Staying Fit
Rachel Nania,
From the time she was 15, Anne Halli-Tierney knew she wanted to be a geriatrician — and it's all thanks to her grandfather, who she said “became a human being” after seeing one.
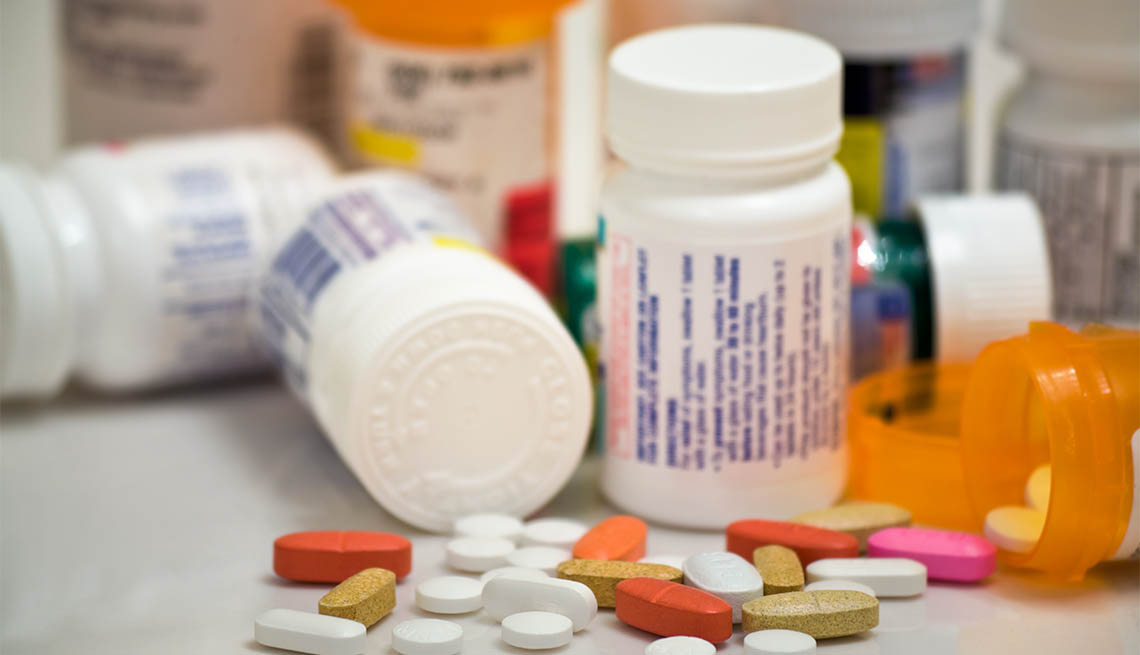
At one point, Halli-Tierney says her grandfather was taking more than 20 prescription medications a day to manage his chronic illnesses. However, after a few visits to the geriatrician — a doctor who specializes in the treatment needs of older patients — that list got whittled down to eight.


AARP Membership— $12 for your first year when you sign up for Automatic Renewal
Get instant access to members-only products and hundreds of discounts, a free second membership, and a subscription to AARP the Magazine.
"He had much more energy, his quality of life went up a great deal, and I think it was because he was literally overmedicated. They just basically made his medication list efficient,” says Halli-Tierney, a geriatrician and assistant professor of medicine at the University of Alabama. “And I was, like, ‘Oh, I want to grow up and do that. ’ “
Fast-forward several years, and Halli-Tierney says polypharmacy — a term used to describe the concurrent use of several medications, typically five or more — is still common, especially among adults who see more than one doctor to manage multiple chronic conditions.
Some researchers estimate nearly half of adults between the ages of 70 and 79 take at least five prescription drugs, and an additional 10 to 20 percent take 10 or more medications. And polypharmacy is becoming more common: Several studies have found that its prevalence has increased in recent years, especially among older adults.
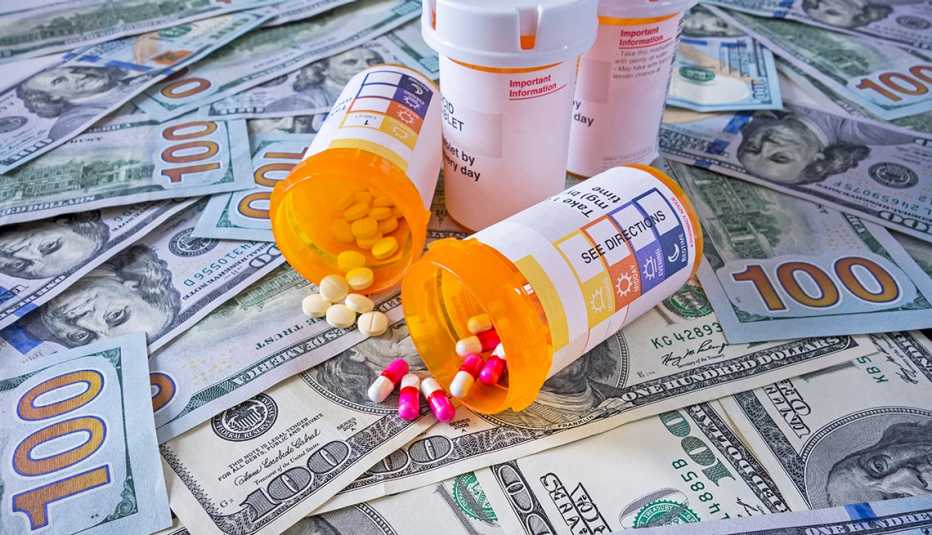
Experts point to several drivers behind the trend, including the growing chronic disease crisis, coupled with television ads that drive patient interest.
Medications are also safer than ever, and this may play a role in the rise of polypharmacy, says Simon Haroutounian, an associate professor of anesthesiology at Washington University School of Medicine in St. Louis and author of Preventing Medication Errors at Home.