Staying Fit
A piece of legislation enacted to help breast cancer patients qualify for Medicaid benefits has become a source of frustration for health care workers and a South Carolina man who has been diagnosed with the disease.

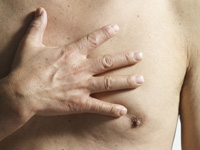
Raymond Johnson, 26, of Cross, S.C., learned about his breast cancer in July. Shortly after his diagnosis, he applied for insurance coverage through the Breast and Cervical Cancer Prevention Act of 2000. His request for coverage was denied, mostly because he is male.
Under the act, a patient must be under age 54, screened for breast cancer through a national early detection program, and uninsured and not eligible for Medicaid. The patient must also be female.


AARP Membership— $12 for your first year when you sign up for Automatic Renewal
Get instant access to members-only products and hundreds of discounts, a free second membership, and a subscription to AARP the Magazine.
"There is a tremendous amount of interest in this story because I think people realize how ridiculous it is that someone would take such an overly rigid interpretation of the rule," says Jeff Stensland, communications director for the South Carolina Department of Health and Human Services.
In search of help
Johnson, a single, childless construction worker, does not have medical insurance through his employer, Stensland says. The state of South Carolina has tried to find ways to cover his care and several organizations have joined the cause.
One of those is Roper St. Francis Healthcare, a nonprofit hospital where Johnson is currently receiving chemotherapy.
"We are pleased this story is raising awareness about male breast cancer risks and the burden of affordable care for the uninsured," says Scott Broome, director of oncology services at RSFH.
The hospital has been coordinating care with the Charleston Cancer Center, where Johnson first went for treatment.

































































More From AARP
Podiatrist Swindles $1 Million From Medicare
He even billed for services on a double amputee.
New Medicare Voucher Plan Draws Fire
Democrats argue voucher plan would end Medicare as we know it.