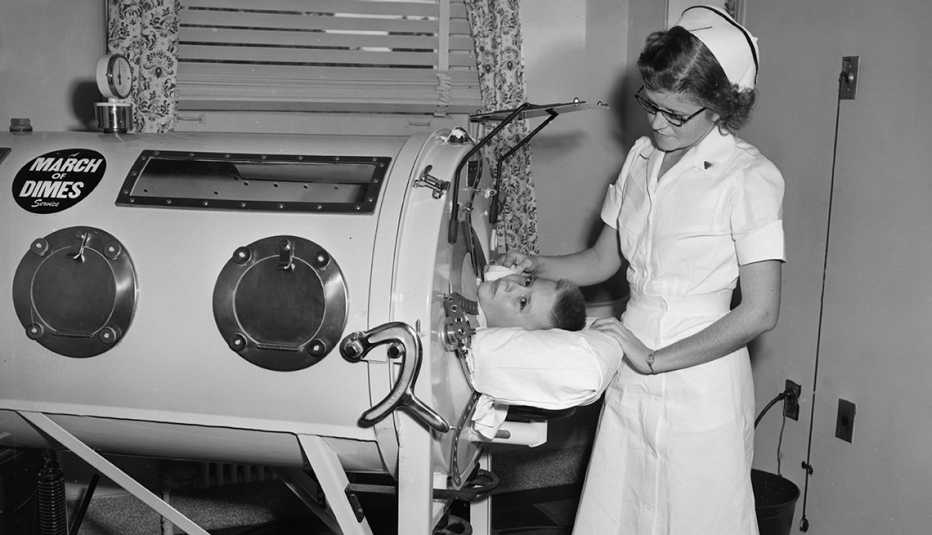
In the early 1950s, when Griffin was infected, outbreaks crippled over 15,000 people in the U.S. annually, according to the CDC. In patients without paralysis, treatment included complete bed rest, isolation and careful observation. For those who were weak or unable to move on their own, others would move their limbs, to prevent the patients from developing deformities. Tank respirators, or “iron lungs,” would assist those whose paralysis left them unable to breathe. These large cylinders encased the patient's entire body (except for the head) and used air pressure to force breathing.
Quarantines, handwashing were common
Avoiding contact with others remains a distinct memory for Griffin. When she was stricken, the family's minister would come to the front door and say a prayer every day. Then, when it was time for a checkup, the doctor would observe the siblings from the entryway, wearing the protective gear of the time.



































































