Staying Fit


After you enroll in Medicare, you need to think about your prescription drug coverage.
Medicare doesn’t automatically cover prescription drugs. Unless you have other comparable drug coverage — from an employer, a former employer or Tricare — you’ll need to sign up for coverage within a certain time. If you miss your deadline, you’ll have to pay a late enrollment penalty.


AARP Membership— $12 for your first year when you sign up for Automatic Renewal
Get instant access to members-only products and hundreds of discounts, a free second membership, and a subscription to AARP the Magazine.
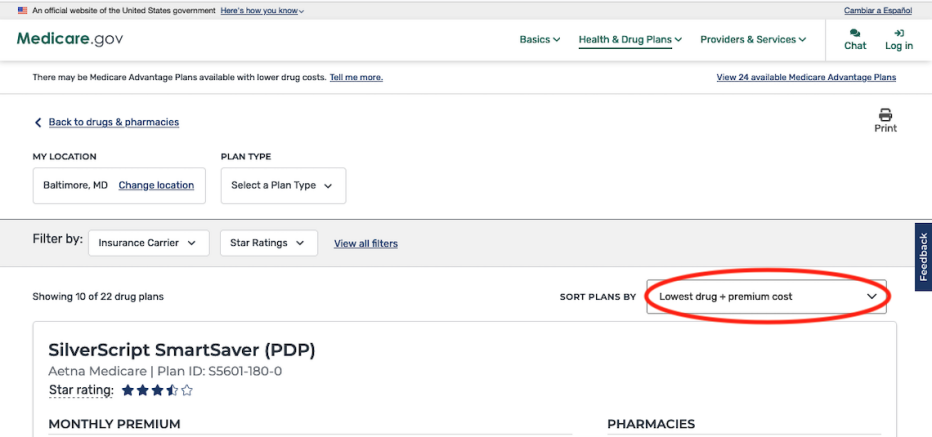
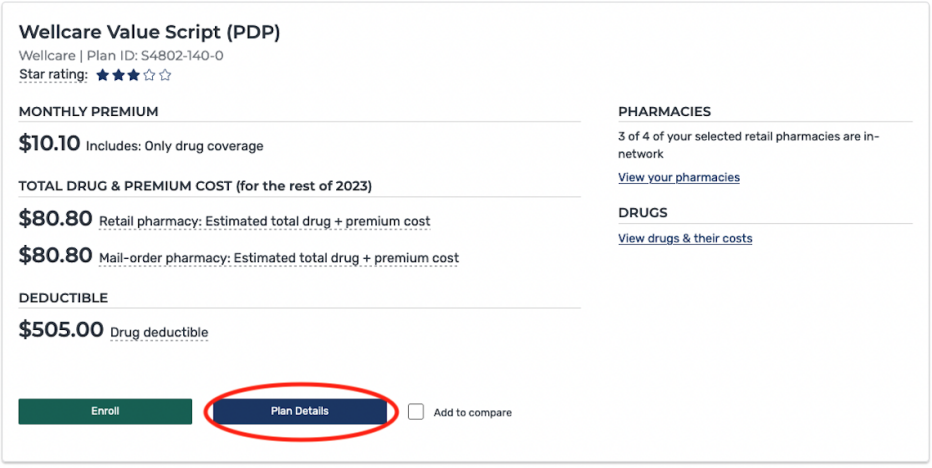
The average Medicare beneficiary has 24 stand-alone Medicare Part D plans to choose from. When choosing a Part D plan, look at premiums as well as coverage for your prescriptions. A plan with low premiums may cost you more by the end of the year if it charges high copayments for your medications.
But Part D plans can change their costs and covered drugs annually. So it’s a good idea to compare your options during open enrollment every year, which runs Oct. 15 to Dec. 7 for new coverage starting Jan. 1.
7 steps to sign up for a Part D plan
The best way to compare Part D plans offered in your area is to use Medicare’s Plan Finder tool. Here’s a step-by-step guide.
One caveat: If you take insulin, call 800-MEDICARE (800-633-4227) or contact your State Health Insurance Assistance Program (SHIP) rather than using the Plan Finder for 2023. A new law that capped insulin copays at $35 per month was signed after the premiums and copays were loaded into the Plan Finder, and this tool may not have the most up-to-date information about the plans’ insulin costs.
1. You have two options: Use your account or Continue without logging in. Either log in to your Online Medicare account or go to the second section and enter your zip code. It may also ask you to select your county. Hit Continue | Medicare Drug Plan Part D | Find Plans.

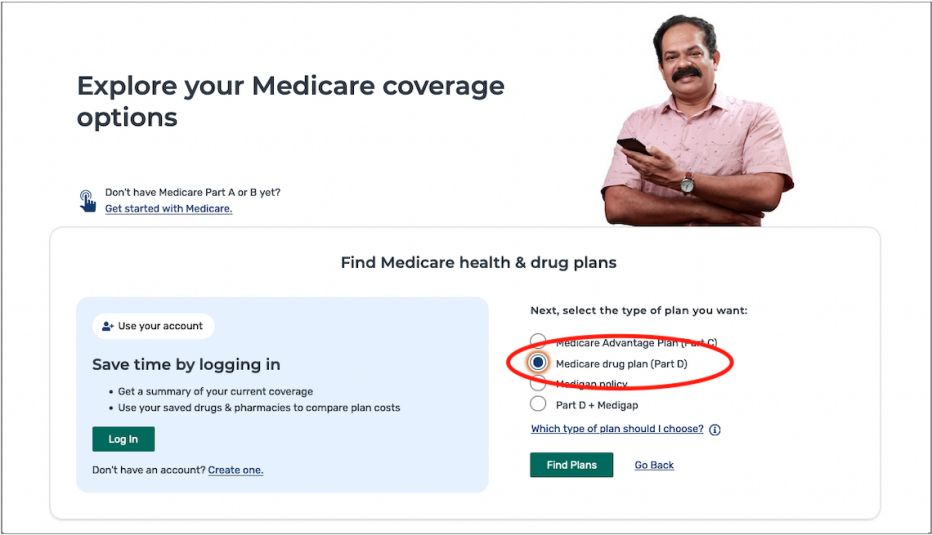
2. Indicate if you get help with your medical expenses. If you’re not sure, you can find out by logging into your Medicare account.
3. If you don’t receive help, you’ll be asked if you want to see your drug costs when you compare plans. Click Yes so you can get a sense of how much you would spend with each plan.
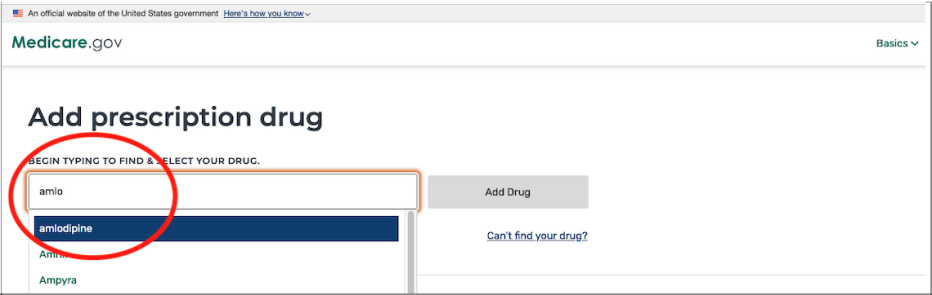
4. Enter the names of your medications. Be sure to include ones you take regularly so you’ll get a good estimate of ongoing costs.
You’ll also need to select the dosage and quantity, and indicate how frequently you need to refill your prescriptions. To add another medication, click Add Another Drug. When you’re finished, click Done Adding Drugs.


































































More on Health
When 9 Biggest Medicare Changes Under New Rx Law Go Into Effect
A year-by-year implementation timeline of the Inflation Reduction Act’s health provisionsHow Much Does Medicare Cost?
Monthly premiums, other out-of-pocket expenses can add up
Understanding Medicare’s Options: Parts A, B, C and D
Making sense of the alphabet soup of health care choices